Contact Information and Acknowledgments
2
Contact Information
Dr. Jennifer Lapum, PhD, RN, Professor, Associate Director of Quality Assurance, Daphne Cockwell School of Nursing, Toronto Metropolitan University (formerly Ryerson University), Toronto, ON., Canada, jlapum@ryerson.ca, @7024thpatient
Michelle Hughes, MEd, BScN, RN, Professor, School of Community and Health Studies, Centennial College, Toronto, Ontario, Canada, MHughes@centennialcollege.ca, @hughes0311
Acknowledgments
Instructional design consultant: Nada Savicevic, MA Interactive Design, MArch, BSc (Eng), Instructional Designer, Office of e-Learning, Toronto Metropolitan University, Toronto, Canada
Biology consultant: Charlotte Youngson, PhD, Department of Chemistry and Biology, Toronto Metropolitan University, Toronto, Canada
Copyeditor, Linn Clark Research and Editing Services, Toronto Canada
Pressbooks consultant: Sally Wilson, Web Services Librarian, Toronto Metropolitan University, Toronto, Canada
Accessibility consultant: Adam Chaboryk, IT Accessbility Specialist, Toronto Metropolitan University, Toronto, Canada
Copyright consultant: Ann Ludbrook, Copyright and Scholarly Engagement, Librarian, Toronto Metropolitan University, Toronto, Canada
Thank you to Centennial College Health Studies Lab Team for supporting this project and sharing their lab space to film the assessment videos.
Artist / Illustrators
Arina Bogdan, BScN, RN (chapter 3-5 images, and cover art)
Pelageya Grebneva, Ryerson, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada (chapter 3-5 images)
Levar Bailey (chapter 2 figure)
Student Advisory Committee
Christina Amirkhanian, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Samin Barakati, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Caitlyn Healey, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Mehak Khawaja, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Tommy Lin, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Maruel Isaac Sanchez, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Conner Sorley, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Lauren Sweeney, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Gabriel Umrao, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Steven Zagada, Toronto Metropolitan, Centennial, George Brown Collaborative Nursing Degree Program, Toronto, Ontario, Canada
Chapter 1 - Introduction to Health Assessment
I
By Dr. Jennifer Lapum, Michelle Hughes, Dr. Oona St-Amant, Dr. Lisa Seto Nielsen, Mahidhar Pemasani, and Riddore Creer
- Understand the role of health assessment.
- Apply the cognitive steps of clinical judgment.
- Understand approaches to health assessment.
- Recognize the role health promotion plays in health assessment.
Introduction to Health Assessment
2
Health assessment is the first phase of the nursing process and involves the collection and analysis of client data. Although it is the first phase, it is an ongoing process. Data collected as part of the health assessment process can be categorized as subjective and objective data. See Table 1.1 for an overview and examples of subjective and objective data.
Table 1.1: Overview and examples of subjective and objective data – adapted from Lapum et al., https://ecampusontario.pressbooks.pub/healthassessment/
|
Data
|
Example
|
|
Subjective
Information that a client or another person (i.e., family, caregiver) shares with the nurse spontaneously or in response to questions.
|
- A client says, “I have had a rash on my ankle and leg for the last two weeks.”
- A parent says, “My eight-month-old son is having trouble breathing.”
- A client’s reason for seeking care is “diarrhea for 10 days.”
- A client types, “I feel sick to my stomach.”
|
|
Objective
Information that the nurse observes when conducting a physical examination, and collecting lab and diagnostic results.
|
- The nurse observes that a client has a bright red rash on the dorsal side of the foot, the lateral malleolus, and anterior and lateral side of the lower leg.
- The nurse observes the client sitting upright, leaning forward, breathing fast with eyes wide open.
- The nurse measures the client’s blood pressure and records it as 112/84 mm Hg and pulse of 84 beats per minute.
- Lab test results: potassium (K+) 4.0 mmol/L, fasting glucose 4.8 mmol/L.
- Chest X-ray report: lungs well inflated and clear. No evidence of pneumonia or pulmonary edema.
|
Subjective data can include information about both symptoms and signs. Symptoms are something that the client feels (e.g., nausea, pain, fatigue). The nurse will not know about a symptom unless the client shares this information. Signs are observable, such as a rash, bruising, or skin perspiration. Signs can be categorized as subjective or objective because the client may tell you about their rash, and you as the nurse may also observe the rash. As reflected in Figure 1.1, a symptom is noted in the image on the left as “I’m having pain” while a sign can be observed in the image on the right, which is the bruising on the left arm.

Figure 1.1: Symptoms and signs
(Attribution: Taken from https://ecampusontario.pressbooks.pub/healthassessment/)
Age ranges are important to consider when determining normal and abnormal findings during health assessment. Depending on the source, these ranges can vary. Unless specified, we use the following terms and estimates in this resource:
- Newborns and neonates: newborns are birth to a few hours old and neonate is up to 28 days.
- Young children: clients who are 5 years and younger, including infants (28 days to 1 year), toddlers (1–2 years), and preschoolers (3–5 years).
- Older children and adolescents: clients who are 6–17 years, including older children/school-age children (6–12 years) and adolescents (13–17 years).
- Adults and older adults: clients who are 18 years and older, including adults (18 years and older) and older adults (65 years and older).
Activity: Check Your Understanding
Drag and drop all of the different items under the correct heading.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=69#h5p-1
Health Assessment: Related Legislation
3
Any health assessment you perform must fall within your nursing scope of practice and be informed by the appropriate nursing College or association practice standards. In Ontario, the College of Nurses of Ontario (CNO) is the legal governing body for nurses, so as a nurse, you must perform health assessment within the CNO legislated scope of practice, the practice standards, and also based on your individual level of competence (i.e., knowledge and expert practice to perform an action).
It is important to be aware of controlled acts, which are activities that are considered harmful if performed by someone who is unqualified as per the Regulated Health Professions Act (RHPA) (CNO, 2020a). As per the RHPA, a controlled act must only be performed with an order or when permitted by specific regulations and you must be competent to perform the skill/procedure (CNO, 2020a). For example, it is within your scope of practice to perform health assessments that move “below the dermis or mucous membrane” or involve putting your finger/hands or an instrument beyond “the external ear canal,” regions where the nasal passages narrow, the larynx, urethra, labia majora, anal verge, or “into an artificial opening in the body” as long as there is an order from a physician AND you are competent to perform this skill/procedure (CNO, 2020a).
As a nursing student, you are not yet a registered nurse. Therefore, with guidance from your supervisor/preceptor/clinical instructor, you must assess your competence to perform the controlled act and do so safely. If the decision is that you do not have the knowledge and skill to perform the controlled act, you may observe and use this as a learning opportunity.
Keep in mind that many controlled acts are related to interventions (e.g., treatment procedures) that you perform as a nurse, and some controlled acts relate to assessment techniques (e.g., performing an invasive technique).
When you perform an assessment, it is important to inform the client what you are assessing and typically share some of the findings that are within your scope of practice (e.g., I noticed inflammation around your ear drum). However, you are not permitted to communicate a diagnosis about what is causing the inflammation around the ear drum. Communicating a diagnosis is not permitted because this is considered a controlled act and outside of the registered nursing specific controlled acts (CNO, 2020b). Communicating a diagnosis is done by certain regulated health professionals such as a physician or nurse practitioner. However, you may be expected to communicate a diagnosis if you are delegated to do so by a physician or nurse practitioner and you have the knowledge to do so.
In performing any health assessment, you are also required to adhere to the CNO practice standards. Common practice standards that apply to health assessment include information related to consent and permission to touch, privacy and confidentiality, therapeutic nurse-client relationship, and documentation. Many of these CNO documents are based on health laws. It is important to recall that nurses are legally obligated to document their health assessment findings as per the CNO Documentation practice standard, as shown in Documentation in Nursing: 1st Canadian edition.
References
College of Nurses of Ontario (2020a). Legislation and regulation: An introduction to the Nursing Act, 1991. https://www.cno.org/globalassets/docs/prac/41064_fsnursingact.pdf
College of Nurses of Ontario (2020b). Legislation and regulation RHPA: Scope of practice, controlled acts model. https://www.cno.org/globalassets/docs/policy/41052_rhpascope.pdf
Clinical Judgment and Nursing
4
When collecting subjective and objective data, you need to consider clinical judgment. In nursing, the purpose of health assessment is to facilitate clinical judgment, which is defined as:
- A determination about a client’s health and illness status.
- Their health concerns and needs.
- The capacity to engage in their own care.
AND
- The decision to intervene/act or not – and if action is required, what action (Tanner, 2006).
The nursing process is the foundation of clinical judgment. However, clinical judgment is more comprehensive, action-oriented, and guided by the philosophy of client safety. Thus, it is important to learn when to act to prevent clinical deterioration, a worsening clinical state related to physiological decompensation (Padilla & Mayo, 2017).
To facilitate clinical judgment, you must determine if the collected data represent normal findings or abnormal findings. When findings are abnormal, you must act on these cues as they signal a potential concern and require action. Failing to recognize abnormal findings and act on these cues can lead to negative consequences including sub-optimal health and wellness – and more importantly, clinical deterioration. Some abnormal findings are considered critical findingsthat place the client at further risk if the nurse does not act immediately.
The process leading to clinical judgment is described as clinical reasoning. This process involves:
- Thoughtfully considering all client data as a whole, whether each piece of information is relevant or irrelevant, and how each piece of information is related or not related.
- Recognizing and analyzing cues. Is the information collected a normal, abnormal, or critical finding? Can the information be clustered to inform your clinical judgment?
- Interpreting problems. What is the priority problem and what are the factors causing it? What else do you need to assess to validate or invalidate your interpretation? What other information do you need to collect to make an accurate clinical judgment?
- Determining, implementing, and then evaluating appropriate actions (Dickison et al., 2019; Tanner, 2006).
The clinical reasoning process is encompassed by critical thinking. This means that when engaging in the process of clinical reasoning, you should systematically analyze your own thinking so that the outcomes are clear, rational, creative, and objective with limited risk of judgment and error.
A client tells you “I have a headache.” As the nurse, you immediately recognize the cue: headache. However, you do not have sufficient information to analyze this cue and identify the significance. Thus, you may ask a series of subjective questions such as “When did the headache start? What were you doing when it started? Have you ever had this type of headache before?” The client’s response will provide you detailed information to facilitate your critical thinking and the process of hypothesizing what is going on, and thereby helping you determine what actions to take.
Clinical judgement is facilitated by cognitive steps that help you determine when and how to act to prevent clinical deterioration; see Table 1.2. Like the nursing process, these steps should be performed in an iterative manner as per the client situation and your clinical reasoning process.
Table 1.2: Clinical judgment steps (developed based on NCSBN, 2020)
|
Steps
|
Considerations
|
|
Recognize cues
|
Recognizing cues involves identifying findings that require action because they are abnormal. This involves what Tanner (2006) calls “noticing” (i.e., recognizing when something is abnormal). You should be asking yourself what matters most?
|
|
Analyze cues
|
Analyzing cues involves interpreting/making sense of the collected data, what it means, and how it may relate to possible pathophysiological processes. This involves what Tanner (2006) calls “interpreting”, making sense of the collected data.
|
|
Prioritize hypotheses
|
Prioritizing hypotheses involves figuring out where to start and how to prioritize care. This step involves what Tanner (2006) refers to as “responding” to the collected data
|
|
Generate solutions
|
Generating solutions involves identifying the various options (e.g., actions/interventions) to address the problem or the abnormal findings/cues. This may involve identifying which solutions are indicated/effective, nonessential, unrelated, contraindicated.
|
|
Take actions
|
Taking actions involves identifying the action that should be taken. Examples of actions are specific but could be related to notifying the physician or nurse practitioner, calling for help, monitoring the client, collecting further data.
|
|
Evaluate outcomes
|
Evaluating outcomes involves determining if the action taken was effective. It may include identifying outcomes that are considered improved, unchanged, or worsened.
|
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=131#h5p-6
References
Dickison, P., Haerling, K., & Lasater, K. (2019). Integrating the National Council of State Boards of Nursing Clinical Judgment Model into nursing educational frameworks. Journal of Nursing Education, 58(2), 72-78. https://doi.org/10.3928/01484834-20190122-03
NCSBN (2020, Spring). Next Generation NCLEX news. https://www.ncsbn.org/NGN_Spring20_Eng_02.pdf
Padilla, R., & Mayo, A. (2017). Clinical deterioration: A concept analysis. Journal of Clinical Nursing, 27, 1360-1368. https://doi.org/10.1111/jocn.14238
Tanner, C. (2006). Thinking like a nurse: A research-based model of clinical judgment in nursing. Journal of Nursing Education, 45(6), 204-211. https://doi.org/10.3928/01484834-20060601-04
Why is clinical judgment important? How does it guide the provision of care?
Clinical judgment is important to ensure the nurse’s actions are based on the client’s most important needs. Clients often have several needs, and some are more important than others. As such, nurses need to assess and evaluate the priorities of care: what actions are most important to take first, and then what actions can follow. Typically, priority actions are those that prevent clinical deterioration and death.
Maslow’s Hierarchy of Needs
Priorities of care can be determined using several frameworks such as Maslow’s Hierarchy of Needs. For example, at the most basic level, life requires an open airway to breathe, the physiological process of breathing, and the circulation of blood and oxygen throughout the body. Airway, breathing, and circulation are the ABCs, which you might have learned if you have taken a cardiopulmonary resuscitation (CPR) course.
Maslow’s Hierarchy of Needs was developed to consider basic human needs and motivations of healthy individuals (Bouzenita & Wood Boulanouar, 2016; Francis & Kritsonsis, 2006; Gambrel & Cianci, 2003). Although not well known, Maslow’s work was closely influenced by the Blackfoot tribe in Canada (James & Lunday, 2014). One version includes five levels of needs: those related to physiological, safety, love, esteem, and self-actualization (Maslow, 1943), which can help prioritize care in nursing. Figure 1.2 presents one adapted version of Maslow’s Hierarchy.
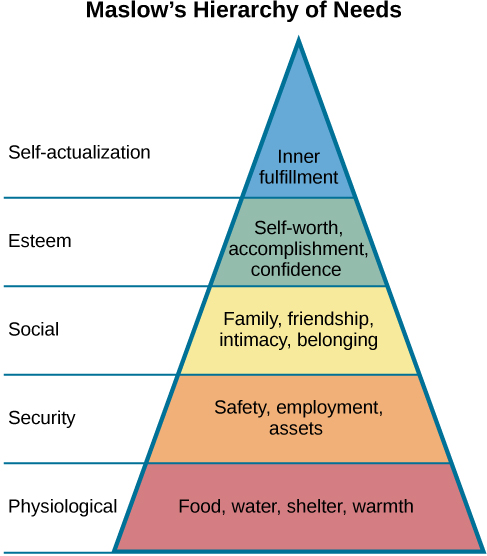
Figure 1.2: Maslow’s Hierarchy of Needs (see attribution statement at bottom of page)
Drawing upon this framework, a nurse can use health assessments to explore five levels of needs:
- Physiological needs – fundamental physical needs required for survival such as air, food/drink, sleep, warmth/clothing/shelter.
- Are these basic physiological needs being met? Is the client’s breathing and circulation supported?
- Safety – needs related to a secure physical and emotional environment.
- Does the client feel safe and secure in general in life? Does the client feel safe and secure in the healthcare environment? Is the bed lowered to the lowest position when you finish your assessment? Is the call bell in reach?
- Love and belongingness – needs related to relationships including friendship and family, intimacy and affection, work, and trust and acceptance.
- Does the client feel love and belongingness in general in their relationships? More specifically, does the client feel cared for by nurses and other healthcare providers?
- Esteem – feelings related to self-worth, dignity, respect, and achievement.
- Does the client feel respected and valued in general by others? Does the client feel respected and valued within the healthcare environment?
- Self-actualization – a process or action of reaching one’s full potential and self-fulfillment.
- What is important to the client in terms of what they want to achieve in life in general? What are the client’s goals that they may have for themselves in their own health and healing journey? Does the client feel satisfied, confident, and accomplished?
You can use Maslow’s Hierarchy of Needs as a guide, but it is important to be aware of the critiques and possible limitations in its application. See Video 1.1 of a conversation between Dr. Lisa Seto Nielsen and Mahidhar Pemasani.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=133#oembed-3
Video 1.1: A discussion about Maslow’s Hierarchy of Needs
Criticisms of Maslow’s hierarchy are related to it being ethnocentric, based on individualistic societies, and not necessarily taking into account diversity in culture, gender, and age (Bouzenita & Wood Boulanouar, 2016; Francis & Kritsonsis, 2006; Gambrel & Cianci, 2003). It should not be arbitrarily applied to all healthcare encounters. Although you may initially focus on physiological needs to ensure the client is stable, the client may have different priorities that are more important to them. By drawing upon Indigenous knowledge, it is vital to recognize the role of community and advocacy in reaching self actualization at every level (Bennett & Shangreaux, 2005). This is particularly important in the context of systemic racism and oppression and the existing disparities among racialized populations including Black communities and Indigenous People.
Levels of Priority of Care
Because of the importance of recognizing clinical deterioration in a client, a nurse must always be attuned to the set of physiological needs that are important to maintain life and prevent death. These priorities of care are related to the ABCs – airway, breathing, and circulation – introduced above. These priorities of care are often categorized as first, second, or third level, with the first level taking a priority (see Table 1.3).
Table 1.3: Priorities of care
|
Priority of care
|
Examples
|
|
First-level priority of care are problems/issues that reflect critical findings, clinical deterioration and/or are life-threatening – and therefore require urgent action. Urgent means that action must be taken immediately.
|
A client in respiratory distress as evident by tachypnea, nasal flaring, laboured breathing, intercostal retractions, and decreasing oxygen levels or a client with hemodynamic instability such as chest pain or the absence of or decreasing pulse or blood pressure.
|
|
Second-level priority of care are problems/issues that may lead to clinical deterioration and may become life-threatening without intervention – and therefore require prompt action. Prompt means that action must be taken quickly.
|
A client with signs and symptoms such as: altered level of orientation, decreased level of consciousness/confusion, elevated temperature, increasing pain levels, and cold extremities. This may include a client with a head injury who can deteriorate quickly in some cases. You should assess if they experienced a loss of consciousness and have any associated symptoms with a concussion.
|
|
Third-level priority of care are problems and issues that are typically focused on functional health, client education, and counselling. These should be addressed, but they are non-urgent and can wait until the client is stable. The problem/issue is not acute in nature, but intervention is required to support the client’s activities of daily living, their knowledge level, and their mental health and wellbeing
|
A client who is post-operative and requires assistance with hygiene and mobility, a client who reports increasing stress levels and problems sleeping, or a client who is newly diagnosed with diabetes and requires education around nutrition and monitoring their blood glucose levels.
|
With regard to levels of care, it is essential to consider what is most important to the client. You should treat the client as the expert in their own life – and also as the expert in decisions about their own healthcare, if they choose. Although a client may have plummeting blood pressure, you need to consider tailoring the intervening action to their wishes. Some clients may not wish for intervention in a life-threatening circumstance. Therefore, you always need to be open to the client’s wishes, but also consider whether they are able to weigh the consequences of their decision (i.e., are they competent to consent?).
In practice, mental health is typically not categorized as a first- or second-level priority of care unless the client is showing signs of clinical deterioration based on the examples noted in Table 1.3. In some situations, mental health may be positioned as a third-level priority of care, for example when a client is experiencing anxiety, depression, grief, but shows no signs of suicidal ideation. These symptoms should be addressed, but according to this framework, they are considered less urgent compared to first- and second-level priorities of care. However, sometimes, you should think differently about how mental health is a priority of care.
In some situations, mental health may take precedence. For example, a client who has attempted suicide or has just overdosed will probably have other physical symptoms as a result and therefore require urgent intervention and constant observation as per Table 1.3. However, the descriptions of the priorities of care presented in the table do not account for a client who has voiced a specific plan for suicide and has identified when and how. This client is at very high risk and requires urgent intervention regardless of what may be viewed as their physical health state or history. The description of priorities of care listed above does not account for this except as a third-level priority – but a client with suicide ideation or has voiced wanting to hurt others requires urgent action to protect their own wellbeing and others and the possibility of clinical deterioration as a result of their actions.
Intervention Types
As illustrated by the text box above, you will need to use your own judgement to determine how to act when a cue presents itself and how to categorize these interventions. This could involve four general types of interventions that you need to be aware of (see Table 1.4) including effective, ineffective, unrelated, and contraindicated. These types of interventions will become more clear as you begin to learn about normal, abnormal, and critical findings for various body systems, and how interventions and actions will affect these findings and the client.
Table 1.4: Types of interventions
|
Type of Intervention
|
Example
The client has no pulse, their chest is not rising, and they are not responsive. As a nurse you need to make a clinical judgment on how to act based on these cues.
|
|
Effective (or indicated) interventions are actions that are adequate to produce the intended result and help the client.
|
Begin CPR immediately. This is also an evidence-informed intervention because a delayed response results in poor outcomes as per the research.
|
|
Ineffective interventions are actions that are not adequate to produce the intended result and therefore will not help the client.
|
Provide mouth-to-mouth resuscitation; without compressions, the oxygen will not circulate.
|
|
Unrelated (or non-essential) interventions are actions that will not produce an effect (positive or negative) and therefore will not help the client.
|
Notify the client’s employer.
|
|
Contraindicated interventions are actions that are not recommended because they have the potential to cause harm to the client.
|
A contraindicated intervention is to delay resuscitation until a physician is present.
|
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=133#h5p-7
Attribution statement for Figure 1.2
Authors: Spielman et al. Publisher/website: OpenStax Book title: Psychology 2e. Publication date: Apr 22, 2020 Location: Houston, Texas. Book URL: https://openstax.org/books/psychology-2e/pages/1-introduction Section URL: https://openstax.org/books/psychology-2e/pages/1-2-history-of-psychology. Textbook content produced by OpenStax is licensed under a Creative Commons Attribution License 4.0 license.
References
Bennett, M., & Shangreaux, C. (2005). Applying Maslow’s Hierarchy Theory. First Peoples Child & Family Review: a Journal of Innovation and Best Practices in Aboriginal Child Welfare Administration, Research, Policy & Practice, 2(1)89-116. https://doi.org/10.7202/1069540ar
Bouzenita, A. I. & Wood Boulanouar, A. (2016). Maslow’s hierarchy of needs: An Islamic critique. Intellectual Discourse, 24(1), 59-81.
Francis, N.H. & Kritsonis, W.A. (2006). A brief analysis of Abraham Maslow’s original writing of self-actualizing people: A study of psychological health. Doctoral Forum: National Journal of Publishing and Mentoring Doctoral Student Research, 3(1), 1-7.
Gambrel, P., & Cianci, R. (2003). Maslow’s hierarchy of needs: Does it apply in a collectivist culture. The Journal of Applied Management and Entrepreneurship, 8(2), 143–161.
James, A., & Lunday, T (2014). Native birthrights and Indigenous science. Reclaiming Children and Youth, 22(4), 56-58.
Maslow, A. (1943). A theory of human motivation. Psychological Review, 50(4), 370-396. https://doi.org/10.1037/h0054346
Guiding Approaches of Health Assessment
6
The guiding approaches of health assessment refer to specific conventions of when and what type of health assessment to perform. For example, how often should you perform an assessment on the client? What type of assessment should you perform and how comprehensive should it be? Approaches always depend on the context of the situation. As you become more experienced, you will also be able to pick up on cues that require additional assessment.
Health Assessment Frequency
The frequency of a health assessment is determined by the setting (e.g., primary care, long term care, acute care) and the health and clinical status of the client.
- The frequency of a primary care visit depends on the client’s age and their health status and needs. For example, guidelines have been established for the frequency of well-baby and childhood visits and maternal health visits. Also, clients with complex healthcare needs (such as multiple morbidities) will need to see their primary care practitioner more often than a healthy adult.
- The frequency of assessment in a long-term care setting is often determined by concerns voiced by the client, the personal support worker (PSW), or the registered practical nurse (RPN). PSW and RPN typically have more 1:1 contact with clients in long-term care settings and will draw the registered nurse’s attention to concerns that may require further assessment.
- The frequency of assessment in acute care (such as medical or surgical units) will be at least every four hours. In critical care, this frequency is increased to usually every 1–2 hours at least. Clients in critical care are usually on a monitor in which their heart rhythm and vital signs such as oxygen saturation and heart rate are constantly monitored and alarm bells will signal if there is an abnormal change. Although there may be a standard for the frequency of assessment based on the unique population you care for or the institution policy, you must be aware that escalation of care and increased frequency may be needed based on the nurse’s assessment and the client’s clinical status. For example, at times clients may require constant observation (e.g., post-surgery, in critical care environments, a client who is unstable or may show signs of deterioration, or a client in mental health distress with suicide ideation or post-attempt).
Health Assessment Types
There are several ways to describe health assessment types. In this chapter, we refer to four types including: primary survey; focused assessment; head-to-toe (abbreviated version); and complete health assessment. As per Table 5.1, the type of health assessment to be performed is determined based on the context of the situation.
Table 1.5: Types of health assessment
|
Type of Assessment
|
Recommendations
|
|
Primary survey
Airway (patency)
Breathing (respiratory rate, work of breathing, oxygen saturation)
Circulation (pulse rate/rhythm, BP, urine output)
Disability (level of consciousness, speech, pain)
Exposure (temperature, skin integrity, pressure injuries, wounds, dressings, drains, lines, ability to transfer/mobilise, bowel movements)
(Douglas et al., 2016)
|
According to current recommendations, all assessments should begin with a primary survey because this structured assessment helps nurses recognize and act on signs of clinical deterioration (Considine & Currey, 2014) that are correlated with death (Douglas et al., 2016). A primary survey collects data in order of importance, and it is aligned with most institutions’ rapid response systems (Considine & Currey, 2014).
This recommendation marks a change from the tradition of beginning an assessment with vital sign measurement (Considine & Currey, 2014) or doing a head-to-toe assessment. A primary survey will help you determine if urgent intervention is needed or whether you should perform a focused assessment or a head-to-toe assessment.
This change in assessment practice is still relatively new. Thus, you may encounter healthcare professionals who are not familiar with this shift in practice and the primary survey. It can provide an opportunity for discussion and learning.
|
|
Focused assessment
An assessment that is specific to a health concern/reason for seeking care.
|
This type of assessment is performed in all areas of care (e.g., primary care, emergency, long-term care, medical, surgical). Because of its specificity, it usually involves a focus on a limited number of body systems based on the health concern, similar to an episodic database.
For example, a client’s reason for seeking care may be an “achy knee.” Thus, the nurse’s assessment will be focused on the musculoskeletal system. Another example may be chest pain. Because there are multiple causes of chest pain, you may need to do a cardiac, respiratory, and musculoskeletal assessment. Another example is a follow-up assessment: a client may have been prescribed a new medication for high blood pressure and needs a follow-up assessment a couple of weeks later to determine the effects.
|
|
Head-to-toe assessment (abbreviated)
A head-to-toe assessment follows a cephalocaudal approach, assessing several body systems, and provides an overview of the client’s current health status.
|
Typically, a head-to-toe assessment should take about 10 minutes and should be performed at the beginning of your shift and when you first interact with a client. There are variations of this assessment based on the client situation, reason for seeking care, and institution/unit.
A head-to-toe assessment usually includes attention to overall wellbeing/needs, pain, vital signs, specific assessments related to neurological, cardiovascular, peripheral vascular, skin, respiratory, gastrointestinal, genitourinary, activity/rest, and wounds/dressings, IV sites, drains/tubes, and oxygen.
Based on the collected data, this type of assessment may influence the need for a more focused examination of a specific body system. For example, you may notice the client has a bloated and hard abdomen. Based on these cues, you should complete an abdominal assessment.
A more complete assessment/head-to-toe may be needed in certain situations when a comprehensive assessment is warranted (see next section on complete health assessment).
|
|
Complete health assessment
A complete health assessment is similar to a head-to-toe assessment, but it is more comprehensive. It involves a subjective and objective assessment of all body systems. It provides a full overview of the client’s current health status.
|
A complete health assessment may take 30–60 minutes depending on the client and the complexity of their health issues. It may be performed for several reasons, often when clients have complex care needs. It is often performed upon admission to a long-term care home or rehabilitation, and sometimes in a primary care setting with new clients. It may also be performed in acute settings when a client has complex health problems and diagnoses have been problematic.
This kind of assessment can vary based on the client situation, developmental stage, reason for seeking care, and institution/unit.
|
When you are new to a work environment, you should inquire about the typical conventions surrounding assessment frequency and type. It is also always helpful to ask your clinical instructor/preceptor about their approach to assessment.
When conducting these assessments, it is important to assess the client’s level of consciousness and level of orientation. New onset disorientation and/or a decrease in level of consciousness are important cues that could indicate clinical deterioration and thus, require immediate intervention. If not yet completed, a primary survey should be done and findings shared with the physician or nurse practitioner.
Level of consciousness is the client’s state of awareness and response to stimuli (voice/sound or physical). Their level of consciousness is described as:
- Alert and oriented: This means that the client is awake (or easily arouses to your voice), engages appropriately in interactions with you, responds appropriately to your questions, and oriented to person, place, time, and self.
- Confused and disoriented: This means that the client shows altered cognition such as difficulty in memory retention, difficulty following commands, uncertain about the environment around them, inattention, and shows signs of disorientation in terms of person, place, time, and self. They may have delayed or inappropriate/incorrect responses to your questions.
- Lethargic: This means that the client is slow/sluggish to arouse to stimuli. For example, you need to say their name loudly or multiple times or physical shake their arm. They are sleepy, lack energy, slow to respond to your questions, but answers appropriately and are oriented.
- Obtunded: This means that the client has a significant impairment in their level of consciousness and requires a significant and continuous stimuli (loud voice, vigorous shaking of the arm). They have difficulty to respond because of the impairment, need constant coaxing to respond, can only answer very simple questions with one word responses that are difficult to hear and understand. Without stimuli, they will immediately return to sleep.
- Unconsciousness: This means that the client does not respond to any stimuli and has no purposeful motor responses.
Level of orientation is assessed by asking the client questions related to:
- Place (questions to ask: Do you know where you are? They may know they are in a hospital because of the room. Thus, you may probe with the question, do you know what hospital you are in?).
- Time (questions to ask: Do you know what date it is? Do you know what day of the week it is? Do you know what month it is? Do you know what year it is?).
- Person (question to ask: Do you know who I am? They may say “yes”, but you should probe with the question, can you tell me who I am? They may be able to identify you as a nurse, but forget your name in some cases).
- Self (question to ask: Do you know who you are? If they respond “yes”, you should probe with the question, can you tell me your name?).
A normal response is that the client is oriented to place, time, person and self. If they are disoriented, you indicate what they are disoriented to. You may indicate oriented to place, person and self, disoriented to time. It is important to consider context when assessing level of orientation. For example, a client may not be aware of the specific date, but knows the day of the week or month.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=135#h5p-8
References
Considine, J., & Currey, J. (2014). Ensuring a proactive, evidence-based, patient safety approach to patient assessment. Journal of Clinical Nursing, 24, 300-307. https://doi.org/10.1111/jocn.12641
Douglas, C., Booker, C., Fox, R., Windsor, C., Osborne, S., & Gardner, G. (2016). Nursing physical assessment for patient safety in general wards: Reaching consensus in core skills. Journal of Clinical Nursing, 25, 1890-1900. https://doi.org/10.1111/jocn.13201
The Ottawa Charter for Health Promotion from the 1980s remains relevant, but in the 1990s there was a shift to a more expansive understanding of health determinants. See Table 1.6 for some examples of health determinants.
Table 1.6: Health determinants. (adapted from the Canadian Public Health Association, 1996).
|
Health determinants
|
Considerations
|
|
Healthy child development.
|
Assessment of healthy child development focuses on the physical, cognitive, and emotional development of the child and whether their needs are being met and developmental milestones are being reached.
|
|
Lifelong learning.
|
This type of learning involves the personal and professional pursuit of knowledge. It can involve developing job skills and improving employability, and thus socioeconomic stability. It may also inspire personal development and foster a continual pursuit of knowledge even into older adulthood
|
|
Absence of racism and discrimination associated with culture, gender, and sexual orientation.
|
Discrimination and racism can negatively affect a person’s health and wellbeing. Therefore, you should assess for the presence of these in a client’s life and how it affects them.
|
|
A life free of violence.
|
A life free of violence positively influences health and wellbeing. It is important to be aware of the negative effects of violence on a person’s life and how you can screen and assess for it.
|
|
Work opportunities and adequate income.
|
Access to work opportunities supports an individual’s development over the course of their life and also provides access to adequate income. Limited access to these opportunities can have negative effects on health and wellbeing.
|
|
Healthy lifestyles (nutrition, activity/exercise, sleep/rest, coping and stress management, and smoke free).
|
A range of lifestyle factors can negatively affect health and wellbeing and lead to certain disease processes. Inquiring about these factors is part of many assessments.
|
|
Healthy, social relationships.
|
Healthy, social relationships are positive health determinants throughout all life stages. These can include parenting relationships, friends, work, and intimate partner relationships: all of these can support development and quality of life.
|
|
Protection from infectious diseases and environmental hazards.
|
Living in an environment free from and/or protected from infectious diseases and environmental hazards is important to overall health and wellbeing.
|
References
Canadian Public Health Association (1996). Action statement for health promotion in Canada. https://www.cpha.ca/action-statement-health-promotion-canada
Integrative Approach to Health Promotion and Assessment
12
As a nurse conducting a health assessment, you have an obligation not only to document and respond to the data you yield through your health assessment, but also to offer guidance to your clients. An integrative, individualized, and adapted approach to health promotion means that you partner with clients to identify their needs. You may apply all three approaches – behavioural, relational, and structural – to health promotion. For example, some situations may call for a behavioural approach: perhaps the client is seeking strategies to reduce their cholesterol. Other occasions may call for a relational approach, such as working with a family experiencing a loss; still others may require a structural approach, such as helping a client complete application forms to cover their medication costs.
All of the health promotion approaches and strategies rely on the nurse’s assessment skills and their capacity to prioritize what is important to the client, their family and community in that particular moment. Although health determinants remain relevant, Gewurtz et al. (2016) also proposed approaching health promotion by focusing on “the integration of physical, mental, social and spiritual components of health and well-being. … [within the context of the person’s] patterns of daily activity” (p. e205).
This marks a change from the traditional prescriptive nature of past approaches, which neglected to truly engage the client as an expert in their own lives – it also includes considering the client’s daily patterns of activity that should be the driving force of health promotion interventions. An effective and integrated health promotion approach that is shaped by the client’s daily patterns of activity, will require that you understand the person’s day-to-day life and what is important to them.
Therefore, when collaboratively developing a health promotion intervention with a client, your assessment should include questions like:
- Tell me about your day-to-day activities.
- What does a typical day look like for you?
- Who is involved in these activities with you?
- Have you had any recent changes in your day-to-day activities in the past year?
- In order to be a healthier you, how would you like these day-to-day activities to be different?
Table 1.7 presents an adapted example based on Gewurtz et al.’s (2016) health promotion approach: it is based on patterns of activity. This example is informed by clinical judgment, which requires identifying health-related cues and the identifying of actions to promote a client’s health and wellbeing. As with all interventions, you should engage the client in identifying what is important to them in terms of their health and wellbeing.
Table 1.7: Example of health promotion
|
Client description
|
Clinical judgement
|
Health promotion
|
|
An international student has moved to a large city to attend their first year of university. They had a close group of friends and family in the small town they grew up in, and now feels lonely. Their day-to-day activities used to be much fuller and they used to feel engaged, and now they just go to class and study.
|
The nurse recognizes the cues of missing a social group. The student’s activity patterns have been disrupted, leading to loneliness and disengagement. To further analyze these cues, the nurse should explore what other activities the student used to do where they grew up and what activities they may enjoy here.
|
Health promotion interventions should be collaboratively co-created with the student based on their needs and wants. Interventions might include connecting with their old social circle via social media/video-conference, and also developing new patterns of social activities at the university, for example by joining extra-curricular groups.
|
A focus on health promotion is important in all healthcare settings including primary care settings and hospital/acute care settings. Although health promotion is categorized as a third-level priority of care, you should integrate knowledge of health determinants into all assessments. A focus on health promotion can help promote client engagement and overall health and wellbeing while reducing negative effects.
References
Gewurtz, R., Moll, S., Letts, L., Lariviere, N., Levasseur, M., & Krupa, T. (2016). What you do every day matters: A new direction for health promotion. Canadian Journal of Public Health, 106(2), e205-e208. https://doi.org/10.17269/CJPH.107.5317
Clinical Judgement Activity
13
Read the following case study and begin to work through the clinical judgement activity as the case unfolds.
A 20-year-old client was brought into the emergency room (ER) by their roommate with abnormal vital signs. The client had a rapid heartbeat of 160 beats per minute, chest pain, shortness of breath with elevated respiration rate of 32 breaths per minute that are shallow and rapid. The client arrived at the ER sweating, shaking, stating they feel nauseous, chills, lightheaded, tingling sensation in their fingers, and as if they are going to faint. The paramedics were unable to get an O2 saturation reading due to the client’s hands shaking and said the last blood pressure (BP) was elevated at 150/92 mmHg. The client’s friend is frantic in the waiting room and calling the client’s parents.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=400#h5p-10
After the healthcare team provided treatment and asked the client a series of health history questions, they concluded the client had a panic attack. After 20 minutes, the client’s vital signs began to stabilize: heart rate 100 beats per minute, respiration rate 22 breaths per minute, BP 130/82, and O2 rate of 96%. The client shared they had been experiencing a lot of stress at school because their midterm exams are next week. The client hasn’t been sleeping, had been drinking a lot of coffee to stay up to study, and had just broke up with their partner. The client stated they had never had a panic attack before, but that their mother used to have them when she was younger.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=400#h5p-11
Generating solutions involves identifying the various options (actions and interventions) to address the abnormal findings/cues. This may involve identifying which solutions are indicated, unrelated, or contraindicated.
Drag the following actions and interventions in the appropriate category before Checking your answer.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=400#h5p-12
Health promotion is an integral element of health assessment and focuses on promoting the agency of the client.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=400#h5p-13
- Health assessment involves collecting subjective and objective data and must be performed within a nurse’s scope of practice.
- Clinical judgment is an important component of health assessment resulting in the decision whether or not to act/intervene, and if action is required, what action.
- Prioritizing care in nursing is informed by Maslow’s Hierarchy of Needs, as well as priorities of care (first, second, or third), and should also consider the client’s wishes.
- Guiding approaches to health assessment include types of assessment such as primary survey, focused assessment, abbreviated head-to-toe assessment, and a complete health assessment.
- Health promotion is an integral element of health assessment informed by behavioural, relational, and structural approaches.
Chapter 2 - Inclusive Approaches to Health Assessment
II
By Dr. Annette Bailey, Dr. Oona St-Amant, Dr. Erin Ziegler, Dr. Lisa Seto Nielsen, Nada Savicevic, Paul Petrie, Evan Accettola, Mahidhar Pemasani, Alexis Andrew, Riddore Creer, Michelle Hughes, and Dr. Jennifer Lapum
French translation version available: https://pressbooks.library.torontomu.ca/evaluationinfirmiere/#main
- Describe the concept of inclusive health assessment.
- Define key principles of inclusive health assessment.
- Outline an anti-oppressive approach to inclusive health assessment.
A health assessment is a “felt” experience for clients.
Pause for a moment and put yourself in a client’s shoes. Imagine seeking care and having the nurse diminish your feelings, make you feel unimportant, and exclude you from the care process. How would this make you feel? Probably disrespected, disengaged, and that you don’t matter – maybe even silenced.
Now, imagine the alternative: the nurse values your feelings, perspectives, experiences, and considers what is important to you. How would you feel? Probably included, respected, and engaged.
The difference here is between health assessments that are exclusive/oppressive versus inclusive/liberating.
Learning to conduct a health assessment is an important part of nursing education and practice. Health assessments help nurses understand the health needs of each client and set priorities for their care. Acquiring this understanding requires:
- objective knowledge, which is obtained through assessment techniques and skills.
- subjective knowledge, which is obtained through empathetic, relational, and interactional skills.
During a health assessment, you will need to communicate and engage critically and empathetically with each unique client to understand how to care for them in relevant and holistic ways.
We are all different, and our illness experiences are informed by, and are as unique as, our social experiences, so you cannot apply a one-size-fits-all care plan. Individual health assessments are important to help you understand each client and tailor a unique plan for them. You will need to embrace all aspects of the client’s humanity and be mindful and attentive to any personal and unconscious biases that may negatively influence your views and interactions with them – this is what is meant by an inclusive health assessment.
Safe nursing practice requires an inclusive approach to health assessment. Nurses are expected to protect the physical and psychological safety of clients. If clients have experienced trauma in the past, they may have psychological and physiological reactions (Cohen et al., 2006) that affect how they engage with health professionals and health interventions. It is especially important to protect the psychological safety of clients who have experienced racial or social trauma, or any type of trauma for that matter. The ongoing global social justice movement has brought to light how experiences with systemic oppression – especially discrimination and racism – lead to socioeconomic disparities that eventually have devastating impacts on health. You must consider this reality during any health assessment.
Unfortunately, the healthcare system is not free of discriminatory and exclusionary practices, and as a result, this can make clients feel unsafe. Black, Indigenous, and LGBTQI2SA+ (Lesbian, gay, bisexual, transgender, queer, intersex, Two-spirit and asexual) populations continue to experience inequitable care and access disparities, which can lead to distrust of healthcare providers, including nurses.
A health assessment is one of the first points of contact between nurse and client. It can be a critical step where a nurse starts to address the experiences of, and repair the harm done to, these groups and others through assessment approaches that uplift, not oppress. For some time, nurses and other healthcare professionals have been encouraged to consider the cultural experiences of clients. However, it is important to transcend the usual emphasis on culture awareness: you should also include anti-oppressive, humanistic practices in health assessments.
This chapter explores what it means to be inclusive during a health assessment, in terms of intent and process.
Reference
Cohen, J. A., Mannarino, A. P., & Deblinger, E. (2006). Treating trauma and traumatic grief in children and adolescents. The Guilford Press.
What is an Inclusive Assessment?
To answer this question, let us first locate its relevance in the context of social justice.
Human existence is defined by differences: different people, experiences, cultures, and perspectives. Social justice is most commonly defined as fairness in terms of opportunities, regardless of differences.
Social injustice is rooted in differences and has led to terrible human suffering in our society. These injustices are the greatest point of weakness for humanity and come in many forms including:
- Racism (e.g., anti-Black, anti-Asian, anti-Indigenous racism)
- Inequality (e.g., sex, gender, racial inequality)
- Ageism
- Ableism
Social injustice can lead to social paralysis for some groups in society because of differential access to resources and opportunities, marginalization, exclusion, and discrimination. Social paralysis is a state of social stagnation imposed by inequity and injustice that hinders social and economic progress of groups in society.
Social injustice can also fuel what is known as “othering discourse” – discourse that promotes an “us” versus “them” mentality (Inokuchi & Nozaki, 2005). This can make marginalized groups feel unworthy and lead to powerlessness, fear, stress, trauma, and vulnerability to illnesses. From a health perspective, extreme manifestations of social injustice can include illnesses such as cancer, heart disease, diabetes, and respiratory disease. For example, researchers have demonstrated that structural injustices related to racism are the root cause of disparities in the prevalence and control of diabetes, as well as diabetes-related deaths, among racial and ethnic minorities (Ogunwole & Golden, 2021)
Without understanding the social roots of illness, it can be easy to blame clients for their illness outcomes, or even to perpetuate injustice in how a client is treated, with differential practices of health assessments across clients. All clients need to feel that their health and their health needs matter – and that they matter. Health assessments should make clients feel safe, respected, and engaged. If they feel marginalized or feel that they are being excluded or treated differently, this can foster injustices in their health outcomes, and in the healthcare system more broadly.
Inclusive health assessments should be grounded in social justice. Nurses must uphold the humanity of all clients in all aspects of care, regardless of the client’s race, ethnicity, gender, sexuality, age, ability, and any other factor that makes them who they are.
Inclusive health assessments are based on four key principles:
- Treat every health assessment as an act of humanity. What does it mean to be treated like a human being? We all want to be accepted, respected, and feel a sense of belonging. If you make a client feel otherwise, you are engaging in an act of oppression, which can affect human dignity and capacity to grow and transform. It is important to recognize that even though nursing is a caring profession, nurses have the power to oppress. You must acknowledge differences among clients, while committing to dismantle social injustices within healthcare systems that render clients inhumane.
- Health assessments are not about sameness. Every client is different, so health assessments have to go beyond the “normal” or standardized approaches to physical assessment. “Normal” is a social construct: a common social idea based on cultural values and relative norms. You need to obtain a nuanced understanding of each client’s unique health and illness experiences and help them move towards a path of healing. A health assessment should be more than a physical assessment: talk with the client to obtain their health history and get to know them. An inclusive health assessment means that you recognize and integrate the client’s unique experiences and knowledge in their care.
- Examine your own personal biases. Everyone carries biases that are acquired through socialization. These may include biases about different races, cultural practices, body sizes, or religious practices. These biases can affect how you present yourself during a health assessment, and consequently how clients feel and respond in your presence. By learning about your own biases – how they developed and how they influence your actions – you can both understand how they lead to further injustices in nursing practice, and how you can start to unlearn them.
- Cultivate a safe environment of care. Create an environment where the focus is on what matters to the client. Approach each client with a “spirit of inquiry” (Registered Nurses’ Association of Ontario, 2007, p. 26). Keep an open mind as you learn about the client’s needs and perspectives: accept the client for who they are, value their feelings and experiences, and don’t judge them. A safe space is important for clients to express themselves without fear of being judged and discriminated against. Clients will engage more when they feel they are collaborating with the nurse on a common goal in terms of what is important to the client. Feeling safe promotes self-worth and a feeling of belonging, which are critical outcomes of social justice in the healthcare system.
Take a moment to test your own biases by taking the Harvard Implicit Association Test: https://implicit.harvard.edu/implicit/langchoice/canada.html When you go to this link, you can click on “Background” to learn more about the origins and purpose of this test or click on “Take a demo test” to test your biases.
The following diagram (Figure 2.1) shows how these key principles are inter-connected. You should incorporate all of them while engaging in an inclusive health assessment. As discussed above, social justice is central to inclusive health assessment, and is therefore located in the middle of the diagram. Importantly, as indicated, social justice is rooted in anti-oppressive perspectives, as discussed later in the chapter. The dotted line signifies the direct interaction between the practice of inclusive assessment in the healthcare system and its continuing impacts in communities.
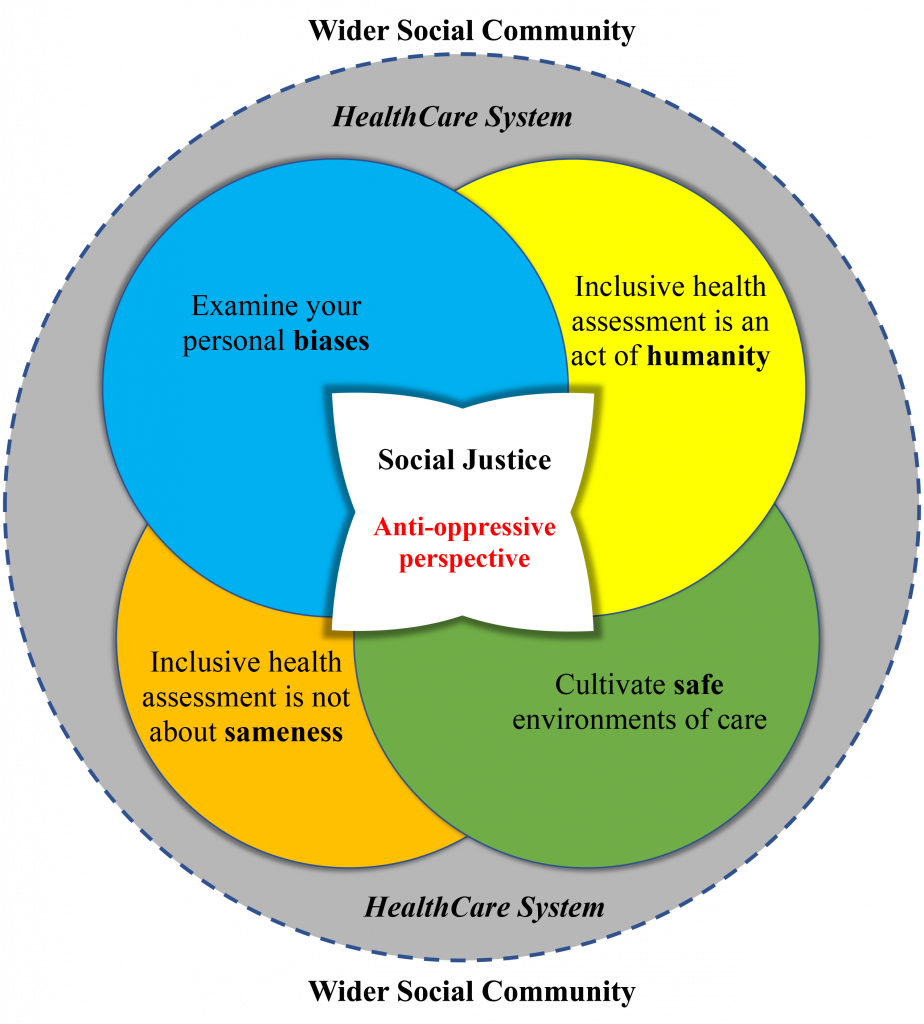
Figure 2.1: Principles of inclusive health assessments (illustrated by Levar Bailey)
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=546#h5p-38
References
Inokuchi, H., & Nozaki, Y. (2005). “Different than Us”: Othering Orientalism, and US middle school students’ discourse on Japan. Asia Pacific Journal of Education, 25(1), 61-74. https://doi.org/10.1080/02188790500032533
Ogunwole, S. M., & Golden, S. H. (2021). Social determinants of health and structural inequities—root causes of diabetes disparities. Diabetes Care, 44(1), 11-13. https://doi.org/10.2337/dci20-0060
Registered Nurses’ Association of Ontario (2007). Healthy work environments best practice guidelines: Professionalism in nursing. Registered Nurses’ Association of Ontario. https://rnao.ca/sites/rnao-ca/files/Professionalism_in_Nursing.pdf
Moving Beyond Culture in Health Assessment
As healthcare professionals, nurses have power. You have power.
If not applied carefully, this professional power can make clients feel marginalized or dismissed. In recent years, progressive developments in theoretical perspectives have guided nursing practice toward more humanistic care and considerations for marginalized clients and communities. New concepts have been introduced to help inform clinical judgement, honour the cultural values/beliefs of clients, and support therapeutic relationship building. These concepts include: cultural sensitivity, cultural competence, cultural humility, and cultural safety. They have helped clarify how personal biases can influence health assessments and other nursing interventions, and have also helped many nurses learn how to minimize their own biases.
Culture can be defined as the beliefs, practices, and values of a racial/ethnic group; it can also include other dimensions such as gender, sexual orientation, ability/disability, age, class, and language (Greene-Moton & Minkler, 2020; Hughes et al., 2019).
Reflect on each client’s culture:
- What are their cultural beliefs, values, and identity?
- What should you do once you are aware of a client’s culture and cultural differences?
- Most importantly, can this understanding of culture help you conduct an inclusive health assessment?
The following discussion explores these questions, beginning with an exploration of how four main concepts of culture relate to health assessments.
Cultural Sensitivity
- In nursing, cultural sensitivity focuses on self in terms of the nurse’s awareness and understanding of a client’s culture as well as attitude toward culture (Srivastava, 2007).
- Cultural sensitivity, therefore, largely rests on the nurse’s ability to be compassionate, considerate, and understanding of clients, including effective communication with clients from different cultures (Foronda, 2008).
Cultural Competency
- In the past, cultural competency has been narrowly operationalized as a checklist of cultural knowledge required by healthcare providers to demonstrate competence when working with various racial and ethnic groups (Curtis et al., 2019; Greene-Moton & Minkler, 2020).
- A nurse who is culturally competent is able to provide effective care to clients from different cultural backgrounds (Sharifi et al., 2019).
- However, if you do not know the cultural beliefs and practices of an ethnic group, does that make you culturally “incompetent”? This kind of ambiguity in the concept of cultural competency has led to the urgency of other effective frameworks for nurses to use, including cultural humility and cultural safety.
Cultural Humility
- Cultural humility is a life-long process of reflection and self-critique in addressing power imbalances within systems to develop mutually beneficial partnerships and relationships (Tervalon & Murray-Garcia, 1998).
- Healthcare professionals should engage in continuous, critical reflection on power and privilege, and find ways to interact with clients of different race, sex, gender, age, and ability that don’t perpetuate oppression.
Cultural Safety
- Cultural safety requires that nurses recognize power differentials and broader social structures that affect health equity (Curtis et al., 2019).
- Nurses must challenge power imbalances in client care, considering the effects of oppression on health (Parisa et al., 2016).
- Culturally safe practice is essential in addressing health and social disparities and inequities, to ensure equitable and client-centred care.
Integration of Concepts
Nurses can apply these four concepts of culture to understand cultural differences and embrace respectful ways of interacting with clients from different cultural backgrounds. This can be a starting point for broader considerations of historical, social, economic, and political factors that also shape health inequities (Smye & Browne, 2002).
Despite the large body of theoretical work on culture and safe practices, many healthcare professionals continue to be intolerant of differences. So, beyond an understanding of culture, what else is needed for nurses to uphold all the elements of social justice in nursing care broadly and in health assessments specifically?
The next section explores how you can apply an anti-oppressive perspective to ensure health assessments are inclusive. This involves confronting and dismantling oppressive practices that are accepted as the status quo in health assessments and the healthcare system more broadly, especially in the care of marginalized groups.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=548#h5p-39
References
Curtis, E., Jones, R., Tipene-Leach, D., Walker, C., Loring, B., Paine, S.-J., & Reid, P. (2019). Why cultural safety rather than cultural competency is required to achieve health equity: A literature review and recommended definition. International Journal for Equity in Health, 18(1), 174–174. https://doi.org/10.1186/s12939-019-1082-3
Foronda, C. L. (2008). A concept analysis of cultural sensitivity. Journal of Transcultural Nursing, 19(3), 207-212. http://doi.org/10.1177/1043659608317093
Greene-Moton, E., & Minkler, M. (2020). Cultural competence or cultural humility? Moving beyond the debate. Health Promotion Practice, 21(1), 142–145. https://doi.org/10.1177/1524839919884912
Hughes, V., Delva, S., Nkimbeng, M., Spaulding, E., Turkson-Ocran, R.-A., Cudjoe, J., Ford, A., Rushton, C., D’Aoust, R., & Han, H.-R. (2020). Not missing the opportunity: Strategies to promote cultural humility among future nursing faculty. Journal of Professional Nursing, 36(1), 28–33. https://doi.org/10.1016/j.profnurs.2019.06.005
Parisa, B., Reza, N., Afsaneh, R., & Sarieh, P. (2016). Cultural safety: An evolutionary concept analysis. Holistic Nursing Practice, 30(1), 33–38. https://doi.org/10.1097/HNP.0000000000000125
Sharifi, N., Adib-Hajbaghery, M., & Najafi, M. (2019). Cultural competence in nursing: A concept analysis. International Journal of Nursing Studies, 99. https://doi.org/10.1016/j.ijnurstu.2019.103386
Smye, V., & Browne, A. J. (2002). “Cultural safety” and the analysis of health policy affecting aboriginal people. Nurse Researcher, 9(3), 42–56. https://doi.org/10.7748/nr2002.04.9.3.42.c6188
Srivastava, R. (2007). The healthcare professional’s guide to clinical cultural competence. Mosby Elsevier.
Tervalon, M., & Murray-García, J. (1998). Cultural humility versus cultural competence: A critical distinction in defining physician training outcomes in multicultural education. Journal of Health Care for the Poor and Underserved, 9(2), 117–125. https://doi.org/10.1353/hpu.2010.0233
Moving Toward Anti-Oppression Perspectives in Health Assessments
Understanding anti-oppression first requires understanding what oppression is.
Oppression
Oppression can be defined as the unjustified use of power and privilege to stagnate others socially, politically, and psychologically. Oppression is imposed through demoralizing interactions, discriminatory and exclusive policies/practices, deprivations in access to resources, and publicly propagated stereotyping that create barriers to opportunities, growth, acceptance, and recognition for some groups in society (Banks & Stephens, 2018).
Oppression is often framed in opposition to privilege, which can be defined as the unearned, unobstructed access to resources, respect, acceptance, and opportunities awarded to others.
Both oppression and privilege are unscripted laws of society that, whether exercised knowingly and unknowingly, govern how we think about and interact with those considered “different.”
Oppression is both experienced and felt. Social oppression is structural, meaning it operates at all levels and systems in society, but it is experienced at the individual/group level in the form of powerlessness, trauma, feelings of unworthiness, and an indefensible struggle for recognition and acceptance. This struggle has yielded a legacy of resilience and resistance in Canada, especially among racialized and Indigenous populations, but the persistent navigation of structural barriers and personal biases has had consequences for these groups, including trauma and illness (Matheson et al., 2019).
Anti-Black racism rooted in slavery and anti-Indigenous racism rooted in colonization are known to be illness-inducing forms of oppression. Experiences of anti-Black and anti-Indigenous racism often translate to less educational and job opportunities, increased rates of incarceration, and more exposure to violence. Black and Indigenous children are more likely to be in the child welfare system (Matheson et al., 2019). These experiences increase the possibility of these individuals coming into contact with the healthcare system.
Anti-Oppression
As you engage with clients in the health and healing process, try to focus on restorative practices. Try to recognize and interrupt the negative consequences of discrimination, racism, colonization, and social injustice. As a nurse, you should operate from a position of cultural sensitivity, cultural competence, cultural humility, and cultural safety, with an overarching professional responsibility to anti-oppressive practices.
An anti-oppressive framework of practice is an all-encompassing commitment to social justice and the flourishing of human dignity.
When you apply an anti-oppressive perspective to a health assessment, you will be acutely aware of the many ways that health inequities can negatively transform the health of clients, their worldviews, and their responses and interactions. This kind of understanding will help ensure that you do not stagnate the client’s healing process, and prompt you to take action to confront discriminatory and exclusive practices within the healthcare system that might hinder the client’s access to equitable care.
Contextualizing Culture
For example, Black youth in Toronto are disproportionately affected by gun violence deaths and injuries. The social stigma of experiences with gun violence often has negative effects on the care they receive from healthcare providers (Khenti, 2018). When assessing a young Black man with an injury, a nurse who is aware of the concepts of culture will understand that race puts the client at risk for this type of injury. From an anti-oppressive perspective, the nurse further understands that racial inequities and social stigma associated with this type of injury may affect healthcare workers’ views and interactions with this young man and put him at risk for discriminatory care. Awareness of this possibility might prompt the nurse to obtain information needed to help advocate for health resources for the client, and also to support all members of the healthcare team in providing accessible and empathetic care.
As you conduct a health assessment from an anti-oppression perspective, you should consider how structural barriers and internalized powerlessness resulting from oppression can silence the voices of marginalized clients and prevent them from advocating for themselves in the healthcare system. Recognizing how to collaborate with these clients to advocate for health needs is an important part of an anti-oppressive approach to health assessments. Always be aware that feelings of disrespect and unworthiness are common consequences of social oppression, so it is critical that you remain professional and respectful to clients of diverse lived experiences in all interactions.
Activity: Check Your Understanding
References
Banks, K. H., & Stephens, J. (2018). Reframing internalized racial oppression and charting a way forward. Social Issues and Policy Review, 12(1), 91-111. https://doi.org/10.1111/sipr.12041
Khenti, A. A. (2018). Three decades of epidemic black gun homicide victimization in Toronto: Analyzing causes and consequences of criminological approach. (Doctoral dissertation). https://yorkspace.library.yorku.ca/xmlui/handle/10315/34979
Matheson, K., Foster, M. D., Bombay, A., McQuaid, R. J., & Anisman, H. (2019). Traumatic experiences, perceived discrimination, and psychological distress among members of various socially marginalized groups. Frontiers in Psychology, 10, 416. https://doi.org/10.3389/fpsyg.2019.00416
Practical Considerations and Application of Inclusive Health Assessment
In the next section, we focus on examples of clients from three populations (Indigenous, Black, and LGBTQI2SA+) to demonstrate key actions and considerations for inclusive assessments.
We chose these groups based on their historical and current experiences with intersecting oppressions and inequities that have impacted on their care in the healthcare system.
We recognize that humanistic nursing care goes beyond race, gender, and sexuality. Therefore, as you learn about these three cases, consider what inclusive assessment and anti-oppressive care might look like for other clients who might experience oppression: immigrant clients, elderly clients, or those with a disability, or other differences (related to religion and other forms of culture) that might lead to oppression.
Inclusive Health Assessments with Indigenous Clients
Case Application: Joyce Echaquan
Joyce Echaquan was a 37-year-old Indigenous woman who died in a Canadian hospital in September 2020. Before she died, she posted a Facebook Live video of a nurse and another healthcare worker demoralizing her with racist slurs, calling her stupid and saying, “she’d be better off dead” (CBC, 2021). https://www.cbc.ca/news/canada/montreal/joyce-echaquan-coroner-inquest-may-19-1.6032387
Take a moment to reflect on this. The healthcare workers did not interact with Joyce in a way that uplifted her humanity.
How might Joyce’s story have been different?
Here are a few strategies to consider when engaging in an inclusive assessment with Indigenous clients:
- Always try to understand the cultural experiences that affect their health. A nurse interacting with someone like Joyce should be aware that as an Indigenous woman, she may have experienced trauma from colonization, anti-Indigenous racism, and systemic oppression, all of which may have affected her health. The experiences of residential schools have inflicted trauma and abuse on Indigenous children and families, which have resulted in problems including addictions, violence, and suicide (Aguiar & Halseth, 2015; Bourassa et al., 2015). It is important to convey respect for Indigenous clients and their family and empathy for their positionality.
- When working with Indigenous people, you should recognize their trauma experiences. Ensure your interactions do not aggravate oppression and health disparities within the healthcare system. Healthcare providers have historically contributed to inequities for Indigenous people, and anti-Indigenous racism persists today in healthcare systems, which has perpetuated systemic discrimination and barriers in healthcare for Indigenous people (Richmond & Cook, 2016). As a result, many Indigenous individuals are distrustful of Canadian institutions including hospitals. Use inclusive and anti-racist communication: language should put clients at ease and promote belonging. Joyce’s case illustrates how treatment by healthcare workers reinforced social oppression and trauma, and stripped Joyce of her dignity before her death.
- Try to uphold their self-determination. Consider how historical and current policies affect all aspects of health and acknowledge the inherent right to self-determination among all clients (Richmond & Cook, 2016). Even if you lack this kind of knowledge, you can engage in assessments that uphold self-determination. Resist controlling or paternalistic approaches to care and instead prioritize the client’s right to make decisions for themselves. In this context, this means that you need to engage in active learning about:
- Systemic discrimination directed at Indigenous Peoples.
- The privileging of Western forms of knowledge within healthcare.
- Inter-generational trauma caused by historical events like residential schools.
- Reflect on your own bias and assumptions about Indigenous people. Reducing inequities in health care for Indigenous people requires being conscious of implicit biases that may affect your view of Indigenous people. Implicit bias toward Indigenous people has become normalized in the healthcare system, such that many are desensitized to it (Wylie & McConkey, 2019). Nurses must engage in critical self-reflection about how their own biases affect their professional practice and the health of their clients (Hughes et al., 2020). When applying an inclusive approach to health with an Indigenous client, you should share the space, listen, and attend to the needs expressed by the client.
References
Aguiar, W., & Halseth, R. (2015). Aboriginal Peoples and historic trauma: The process of intergenerational transmission. https://www.ccnsa-nccah.ca/docs/context/RPT-HistoricTrauma-IntergenTransmission-Aguiar-Halseth-EN.pdf
Bourassa, C., Blind, M., Dietrich, D., & Oleson, E. (2015). Understanding the intergenerational effects of colonization: Aboriginal women with neurological conditions—their reality and resilience. International Journal of Indigenous Health, 10(2), 3-20. https://doi.org/10.18357/ijih.102201515113
Hughes, V., Delva, S., Nkimbeng, M., Spaulding, E., Turkson-Ocran, R.-A., Cudjoe, J., Ford, A., Rushton, C., D’Aoust, R., & Han, H.-R. (2020). Not missing the opportunity: Strategies to promote cultural humility among future nursing faculty. Journal of Professional Nursing, 36(1), 28–33. https://doi.org/10.1016/j.profnurs.2019.06.005
Matheson, K., Foster, M. D., Bombay, A., McQuaid, R. J., & Anisman, H. (2019). Traumatic experiences, perceived discrimination, and psychological distress among members of various socially marginalized groups. Frontiers in Psychology, 10, 416. https://doi.org/10.3389/fpsyg.2019.00416
Wylie, L., & McConkey, S. (2019). Insiders’ insight: Discrimination against Indigenous Peoples through the eyes of health care professionals. Journal of Racial and Ethnic Health Disparities, 6(1), 37–45. https://doi.org/10.1007/s40615-018-0495-9
Richmond, C. A. M., & Cook, C. (2016). Creating conditions for Canadian Aboriginal health equity: The promise of healthy public policy. Public Health Reviews, 37(2), 1-16. https://doi.org/10.1186/s40985-016-0016-5
Inclusive Health Assessments with Black Clients
Case Application: Mireille Ndjomouo
Mireille Ndjomouo was a 44-year-old Black mother of three children who died in a Canadian hospital in March 2021. In a video she posted to social media before her death, she begged for help: “it’s as if they’re killing me little by little … I have children. I don’t want to die and leave my children.” She was begging to be moved from that hospital, stating that she had been treated with penicillin despite telling hospital staff she was allergic (World News, 2021). https://www.vice.com/en/article/pkdnpn/mireille-ndjomouo-posts-video-begging-for-help-in-quebec-hospital-days-before-she-died
Mireille was clearly feeling a sense of powerlessness; her voice and her own knowledge of her health needs were not respected.
How might Mireille’s story have been different?
Here are a few strategies to consider when engaging in an inclusive assessment with Black clients as offered by Dr. Nadia Prendergast, a nurse scholar who focuses on anti-Black racism research:
- Be mindful that experiences with racism in society and the healthcare system affect responses to healthcare professionals. The historical injustices of a 200-year tradition of slavery have caused multigenerational traumas that can make Black clients distrust individuals and interventions within healthcare systems (Kennedy et al., 2007). This distrust may lead them to perceive assessment questions as intrusive. Black clients’ historical experiences with the healthcare system may make them reluctant or abrupt in answering some questions. Some healthcare professionals may view this as aggression – you should avoid perceiving this reluctance as aggression. Instead, explain your reasons for asking the questions and reassure confidentiality. Gauge whether it is safe to ask about their previous experiences with the healthcare system, as this may be seen as interrogating. If the nurse had considered Mireille’s experiences with racism, outcomes might have been different. Try to break down any potential or apparent barriers with consistent acceptance, friendliness, genuine care, and patience.
- Be aware of your own assumptions about Blackness. Blacks share the common experience of oppression resulting from slavery and present-day racial injustices, but they are not a homogenous group. Media and common myths have led to false perceptions of Blackness, including the false idea that Black people do not feel pain because their nerve endings are different. For example, pain is the most disabling symptom of sickle cell disease, but physicians often deny pain medication to Black sickle cell disease clients, seeing them as drug seekers or drug addicted (Bergman & Diamond, 2013). A Black male youth presenting with pain and asking for morphine might be perceived and treated as a drug addict, when he is actually having a sickle cell crisis. This kind of incorrect assumption can lead to improper assessments and care, as with Mireille. Always invite Black clients to share their own knowledge. Being willing to learn from the client creates an equitable environment for healing. Culture is exercised and interpreted differently by everyone, so it is unrealistic for you to learn everything about other cultures; instead, try to come from a place of recognition, awareness, and desire to dismantle racism.
- Be attuned to your own biases about Black clients. Systemic oppression has worked to influence perceptions of Blacks as primitive and unintelligent (Smiley & Fakunle, 2016). Linked with this are biases around people who speak with an accent as being perceived as not intelligent or being less intelligent, as well as the use of gesticulations and loud voice volumes as being signs of mental health, violence, and uneducatedness. These biases can affect how you engage with Black clients – and even when not intentional, Black clients may interpret behaviours that are dismissive and judgemental as racism. Racism manifests in our biases about racialized people as lesser beings, and therefore, less deserving of the respect and human honouring that are important aspects of an inclusive assessment. Remember that racialized clients are also assessing you as the nurse. It is vital that you actively strive to be anti-racist as opposed to merely claiming that you are not racist. You must always be conscious of your own biases, and in this context, especially about Black intelligence. You should respect the knowledge that Black clients bring to health assessments. In Mireille’s case, her knowledge of her penicillin allergy was not respected.
References
Bergman, E. J., & Diamond, N. J. (2013). Sickle cell disease and the “difficult patient” conundrum. The American Journal of Bioethics, 13(4), 3–10. https://doi.org/10.1080/15265161.2013.767954
Kennedy, B. R., Mathis, C. C., & Woods, A. K. (2007). African Americans and their distrust of the health care system: healthcare for diverse populations. Journal of Cultural Diversity, 14(2).
Smiley, C., & Fakunle, D. (2016). From “brute” to “thug:” The demonization and criminalization of unarmed Black male victims in America. Journal of Human Behavior in the Social Environment, 26(3-4), 350-366. https://doi.org/10.1080/10911359.2015.1129256
Inclusive Health Assessments with LGBTQI2SA+
Case Application: Cody
Cody is a 16-year-old who identifies as a transgender male. He presents to the emergency department with anxiety. While at hospital, he experiences discrimination from hospital staff by being misgendered and not being called by his preferred name. In this virtual simulation game, you can see Cody’s interactions with the healthcare system. https://soginursing.ca/eresource/index.html#/lessons/rf4jDfaDQfwab1IIq3E6xF6zF-9o4jkT
LGBTQI2SA+ individuals have historically experienced stigmatization, discrimination, and marginalization in society and in accessing healthcare.
How might Cody’s story have been different?
Initial interactions during a health assessment can affect whether the client feels comfortable disclosing their sexuality and gender identity, and whether they will return for services (Bosse et al., 2015). When talking to clients about gender and sexuality, always avoid making assumptions.
It is important to have even a basic understanding of gender identity. Gender identity is one’s sense of their gender, often identified as male or female, and can be classified as cisgender or transgender: an individual who identifies as cisgender has a gender identity that aligns with their sex at birth, whereas an individual who identifies as transgender has a gender identity that is incongruent with their sex at birth (Bourns, 2019). Individuals who identify as non-binary may not identify as male or female, or they may identify with no gender, or as a gender other than male or female, or as more than one gender (James et al., 2016). Within the Indigenous population, those who identify as Two-Spirit may describe their gender, sexual, or spiritual identity as a person who embodies both a male and a female spirit (TransCare BC, 2017).
Sexuality refers to an individual’s experience and how they express themselves sexually. A person refers to their sexual orientation based on who they are sexually attracted to. Individuals who are attracted to the opposite gender identify as heterosexual, whereas those who are attracted to the same gender identity as homosexual. Individuals who are attracted to two genders may identify as bisexual (Rainbow Health of Ontario, 2020). Heteronormativity is the assumption that heterosexuality is the norm, which remains prevalent (Searle, 2019). It is critical to be aware of heteronormative assumptions during a health assessment.
Contextualizing Culture
For example, imagine you are doing a health assessment on an 18-year-old female with the identified pronouns she/her. If you are asking about her sexual activity and ask if she has a boyfriend, you have made a heteronormative assumption, which can have negative effects on trust and the nurse–client relationship. Instead, ask if she is sexually active, who she has sex with, and her sexual orientation.
Stigma, discrimination, homophobia, and transphobia have created social isolation and mental health challenges, including suicide risks, for LGBTQI2SA+ individuals. Therefore, it is important to ensure an inclusive and gender-affirming environment during each health assessment.
Here are a few strategies for fostering inclusive health assessments with LGBTQI2SA+ individuals:
- Before every interaction, reflect on the beliefs or assumptions that you have about LGBTQI2SA+ individuals and how these assumptions may conflict with the principles of inclusive health assessments
- When meeting a new client, introduce yourself with your name and pronoun and ask which name and pronoun they use. This normalizes gender identity and reduces stigma for transgender and gender non-conforming individuals.
- When doing an assessment, ask the client their preferred words for their body parts. Using the term genitals instead of vagina or penis can be important for transgender and non-binary individuals (Bosse et al., 2015).
References
Bosse, J., Nesteby, J., & Randall, C. (2015). Integrating sexual minority health issues into a health assessment class. Journal of Professional Nursing, 31, 498-507. http://doi.org/10.1016/j.profnurs.2015.04.007
Bourns, A. (2019). Guidelines for gender-affirming primary care with trans and non-binary patients. http://www.transforumquinte.ca/downloads/Guidelines-and-Protocols-for-Comprehensive-Primary-Care-for-Trans-Clients-2019.pdf
Rainbow Health Ontario (2020) LGBT2SQ terms and definitions glossary. https://www.rainbowhealthontario.ca/news-publications/glossary/
Searle, J. (2019). Queer phenomenology, the disruption of heteronormativity, and structurally responsive care. Advances in Nursing Science, 42(2), 109-122. https://doi.org/10.1097/ANS.0000000000000258
The Trans PULSE Canada Team (2020). Health and health care access for trans and non-binary people in Canada. https://transpulsecanada.ca/research-type/reports
Trans Care BC. (2017). Gender-affirming care for trans, Two-Spirit, and gender diverse patients in BC: A primary care toolkit. http://www.phsa.ca/transcarebc/Documents/HealthProf/Primary-Care-Toolkit.pdf
We hope that this chapter contributes to your advocacy work and inspires you to engage in confronting oppression by dismantling the systems that support it. You can begin by engaging with clients in health assessments that are respectful and recognize their humanity.
Power and privilege negatively affect the health of marginalized people. It is important to consider the effects of power structures at the individual level – think about illness and its roots. Consider how social oppression shapes the everyday struggles of marginalized groups. These individuals must struggle to overcome the effects of these forces: over time, a client’s resistance to intersecting levels of oppression can be internalized and affect their health. When interacting with clients in health assessments, try to make a deliberate attempt to dismantle oppressive structures.
Honour the knowledge of the client you are caring for. Your clients have knowledge of themselves, their being, and their experiences. This knowledge is important. If we as healthcare providers frame ourselves as the knower of all people, we are assessing and delivering care from a position of power: we are missing out on what it means to do an inclusive and individualized health assessment. You should embrace the knowledge clients have of their own bodies and minds. Clients also do their own assessment of nurses – they assess how well you tap into their knowledge and wisdom. You will need to reach a place where you understand your own privilege and power and can be attentive and conscientious about yourbiases.
Recognize your biases. How can you care for clients without imposing your biases? Health assessments involve a nurse’s subjective as well as objective knowledge. If your subjective views are influenced by bias, this can affect client engagement and ultimately the outcomes of health assessments. Think about what you need to relearn and unlearn.
- Health assessments require both objective knowledge (knowledge obtained through assessment techniques and skills) and subjective knowledge (knowledge about the unique needs and experiences of clients, obtained through empathetic and relational skills).
- Illness experiences are informed by our social experiences. They are unique, so a one-size-fits-all model of care will not suit all clients.
- An inclusive health assessment involves embracing all aspects of the client’s humanity and being mindful and attentive to any personal and unconscious biases that may negatively influence your views and interactions with the client.
- Inclusive health assessments require that you understand what it is to be human and what it means to be oppressed.
- Without understanding the social roots of illness, it is easy to blame clients for their illness outcomes, or even perpetuate injustice in how a client is treated, and in differential practices of health assessments across clients.
- Nurses should operate from positions of cultural sensitivity, cultural competence, cultural humility, and cultural safety; they have an overarching professional responsibility to anti-oppressive practices.
Chapter 3 - Respiratory System
III
By Dr. Jennifer Lapum, Michelle Hughes, Margaret Verkuyl, Paul Petrie, Siobhan Doyle, and Mahidhar Pemasani
- Apply subjective assessment skills.
- Apply objective assessment skills.
- Use clinical judgment.
- Integrate health promotion interventions into actions.
- Integrate an inclusive approach to respiratory assessment.
Introduction to the Respiratory System
16
The respiratory system is important to assess because it is responsible for gas exchange, specifically facilitating oxygenation and ridding the body of carbon dioxide. If this system is not functioning properly, hypoxemia, hypoxia, and hypercapnia can occur. These pathophysiological processes can affect all body systems. As a nurse, your assessment of the respiratory system provides information about the functioning of this system and potential cues that require your action.
Respiratory System Components
The main components of the respiratory system include the upper and lower respiratory tract (see Figure 3.1).
The upper respiratory tract includes:
- The nasal cavity and paranasal sinuses.
- The pharynx and larynx.
The lower respiratory tract includes:
- The trachea, bronchi, and respiratory units.
- The lungs (three right lobes and two left lobes).
- The pleural membranes (visceral and parietal) and the pleural cavity.
- The pulmonary artery and pulmonary vein.
- The diaphragm.
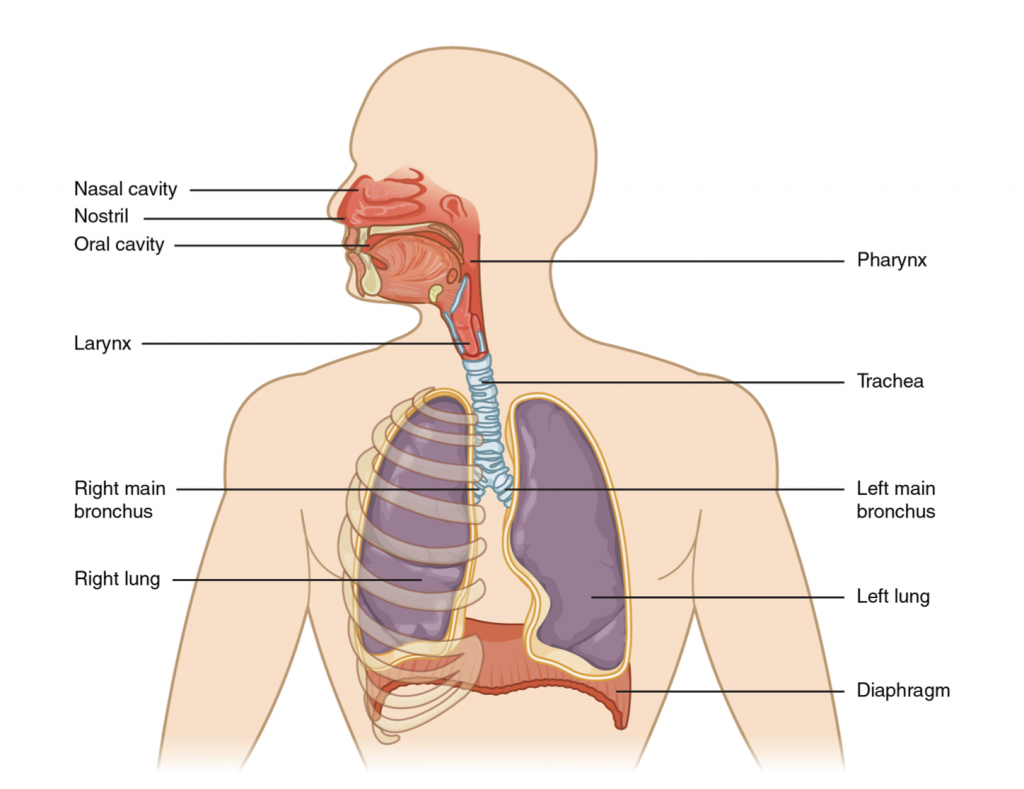
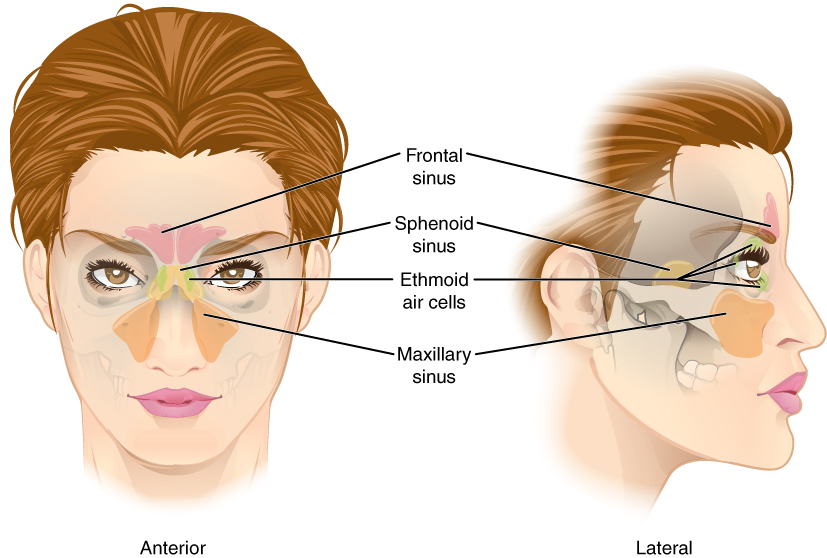
Figure 3.1: Anatomy of the respiratory system
(Attribution: Gordon Betts, Kelly A. Young, James A. Wise, Eddie Johnson, Brandon Poe, Dean H. Kruse, Oksana Korol, Jody E. Johnson, Mark Womble, Peter DeSaix. OpenStax, Anatomy & Physiology. 2013. Used under a CC BY 3.0 license. Download for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction)
You have already learned about the anatomy and physiology of the respiratory system: see Video 3.1 and Video 3.2 for a quick overview.
Video 3.1: Respiratory system physiology
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=63#oembed-5
https://www.khanacademy.org/science/high-school-biology/hs-human-body-systems/hs-the-circulatory-and-respiratory-systems/v/meet-the-lungs
Video 3.2: How the lungs work
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=63#oembed-6
The respiratory system is interconnected and influences many other body systems, so it is rarely assessed in isolation. When attempting to make sense of concerning respiratory cues, nurses commonly assess other body systems: cardiovascular, skin, and musculoskeletal.
Subjective assessment of the respiratory system involves asking questions about the health of the client and symptoms that occur because of pathologies that affect the upper and lower respiratory tract. A full exploration of these pathologies is beyond the scope of this chapter, but common problems associated with the respiratory system include sinusitis, nasal polyps, asthma, pneumonia, cancer, cystic fibrosis, bronchitis, emphysema, chronic obstructive pulmonary disease, and respiratory viruses like coronaviruses and RSV.
Common symptoms that can be related to the respiratory system include nasal congestion/discharge, sinus pain/pressure, dyspnea, coughing, wheezing, and pain. See Table 3.1 for guidance on subjective health assessment. Many of the questions in this table align with the PQRSTU mnemonic. You should consider asking questions in order of importance, thus, you do not follow the sequential order of PQRSTU.
You should also ask about any medications (prescribed or over the counter) the client is taking: the name, dose, frequency, reason it was prescribed, and how long they have been taking it.
Remember to always ask questions related to health promotion. Depending on the context of the assessment, you may ask these questions and engage in a discussion during a subjective assessment or after an objective assessment. A section on “Health Promotion Considerations and Interventions” is included later in this chapter after the discussion of objective assessment.
Many respiratory-related pathologies are related to inflammatory processes, narrowed airways, and mucous production. These processes cause a variety of symptoms including difficulty breathing, coughing, and noisy breathing. They can also influence the body’s oxygenation and affect a person’s capacity to engage in activities of daily living.
The SARS-CoV-2 virus (commonly referred to as COVID-19 disease) is a highly infectious virus (emerged in 2019) that affects the lungs and breathing as well as other body systems. It became a pandemic in 2020 because it was highly transmissible and affected people across the globe. It is transmitted through airborne participles and droplets from the mouth and nose when you breathe, talk/sing/yell, cough, or sneeze. Video 3.3 that will help you understand how the virus affects the lungs in terms of inflammation, fluid accumulation, and lung damage.
Video 3.2: How COVID-19 affects the lungs
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=335#oembed-3
Table 3.1: Common symptoms, questions, and clinical tips
|
Symptoms
|
Questions
|
Clinical tips
|
|
Dyspnea refers to difficulty breathing and can be described as shortness of breath, a feeling of breathlessness, not being able to get sufficient air, or being unable to catch your breath.
The feeling of not being able to catch one’s breath is particularly upsetting because it feels like suffocation.
When a client is having difficulty breathing, they often also have rapid breathing: tachypnea.
Older adults sometimes experience mild shortness of breath upon exertion because of the anatomical lung changes including decreased muscle mass, lung elasticity, and increased lung rigidity. This makes it more difficult to breathe and causes the stiffening of lung expansion and recoil, decreased vital capacity, and increased residual volume.
|
Do you currently have any difficulty breathing or shortness of breath? Have you recently experienced any difficulty breaking or shortness of breath?
Remember to incorporate the language that the client uses into your probing.
Additional probes if the client’s responses are affirmative:
Quality: What does your difficulty in breathing feel like?
Provocative/palliative: Is there anything that makes your breathing worse? Is it worse when you are lying down? Is there anything that makes your breathing better? Does it feel better when you are sitting up?
Severity: Can you rate your difficulty in breathing on a scale of 0 to 10 with 0 being no difficulty and 10 being the most difficult breathing you have ever had?
Timing/treatment: When did the difficulty in breathing begin? What were you doing when it began? Is it constant or intermittent? Do you get short of breath with activity/exertion? If so, what type of activity? Have you taken anything to treat your difficulty in breathing?
Understanding: Do you know what is causing the difficulty in breathing?
|
As you are assessing the client, consider raising the head of the bed so that it is easier for them to breathe. However, this decision may be influenced by whether the client’s condition is stable. For example, if the client is showing signs of clinical deterioration and their blood pressure is low, you should lower the head of the bed to increase the amount of blood returning to the heart.
Use a primary survey approach to determine cues that may indicate clinical deterioration. Assess the client’s respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature, followed by auscultation of lungs.
|
|
Coughing, also known as “tussis,” is a common respiratory symptom. It is usually an involuntary reflex involving expulsion of air from lungs or an attempt to clear one’s throat/breathing passages from foreign bodies, irritants, fluids, and mucus.
Coughing can be associated with acute or chronic infections or diseases. Coughs can be dry or wet, and wet coughs often produce expectorate (mucus). Mucus can be thin or thick and can be clear, yellow, green, pink-tinged, or bloody. Bloody expectorate is called hemoptysis.
|
Do you currently have a cough or have you recently had a cough?
If the client’s response is affirmative, begin with an open-ended probe: Tell me about the cough.
You will probably need to probe further. Additional questions might include:
Quality: Can you describe the cough? Can you describe what the cough sounds like?(Clients may describe the quality in various ways such as dry, wet, bubbling, barking, or hacking. You can provide examples if they are struggling to find the words). Do you cough anything up? (sputum or phlegm/mucus). If so, can you describe it? Is it thick or thin? What colour is it?
Timing/treatment: When did the coughing begin? Is it constant or intermittent? Have you treated it with anything?
Provocative/palliative: Is there anything that makes the coughing worse? Is it worse at a particular time of day? Is there anything that makes it better? Does it feel better when you are sitting up?
Region: Do you feel the cough is worse in a particular area? (e.g., throat, lungs)
Severity: Can you rate your coughing on a scale of 0 to 10 with 0 being no coughing and 10 being the worst coughing you have had?
Understanding: Do you know what is causing the coughing?
|
Until the origin is ruled out, consider it transmissible. Wear eye protection, and you and the client should both wear face masks.
You should consider raising the head of the bed. A client who is coughing with expectorate might be more comfortable sitting upright.
Assess the client’s respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature, followed by auscultation of lungs.
|
|
Chest and nasal congestion is accumulation of mucus in the chest/lungs and/or in the nasal cavity/nose.
This congestion may be associated with coughing, runny nose, and sneezing.
|
Do you have any chest or nasal congestion?
If the client’s response is affirmative, additional probes might include:
Quality/quantity: Tell me about it. How bad is it?
Timing: When did it begin? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Region: Where do you feel the congestion?
Treatment: Have you treated it with anything? Do you take any medications for it?
Understanding: Do you know what is causing it or what it is related to?
|
Assess the client’s respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature followed by auscultation of lungs.
|
|
Sinus pain/pressure is a sensation felt in the sinuses. It is commonly associated with inflammation, infection, and/or blockage of the sinuses.
|
Do you have any pain or pressure in your sinuses?
If the client’s response is affirmative, additional probes might include:
Quality/quantity: Tell me about it. How bad is it?
Timing: When did it begin? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Region: Where do you feel the pressure/pain?
Treatment: Have you treated it with anything?
Do you take any medications for it?
Understanding: Do you know what is causing it or what it is related to?
|
Sinus pain can be associated with several other symptoms such as nasal congestion, nasal discharge, headaches, earaches, and pain around the ear and down the neck. It is important to assess the client for any associated symptoms.
The location of the sinus pain is important to assess to potentially help determine the cause and the sinuses affected.
|
|
Wheezing is a whistling sound or noisy breathing associated with inspiration and/or expiration. It is commonly associated with narrowing of the airways, inflammation, and bronchospasm.
|
Do you hear any wheezing when you breathe?
If the client’s response is affirmative, begin with an open-ended probe: Tell me about the wheezing.
You can probe further with questions related to the PQRSTU mnemonic such as:
How often does it happen? How bad is it? Is there anything that triggers the wheezing? Do you know what causes it? Is there anything that makes it better? Do you treat it with anything? (e.g., medications, puffers).
|
Wheezing can be associated with an acute or a chronic condition. Some clients can hear it themselves and report it; you might also hear it when you auscultate the lungs.
If a client is currently wheezing, it is essential to rule out anaphylaxis, because this is a life-threatening condition. Assess whether the client has allergies and if so, whether they may have been exposed to the allergen. Common allergens related to anaphylaxis are insects (e.g., bees), food, and medications. Related anaphylaxis symptoms might include pruritus, rash/hives, difficulty swallowing, swelling of face or lips, and nausea.
Administration of epinephrine is a priority if anaphylaxis is suspected.
|
|
Chest pain associated with the respiratory system can be described in many ways: a sensation in the chest, discomfort, tenderness, tightness, and sharp pain.
Depending on the etiology, the pain can worsen when breathing and coughing.
|
Do you currently or have you recently had any chest pain or sensations in your chest?
If the client’s response is affirmative, first ask: Do you have the pain now?
Additional probes may include:
Quality/quantity: Tell me about it. What does it feel like? How bad is it?
Timing: When did it begin? What were you doing when it began? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Region: Where do you feel the pain/sensation?
Treatment: Have you treated it with anything? Do you take any medications for it?
Understanding: Do you know what is causing it or what it is related to?
|
It is important to address any current pain, particularly if it could be of cardiac origin.
Pain that is associated with the respiratory system can sometimes be relieved by position change. If the client is stable, try sitting them upright. However, if the client is showing signs of clinical deterioration, it is best to position them in supine position and lower the head of the bed in case prompt intervention is needed.
Assess the client’s respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature, followed by auscultation of lungs.
|
|
Other respiratory symptoms can include fatigue, perspiration, confusion, light-headedness, sneezing, sore throat, headache/body aches, fever/chills, colour changes in skin/lips/nails (such as cyanosis, lymph node swelling, and decreased appetite.
|
Always ask one question at a time. Questions might include:
Have you experienced fatigue? (Or perspiration, confusion, light-headedness, sneezing, sore throat, headache/body aches, fever/chills, colour changes of your skin/lips/nails such as cyanosis, lymph node swelling, decreased appetite?)
Use variations of the PQRSTU mnemonic to assess these symptoms further if the client’s response is affirmative.
|
These symptoms can be related to other body systems and non-respiratory issues. It is important to explore these symptoms specifically if the client answers affirmatively to other respiratory-related symptoms.
|
|
Personal and family history of respiratory conditions and diseases.
As noted earlier, common issues associated with the respiratory system include asthma, allergies, pneumonia, bronchitis, emphysema, chronic obstructive pulmonary disease, cancer, cystic fibrosis, and respiratory viruses like coronaviruses.
|
Do you have any chronic respiratory conditions or diseases? Do you have a familial history of respiratory conditions or diseases? (e.g., asthma, allergies, emphysema).
If the client’s response is affirmative, begin with an open-ended probe: Tell me about the condition/disease?
If the client has a personal history probing questions might include:
Timing: When did it occur? When were you diagnosed?
Quality/quantity: How does it affect you? What symptoms do you have?
Treatment: How is it treated? Do you take medication?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
|
The biological and non-biological nature of family may be important to consider when asking questions: risk factors may be influenced by genetics and/or culture. Although there may be a genetic role to some respiratory-associated diseases (e.g., asthma, cystic fibrosis), it is more likely that environment and cultural factors like family traditions and practices play a larger role (e.g., lung cancer, emphysema). One example might be living with a smoker.
|
It is important to understand which respiratory symptoms are cues that require action. Urgent intervention is required with the following cues: cyanosis/pallor, new onset confusion, severe shortness of breath or wheezing, or chest pain. All of these can be related to clinical deterioration and hypoxia.
If cues suggest clinical deterioration, you should ask a colleague to call the physician/nurse practitioner while you perform a primary survey and a focused objective assessment on the respiratory system. Assess respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature, followed by auscultation of lungs.
If the client is wheezing, and you think it may be related to a foreign object, quickly inspect the nose and mouth and dislodge it if you can do so simply. For example, young children often put small toys/objects up their nose; it can become lodged and affect breathing.
Note that chest pain could be respiratory or cardiovascular related depending on the underlying pathophysiology.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=335#h5p-16
An objective assessment of the respiratory system includes:
- Brief scan of the respiratory system.
- Inspection and palpation of the nose and sinuses.
- Inspection, auscultation, palpation, and percussion of the posterior and lateral thorax followed by the anterior thorax.
An objective assessment is usually completed after the subjective assessment, but if the client shows signs of respiratory distress, you may proceed directly to the objective assessment and associated interventions. In this case, it is important to prioritize care after a brief scan that involves components of the primary survey. The physical techniques of inspection and auscultation are usually prioritized.
It is important to be aware of the landmarks of the anterior and posterior chest. This knowledge helps you accurately landmark and also informs the documentation of the findings. See Figure 3.2 for anatomical locations and Figure 3.3 for reference lines.

Figure 3.2: Anatomical landmarks
Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
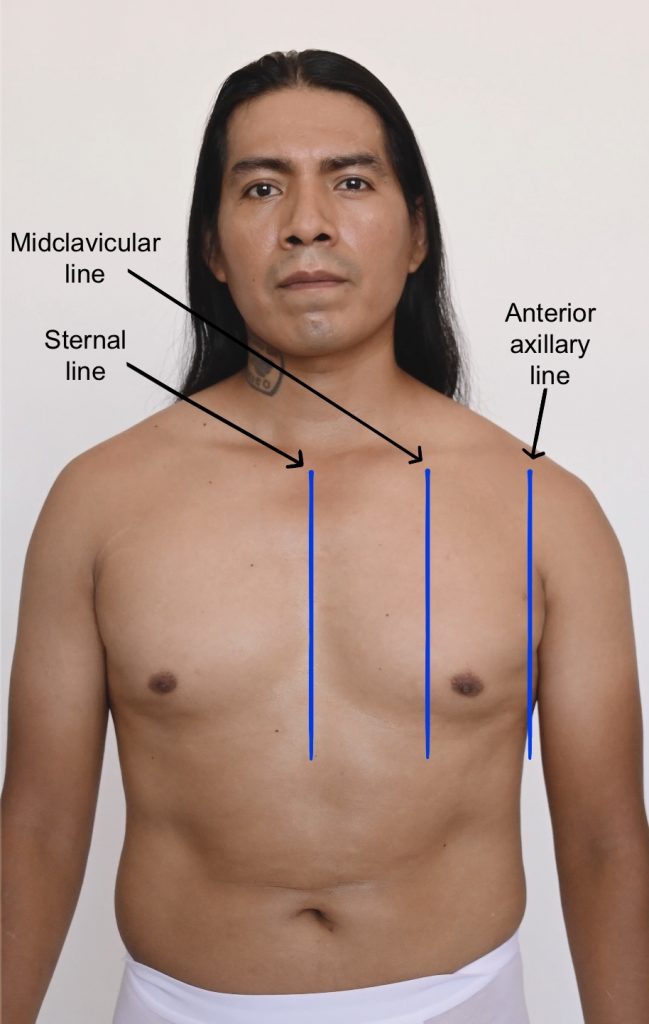
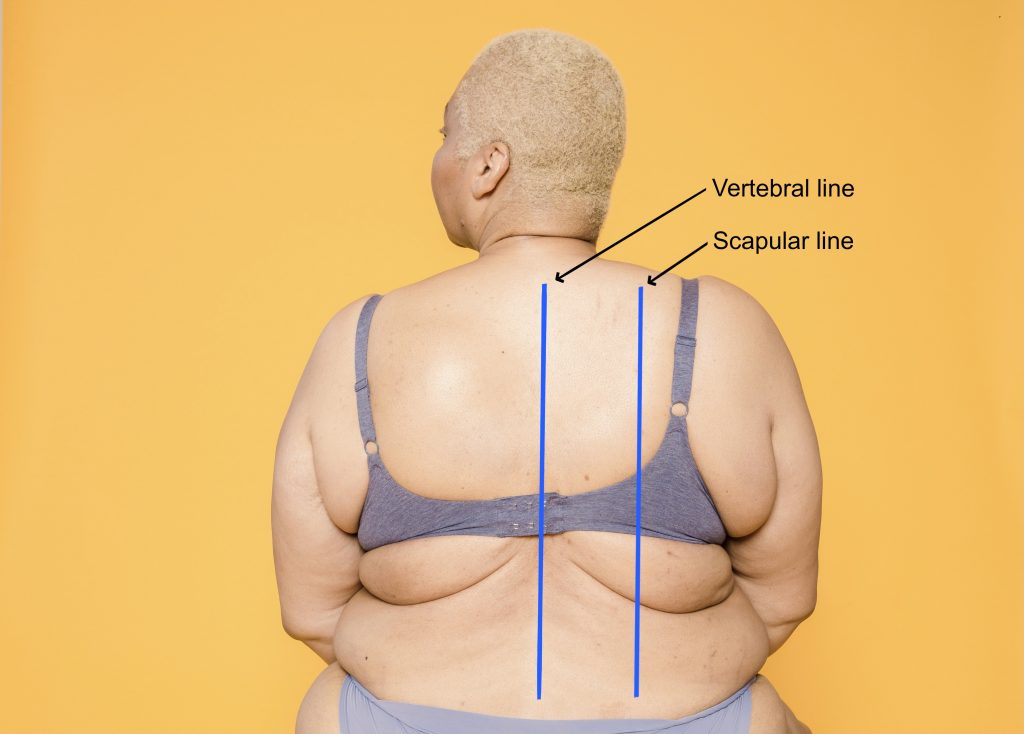
Figure 3.3: Reference lines
Image on left: Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
Image on right: Photo by Laura Tancredi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
Be aware of the environmental temperature in the room and the temperature of your hands. Room temperatures are not easily modified, so you should attempt to limit exposing the client and keep them covered. You should also try to warm your hands and stethoscope before placing them on the client’s body.
Ensure the client is positioned in the best way to assess the lungs: usually seated or in the high-fowlers position with the client looking straight ahead so that the lungs can fully expand. If you are assessing a young child or newborn, you could ask someone (e.g., care partner, healthcare provider, parent) to help hold the client upright on the exam table or sit the client in their lap while assessing the respiratory system.
You should help the client into the side-lying position if they are in a supine position and cannot sit upright. This repositioning may require the help of another healthcare provider if the client is unable to roll over themselves.
Assessment of the posterior and lateral thorax involves assessing from the shoulders and the axillary area down to the bottom of the rib cage. Assessment of the anterior thorax involves assessing from the lung apices (just above the clavicles) down to the bases (at bottom of the rib cage). To help visualize, see Figure 3.4 for the location of the lobes on the anterior and posterior thorax and Figure 3.5 for the location of the lobes on the lateral thorax (shown upon inspiration).
Keep in mind, you should do the entire assessment on the bare skin.
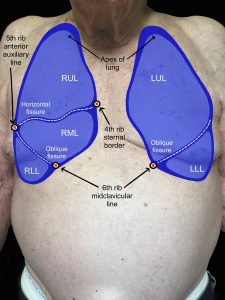
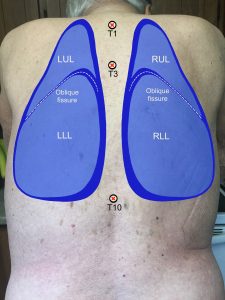
Figure 3.4: Location of lobes on anterior and posterior thorax
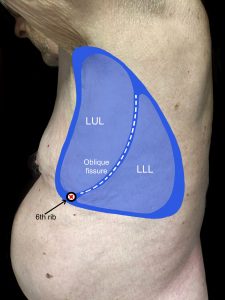
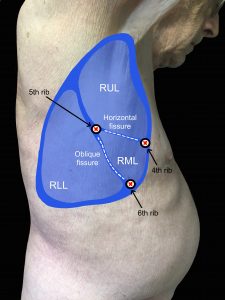
Figure 3.5: Location of lobes on lateral thorax
Always use a trauma-informed approach to inform your respiratory assessment. This is particularly important considering that areas of the chest will be exposed. Do not assume who may have experienced trauma: it can happen to anyone, regardless of gender, age, or socioeconomic/educational level.
You could start by asking the client if they would like a family member or friend present or another healthcare provider. You should explain what you are doing throughout the assessment and explain why these actions are important to perform. Sometimes it is helpful to show on your own chest (over your uniform) where you will be palpating and placing your hands or the stethoscope.
Maintain privacy by closing the door and/or curtains. Use draping and only expose the necessary areas of the chest. Clients may feel awkward or embarrassed having their thorax exposed, particularly the anterior side. This feeling can be felt by people of all genders and ages. While you have the gown open at the back, use the drape to cover the lower half of the thorax. When you need to assess the anterior thorax, use the drape to cover any area not being assessed; the drape can be secured around the abdomen. With the anterior thorax, you can ask the client to lower the patient gown at the top so that you can assess the upper thorax and then, you can have them pull the gown up at the bottom to assess the lower thorax. Another alternative method is to have gown open at the front instead of the back.
You should always be professional, confident, and efficient. Try to be responsive to the client’s verbal and non-verbal cues. If they seem uncomfortable, you could acknowledge this by saying, “Many clients feel uncomfortable having their lungs assessed because it involves exposing their chest. I will only ask you to expose the areas that I need to assess and then you can cover back up again. Is there anything I can do to make this easier for you?”
Contextualizing Inclusivity – Chest Binding
An inclusive approach to health assessment is vital because clients need to feel accepted for who they are. Some non-binary and transmasculine clients may wear a chest binder because they feel uncomfortable or distressed about having breast tissue. Binders are garments designed to flatten the appearance of the chest wall. They come in different forms and can extend from the chest down to the diaphragm or to the hips: they may look like a sports bra or tank top, and some clients may use compression bandage.
The binder needs to be removed to adequately listen to the lungs, as these sounds may be diminished through the binder. You may or may not be aware of whether the client you are assessing wears a chest binder, so you can apply an inclusive approach by acknowledging the vulnerability that clients may feel. Provide step-by-step instructions so that they are prepared, and ask non-judgmental questions like “Assessing your lungs requires me to assess on the bare skin on the front and back of your chest. Is there anything that would impede me from doing so?” You can also ask if they have any questions before beginning such as “Do you have any questions before we begin?”
You should also assess the binder for proper fit: a good fit allows for normal chest expansion and deep breathing.
Brief Scan – Respiratory System
19
A brief scan (see Figure 3.6) involves inspection of the client’s breathing and includes elements of the primary survey. This assessment helps you quickly recognize cues of clinical deterioration, specifically signs of respiratory distress, and may influence your decision on whether immediate action is required. The steps of a brief scan are prioritized in order of importance. For example, you need to assess whether an airway is patent (i.e., not obstructed) before you assess presence of breathing and respiratory rate.
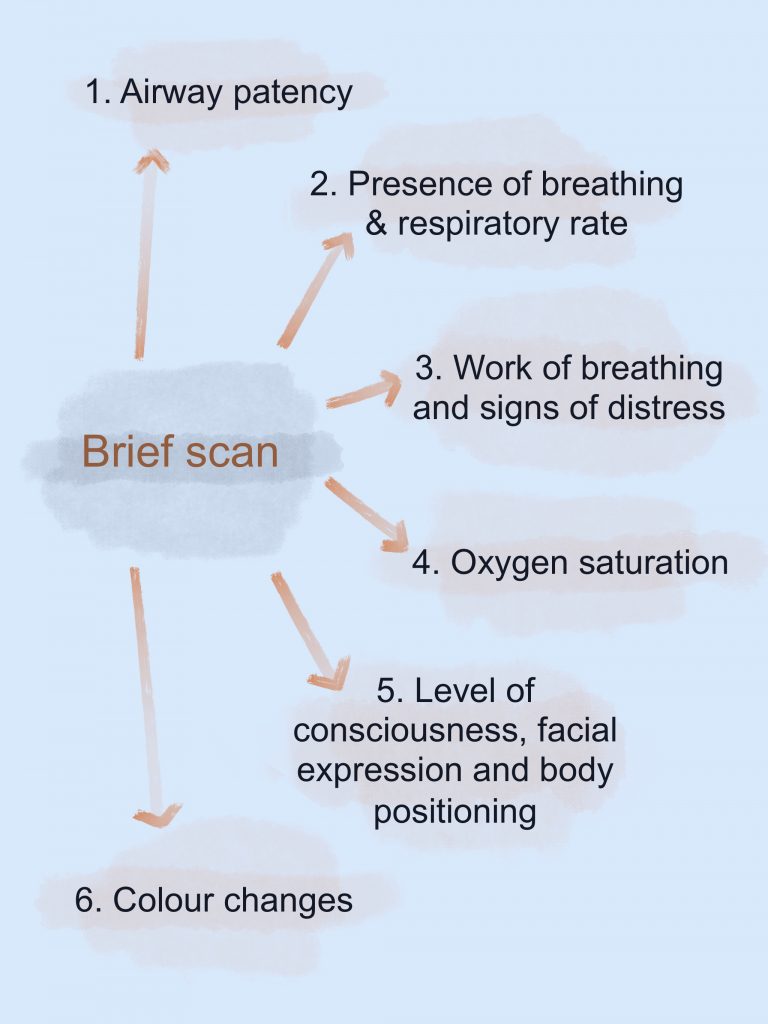
Figure 3.6: A brief scan
Guided by the primary survey, steps of the brief scan of the respiratory system include assessing respiratory effort and signs of respiratory distress:
1. Assess airway patency
- Determine whether there is an open airway or the presence of obstructive airway symptoms (e.g., secretions [mucus, blood, vomit], snoring, stridor, difficulty breathing, coughing, drooling, wet sounding voice, unable to speak). Partial or complete obstruction of airways are commonly associated with foreign objects, inflammation, and direct injury/trauma to the airway. An obstructed airway is a first level priority of care because it affects oxygenation and can lead to clinical deterioration.
2. Assess presence of breathing and respiration rate
- First, assess the presence of breathing and eupnea, which is normal automatic breathing with a regular rhythm. Apnea is the cessation of breathing and can be permanent or intermittent. It can result in severe hypoxia, and can be associated with respiratory depression from certain medications, and can also involve sleep apnea when breathing stops intermittently.
- If breathing is present, count the rate for 30 seconds if the rhythm is regular and one minute if it is irregular. Are there signs of bradypnea or tachypnea? See Table 3.2 for normal respiratory rates.
Table 3.2: Respiratory rate ranges (taken from: https://pressbooks.library.ryerson.ca/vitalsign2nd/chapter/what-is-respiration/)
| Age |
Rate (breaths per minute) |
| Newborn to one month |
30 to 65 |
| One month to one year |
26 to 60 |
| 1 to 10 years |
14 to 50 |
| 11 to 18 years |
12 to 22 |
| Adult and older adult |
10 to 20 |
3. Assess work of breathing and signs of respiratory distress.
- Is the breathing silent or noisy? Do you hear wheezing or stridor? Normal breathing is silent. Noisy breathing with wheezing or stridor is a sign of distress.
- Do you observe nasal flaring? (This is a common symptom of respiratory distress particularly in infants and young children. However, keep in mind that newborns are nose breathers. Additionally, air does not enter the lungs until birth so the newborn may be congested and you may observe nasal flaring).
- Do you observe use of the accessory muscles (i.e., sternomastoid and trapezius) and intercostal tugging/pulling/retractions? Unobstructed breathing with no respiratory distress should be quiet with no observable use of accessory muscles or intercostal tugging. Observable use of accessory muscles and intercostal tugging are signs of distress.
- Do you observe any abnormal patterns of breathing? One example of an abnormal pattern of breathing is agonal breathing; it involves an irregular rhythm with gasping and is a sign that a person is near death.
4. Assess oxygen saturation.
- Is the oxygen saturation level below 95 to 97%? Although 97 to 100% is the normal range for oxygen saturation levels, older individuals may have a slightly lower saturation (also, see Knowledge Bites for information about when lower oxygen saturations are acceptable in certain populations). Keep in mind that a saturation below 97% with children should always be further investigated.
- Nail polish should be removed before assessing oxygen saturation with a pulse oximeter on the finger.
- The accuracy of pulse oximetry can be affected by low perfusion states (e.g., vasoconstriction or low cardiac output). If you suspect low perfusion or you are getting a weak signal on the finger, use a pulse oximeter that snaps on the ear or can be taped to the forehead. These approaches to measuring oxygen saturation are best when a client has artificial nails.
Contextualizing Inclusivity – Pulse Oximetry
Oxygen saturation measured with pulse oximetry is sometimes overestimated in a client with dark skin: oxygen saturation may appear higher than it really is. If a client indicates that they are short of breath, but this is not reflected on the pulse oximeter, believe the client and assess further. It is always best to assess further when the client’s signs and symptoms do not align with the pulse oximetry.
5. Assess level of consciousness, facial expression, and body position for signs of respiratory distress.
- Does the client have an altered level of consciousness and confusion? Normally, clients should be alert and oriented.
- Does the client show signs of agitation such as wide eyes and grimacing? Normally, a client should have a relaxed facial expression.
- Is the client showing signs of distress including hunched over/tripod position or unable to sit up? A client should normally be in a relaxed posture, while those in respiratory distress often shift into a tripod position: leaning forward with hands and/or forearms resting on their legs or another surface such as a table.
6. Assess colour changes (and fingernails for clubbing and testing capillary refill)
- Are there signs of cyanosis or pallor in the lips, mucous membranes, fingernails, or conjunctiva? Cyanosis and pallor result from hypoxemia, and can have many causes.
Contextualizing Inclusivity – Assessing Colour Change
Cyanosis: This is best seen in areas with rich vasculature and thin overlying dermis: mucous membranes/lips, conjunctiva, and extremities (fingernails). In people with darker skin, cyanosis can appear as a grey/white shade around the lips and the conjunctiva can appear as a grey/bluish shade while people with yellowish tones to their skin can have a greyish/green shade (Lewis, 2020; Sommers, 2011). In people with lighter skin, cyanosis appears as a dusky bluish/purple shade (Lewis, 2020).
Pallor: In people with darker skin, this can appear as a grey shade to the mucous membranes/lips, nail beds, and skin, and a yellowish shade in people with lighter brown skin; it can be helpful to look at the palms of people with dark skin when assessing for pallor as they tend to be paler (Lewis, 2020). In people with lighter skin, pallor can appear as a generalized pale discolouration to the skin, nail beds, and mucous membranes/lips. In people of all skin colours, the conjunctiva is normally a healthy pink due to the vascularity, but with pallor it will appear white or very pale pink (Mukwende et al., n.d.).
- While assessing fingernails, also assess for presence of clubbing. Clubbing is related to conditions that lead to chronic hypoxia and cause the nail angle to flatten to 180 degrees or more, the nail bed to soften and become spongy, and the fingertips distal to the distal interphalangeal joint to become enlarged. Normally, the nail angle is about 160 degrees with firm nailbeds, and no enlarged fingertips. It is often assessed on the index finger, but in cases of early clubbing it may not have advanced to that digit, so it is best to assess the thumb first. To assess for the presence of clubbing:
- Ask the client to stick their thumb (or index finger) out so that it is parallel to the ground and view it at eye level (this is considered the profile sign).
- Inspect the nail angle at the intersection of where the nail base meets the skin (the angle should be about 160 degrees).
- Inspect for enlarged fingertips that look “bulb-like” (see Figure 3.7).
- Palpate the nail bed (it should be firm to touch).
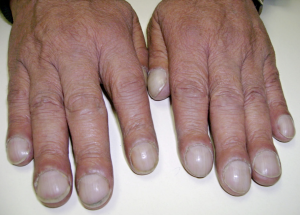
Figure 3.7: Clubbing of fingernails on a person’s hands. Taken from Acopaquia.jpg by Desherinka is licensed under CC BY-SA 4.0
- Test capillary refill on two or three fingernails of each hand. Start by applying pressure with your own finger to the client’s nail; this causes the nail to blanch (become pale in colour). Apply the pressure for about 5 seconds and then release and observe the return in colour. It should return within 3 seconds or less; a more sluggish return (more than 3 seconds) suggests that there may be issues with oxygenated blood perfusion, which might be caused by respiratory, cardiac, and/or peripheral vascular system issues.
7. Note the findings
- Normal findings might be documented as: “Patent airway, quiet breathing with no signs of respiratory distress. Alert. Oxygen saturations 98%. No colour changes with translucent nails and pinkish undertone. No signs of clubbing. Capillary refill returns within 1–2 seconds.”
- Abnormal findings might be documented as: “Stridor present, nasal flaring and intercostal tugging, pallor noted around lips. Oxygen saturations 91%. Slow capillary refill at 4–5 seconds.”
A client who is in respiratory distress requires immediate intervention, especially if signs indicate an obstructed airway, increased work of breathing, an altered level of consciousness, and an oxygen saturation dropping below 92%. Stay with client and call for help (a senior nurse, physician, or nurse practitioner) if a client is in respiratory distress.
- If an airway is not patent, try to open the airway with a head-tilt-chin-lift and inspect the mouth and nose for obstructions.
- If oxygen saturations are low, try to wake the client if they are sleeping, sit them upright, and ask them to take a few deep breaths. Supplemental oxygen can be applied if there are standing orders on your unit.
You may need to keep the client in a supine position if you suspect that they are deteriorating quickly and may go into respiratory or cardiac arrest. Notify the critical care response team (CCRT) or call a code in this case. Bag-mask-ventilation may be needed if the client is in respiratory arrest.
Lower oxygen saturation levels (between 88 to 92%) are acceptable for those with Chronic Obstructive Pulmonary Disease (COPD).
In a healthy person without COPD, the strongest stimulus for the normal respiratory drive is hypercapnia (increased carbon dioxide, CO2, in the blood). This means that a person is stimulated to breathe when there are high CO2 levels in their blood.
In contrast, a person with COPD has a reduced capacity to exhale carbon dioxide, leading to hypercapnia (increased CO2 in the blood). As a result, there is a shift in the normal respiratory drive: the respiratory drive becomes a hypoxic drive, meaning that low oxygen is the primary stimulus to breathe. This means that low oxygen levels stimulate respirations as opposed to hypercapnia because a person with COPD is a CO2 retainer (i.e., they retain CO2 in their lungs). Therefore, when performing a brief scan, consider oxygen saturation levels in the context of existing conditions and be cautious about applying oxygen when a client’s oxygen saturation is lower than normal, particularly if the client has COPD.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=339#h5p-17
References
Lewis, G. (2020). Identifying AEFI in diverse skin colour. https://mvec.mcri.edu.au/references/identifying-aefi-in-diverse-skin-colour/
Mukwende, M., Tamony, P., & Turner, M. (n.d.). Mind the gap: A handbook of clinical signs in black and brown people. (1st edition). https://litfl.com/wp-content/uploads/2020/09/Mind-the-Gap-A-handbook-of-clinical-signs-in-Black-and-Brown-skin.-first-edition-2020.pdf
Sommers, M. (2011). Color awareness: A must for patient assessment. American Nurse. https://www.myamericannurse.com/color-awareness-a-must-for-patient-assessment/
Inspection and palpation of the nose should be performed standing directly in front of the client while they are sitting upright on the examination table or a chair. It is important to don gloves as you may be in contact with bodily fluids such as nasal discharge.
Inspection
Steps to inspect the nose include:
- Inspect the external surface of the nose for colour.
- Normally, the nose is the same colour as the rest of the face with no discolourations such as redness. Describe the appearance and location of any discolourations noted.
- Inspect the contour and external surface of the nose for symmetry, swelling, and malformations such as masses and lesions.
- Normally, the nose is symmetrical with no swelling or malformations. Describe the appearance and location of any abnormalities.
- Inspect the nasal cavity and mucosa of the nose for colour, discharge/bleeding, swelling, foreign bodies, and malformations. See Figure 3.8 and Video 3.4.
- Ask the client to tilt their head gently backwards while you use your finger to elevate the tip of their nose.
- Use a penlight or the light source from a otoscope to illuminate the nasal cavity. Use a large/wide cover for the otoscope probe and ensure that you do not touch any part of the nose with it as the mucosa is sensitive and highly vascular. Discard the probe cover in the garbage when done.
- The nasal mucosa is normally pinkish red in colour with no discharge or bleeding. Describe any discolouration of the mucosa or the colour and amount of any discharge/bleeding. Describe the appearance and location of swelling and foreign bodies. In children, common foreign bodies include little toys and beads.
- Common malformations may include lesions, masses, polyps, and deviated or perforated septum. If any are present, describe the appearance and location. Polyps appear as a tear-drop formation. A deviated septum is when the septum is off centre and bulges laterally. A perforated septum is when there is a hole/opening in the septum; it is typically observed when you illuminate one side of the nasal cavity and you observe the light on the other side.
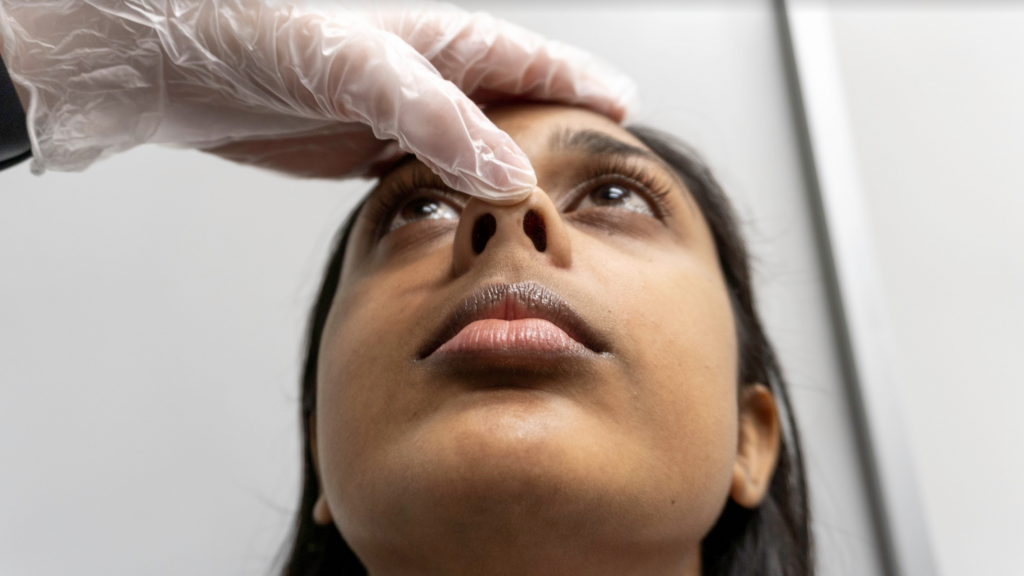
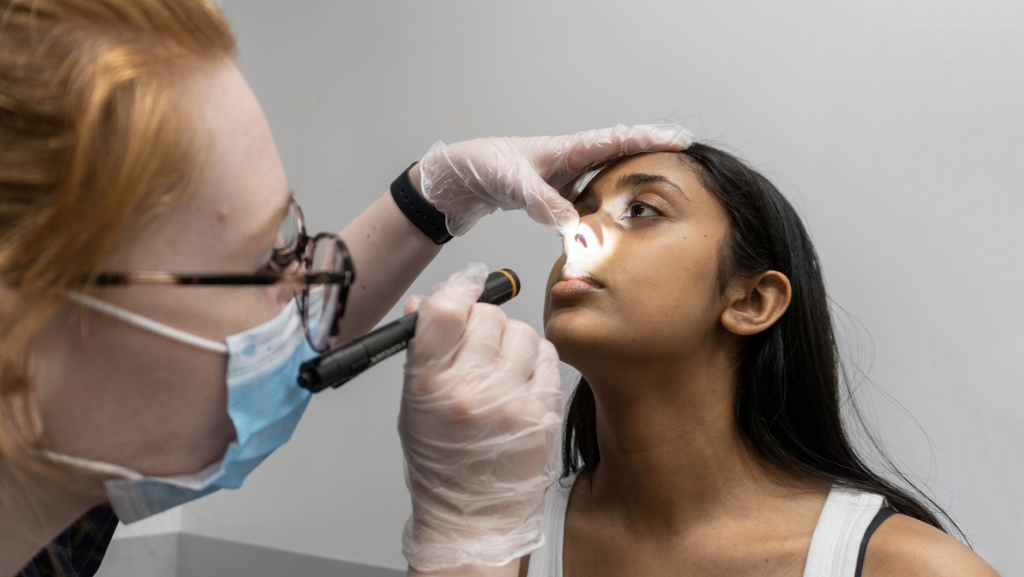
Figure 3.8: Inspecting the nasal cavity and mucosa
4. Note findings:
-
- Normal findings might be documented as: “External nose is symmetrical with no discolouration, swelling or malformations. Nasal mucosa is pinkish red with no discharge/bleeding, swelling, malformations or foreign bodies.”
- Abnormal findings might be documented as: “Bright red nasal mucosa with purulent discharge.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=1389#oembed-3
Video 3.4: Inspecting the nasal cavity and mucosa
Palpation
Steps to palpate the nose and sinuses include:
- With your thumb, gently palpate one sinus at a time.
- Use a circular motion to palpate.
- Begin with the frontal sinuses inferior to the eye brows over the bony ridge. Avoid the eye socket.
- Then, palpate the maxillary sinuses inferior to the zygomatic bone slightly lateral to the nose.
- Inquire if the client had any pain/tenderness upon palpation. A slight pressure is normal. If pain/tenderness is present, assess further subjectively.
- Palpate the nose for airflow/patency.
- Occlude one naris at a time while placing your index finger over the outside of the nose/nasal wing.
- Ask the client to take a deep and quick inhalation in through the nose (like a sniff in which you draw air inwards as if you are trying to smell something).
- Note the client’s capacity to breathe inwards. The client should be able to breathe inwards with no obstructions.
- Gently palpate the external nose if trauma/injury or lesions are present.
- Use the thumb and the index finger to palpate the contour.
- Lesions can be palpated with the index finger and note the consistency of lesions (e.g., are they soft or firm?).
- Note the findings:
- Normal findings might be documented as: “No sinus pain noted. Nose is patent with good air flow.”
- Abnormal findings might be documented as: “Left frontal sinus pain 6/10.”
None of the abnormal findings on their own are considered critical findings. However, you should call for assistance while monitoring breathing and vital signs and performing a focused assessment if the client is experiencing signs of respiratory distress associated with any malformations, trauma/injury to the nose, or nasal obstructions. It can be helpful to sit the client upright to assist with breathing. Deviated septum is quite common. Unless it affects a client’s breathing, typically no action is required. Similarly, if a client has a nasal obstruction or an absence of sniff, you should attempt to determine the cause. Is it mucous or a foreign body (like a toy)? Does it just affect one side? If an obstruction is noted, assess for the presence of any findings of respiratory distress. Usually absence of sniff in one naris isn’t an urgent finding as you can breathe through the other side and the mouth, but you should evaluate the cause. Other abnormal findings that require action are lesions and sinus pain. A focused assessment should be performed and findings reported to the physician/nurse practitioner. Depending on the cause, sinus pain may require treatment such as decongestants, antibiotics, or antihistamines. Cutaneous lesions on the nose should be closely examined. There are many causes of lesions such as herpes simplex virus or a melanoma. For example, the lesion in Figure 3.9 is a carcinoma. These lesions are not a critical finding, but they are life-threatening; they require prompt intervention because they are curable if diagnosed and treated early.
Figure 3.9: Squamous cell carcinoma lesion
(Image from the National Cancer Institute: https://visualsonline.cancer.gov/details.cfm?imageid=2165)
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=1389#h5p-62
Posterior and Lateral Thorax - Inspection
21
1. Inspect for symmetry of thorax and chest expansion.
- Compare the left and right sides of the thorax. Are the shoulders, scapula, and ribs on symmetrical upon observation?
- When the client breathes, does the left and right sides of the thorax expand and recoil symmetrically? Also, test for symmetrical chest expansion by placing your thumbs (on either side of vertebra) just below the inferior border of the scapula (about T9/T10) with fingers stretched out to the lateral sides of the thorax. Pinch a piece of skin in between your thumbs and ask the client to take a big breath in and out. If the thumbs move equally apart and back together at the same time upon inspiration and expiration, this indicates symmetrical expansion. Make a note if the expansion is asymmetrical (one side has limited expansion, lags in expansion, or does not expand). This can happen when one lung cannot expand due to conditions that involve inflammation and air between the lungs and chest wall (i.e., pneumothorax) or partial or complete collapse of the alveoli (i.e., atelectasis). You may also notice that in pregnant women, the thorax shortens while the costal angle widens to accommodate the enlarging uterus: this is normal.
2. Inspect the spinous process, ribs, deformities, masses, and swelling.
- Do the spinous processes appear in a straight line down the vertebral line of the posterior thorax?
- Are the ribs sloping downwards?
- Do you observe any deformities, masses or swelling?
3. Inspect skin colour and skin integrity
- Is the skin colour consistent across the posterior and lateral thorax?
- Do you notice any skin discolouration?
- Do you notice any scars? If so, ask the client the cause. For example, a client may have a scar from lung surgery such as a lobectomy, and this surgery can lead to no air entry when you auscultate the lungs.
4. Inspect the anteroposterior to transverse diameter of the thorax. See Figure 3.10. The transverse diameter is shown in the first image across the chest. The anteroposterior diameter is show in the second image from front to back. In most adults, the anteroposterior to transverse diameter ratio is about 1:2.
- The ratio will be closer to equal (1:1) when a client has conditions that give rise to hyperinflated lungs (e.g., emphysema). Also, a 1:1 ratio is usually present in children younger than two years of age.
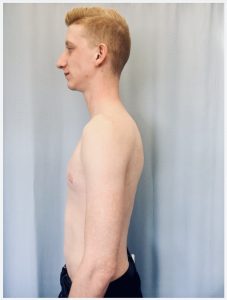
Figure 3.10: Anteroposterior to transverse diameter
5. Note the findings
- Normal findings might be documented as: “Symmetrical posterior thorax with symmetrical chest expansion, no thorax deformities or masses, spinous process in a straight line, no skin discolouration, anteroposterior to transverse diameter 1:2.”
- Abnormal findings might be documented as: “Horizontal ribs with a 1:1 anteroposterior to transverse diameter.”
None of the abnormal findings on their own are considered critical findings. However, if you notice asymmetrical lung expansion, be aware that this is associated with decreased ventilation. You should investigate whether there is decreased or absent air entry in the affected lung, which may be lagging behind or not expanding at all. Examples of underlying pathologies can include pneumothorax, atelectasis, pleural effusion, or partial or complete obstruction of the airway on the ipsilateral side.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=341#h5p-18
Posterior and Lateral Thorax – Auscultation
22
Auscultating the posterior and lateral thorax involves the following steps (see Video 3.5):
Step 1: Perform hand hygiene and cleanse the stethoscope.
Step 2: Ensure the client is in an upright position and ask them to take a big breath in and out through the mouth each time they feel the stethoscope on their posterior thorax.
-
-
- Instruct the client to breathe through the mouth because this makes it easier for you to listen to lung sounds, particularly if there is any nasal congestion or obstructions.
- Keep in mind that breathing a bit more deeply may trigger shortness of breath or dizziness for some clients. You should notify them that they can take a break and breathe normally if they need to. Also be aware that older adults may have difficulty taking a big breath.
Step 3: Place the stethoscope’s diaphragm on the chest in about four to eight locations on each side of the posterior thorax and then at three locations on the right lateral thorax and at two locations on the left lateral thorax so that you listen to all lung lobes. Make sure you have a complete seal. See Figure 3.11 for the placement pattern. The number of locations depends on the size of the thorax. For example, less locations are needed on a client with a smaller thorax (e.g., infants). Note that the posterior thorax is primarily lower lobes.
-
-
- On the posterior thorax, begin at the shoulders at the scapular line, moving from one side to the other side, then move down, and repeat. As you move down the thorax, place your stethoscope close to the vertebral line so that you avoid listening over the scapula. Toward the bottom, listen close to the vertebral line and also move laterally.
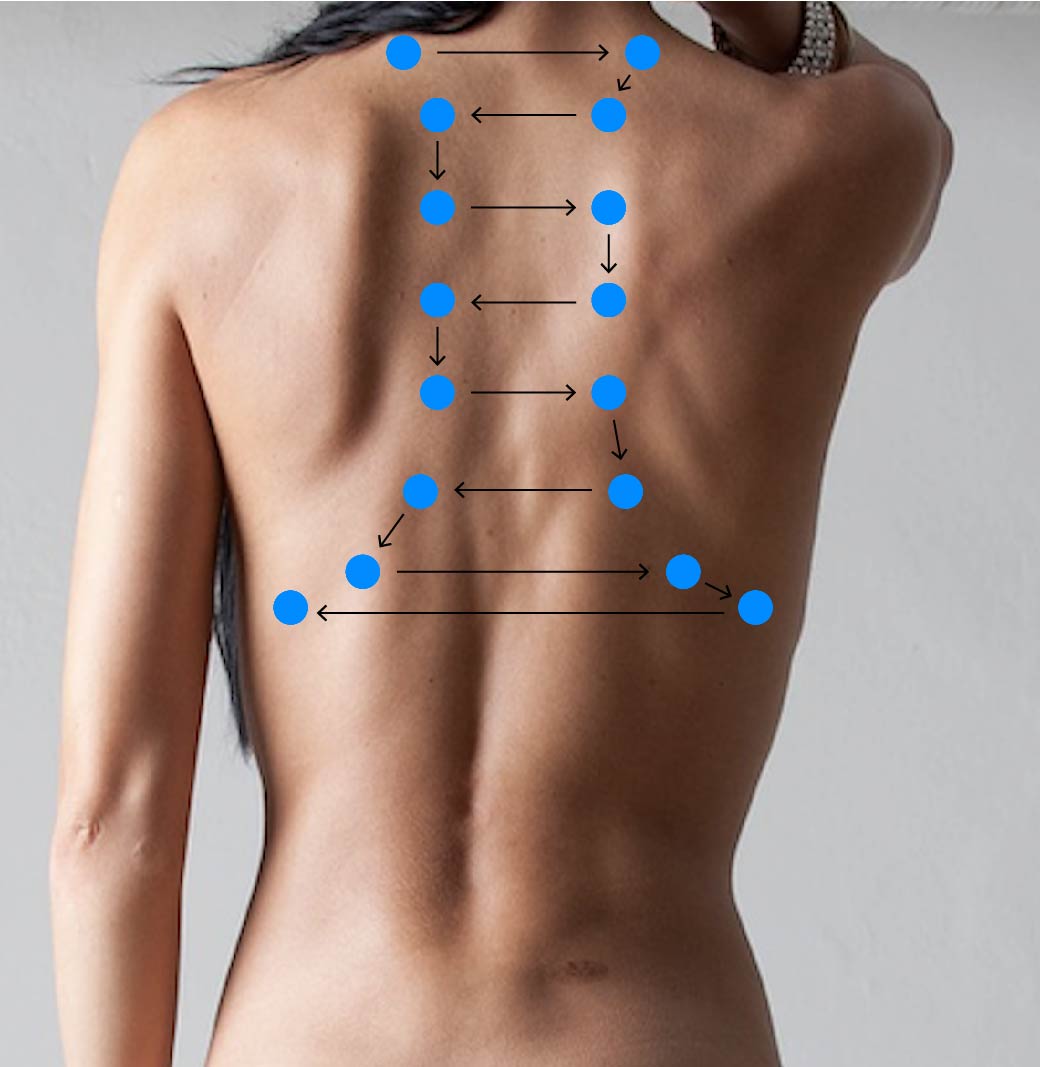
Figure 3.11: Placement pattern for auscultation of posterior thorax
Image by Claudio_Scott from Pixabay (image was cropped and illustrated upon for the purposes of this chapter)
-
-
- On the lateral thorax, place the stethoscope at three locations on the right side so that you listen to the right upper, middle, and lower lobes, and then two locations to listen to the left upper and lower lobe. See Figure 3.12 below.
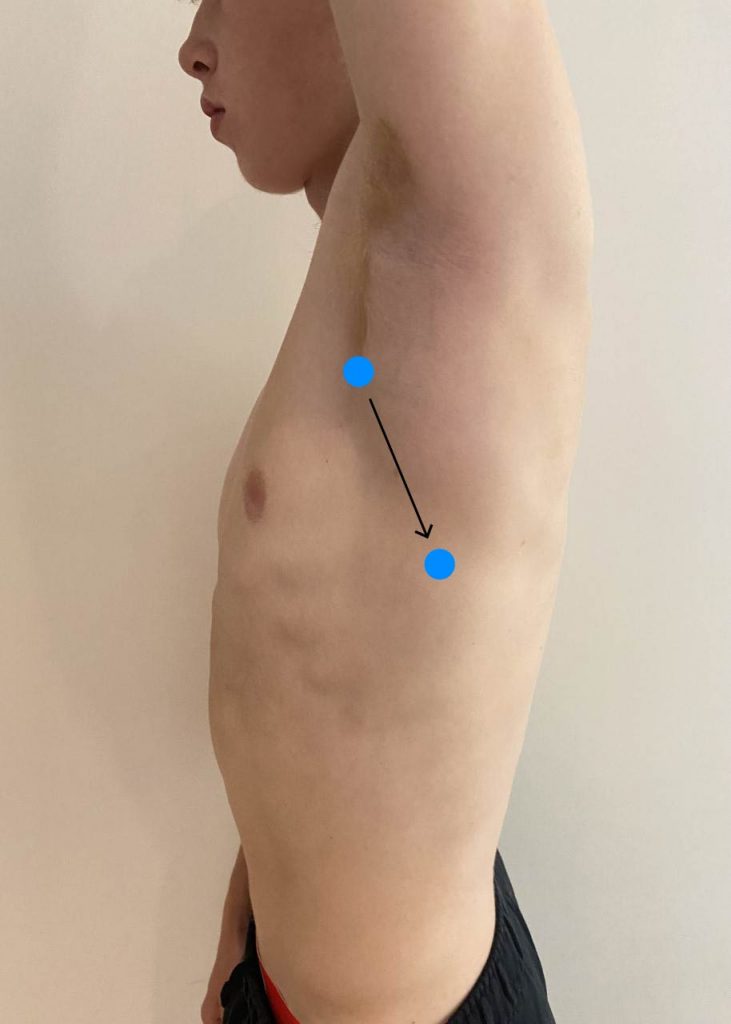
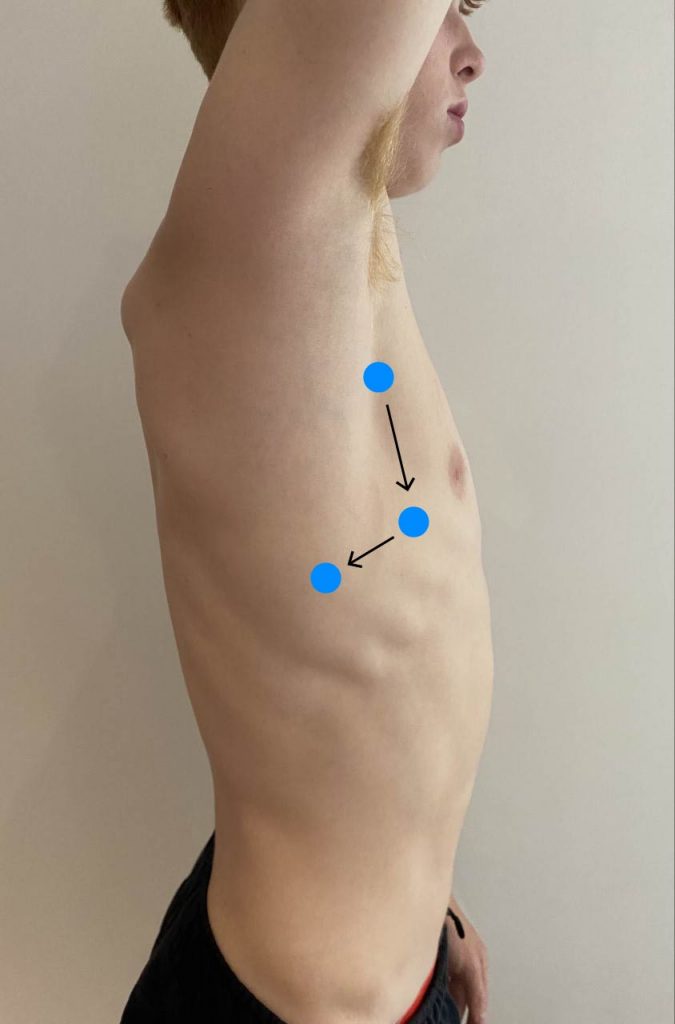
Figure 3.12: Placement pattern for auscultation of lateral thorax
Step 4: In each location, listen to one full respiration (inspiration and expiration) and compare air entry bilaterally.
Step 5: Listen for the following:
-
-
- Air entry quality and equality.
- Quality: Note whether it is good, decreased, or absent.
- Equality: Note whether air entry is equal bilaterally.
-
- Normal breath sounds including clear air entry and the location of bronchovesicular and vesicular.
- Air entry is normally clear with no abnormal sounds (e.g., adventitious breath sounds – see below)
- Bronchovesicular breath sounds are moderate in loudness; inspiration is equal to the expiration phase, and heard on the upper thorax close to the vertebrae and near the bronchi.
- Vesicular breath sounds are quiet and low-pitched; inspiration is longer than the expiration phase, and heard in the periphery of the lung fields and near the smaller airways in an older child and adult. (Note: in young children particularly under two and threes of age, vesicular sounds are not heard because of their small thoraxes. Rather, you hear bronchovesicular).
NOTE: When a person takes a breath in, it takes time for the air to get to the periphery of the lung fields resulting in a long inspiration phase. When a person breathes out, the expiration phase is short with vesicular sounds because the breath leaves the periphery of the lung fields quickly.
NOTE: Another type of normal breath sounds are bronchial sounds, which are heard over the tracheal area. These sounds are described as hollow sounds and harsh sounds, particularly upon expiration; the expiration phase is longer than the inspiration phase. These are heard over the trachea area, and are not heard on the posterior thorax except in the case of an underlying pathology.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=343#h5p-69
Audio 3.1: Normal breath sounds
-
-
- Adventitious sounds are abnormal lung sounds with several causes. You will become familiar with the quality of these sounds after listening to the thorax of many clients and listening with an expert nurse. When you hear these sounds, you should note the quality and the location. For example, what lobes do you hear these sounds in?
- Wheezes are an adventitious sound heard in the lungs when there is bronchoconstriction (i.e., narrowing of the airways) that can happen with inflammation and bronchospasm with conditions such as asthma, emphysema, or an allergic reaction. Wheezes are a continuous musical-like sound that can be heard on inspiration or expiration and can be low- or high-pitched. Higher pitch = increased bronchoconstriction. Lower pitch = decreased bronchoconstriction. Wheezes are often described as mild, moderate, or severe.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=343#h5p-71
Audio 3.2: Adventitious sounds: Wheezes
-
-
-
- Stridor is a more extreme form of wheezing when the upper airways are partially obstructed, and have congenital (i.e., problem present at birth), infectious (e.g., croup, bronchitis), or trauma-related (e.g., foreign body, neck fracture) causes. The sound is continuous and high-pitched. Although commonly heard on inspiration, it can be heard on expiration too. It is usually associated with other signs of respiratory distress and requires immediate response.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=343#h5p-72
Audio 3.3: Adventitious sounds: Stridor
-
-
-
- Crackles are an adventitious sound heard in the lungs when there is an accumulation of fluid (e.g., mucus), such as with pneumonia. They sound like an interrupted popping and even a bubbling noise that can be described as fine, moderate, or coarse crackles depending on the severity. Mild crackles are typically heard in the bases because fluid accumulation in the lungs is affected by gravity. Crackles are typically heard upon inspiration, but they may be heard upon expiration and heard throughout the thorax, particularly when the crackles are coarse. Coarse crackles are associated with increased severity in terms of fluid accumulation in the lungs.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=343#h5p-70
Audio 3.4: Adventitious sounds: Crackles
Step 6: Note the findings:
-
-
- Normal findings might be documented as: “Good air entry, equal bilaterally, no adventitious sounds audible throughout all lobes. Bronchovesicular sounds heard in upper lobes close to vertebrae. Vesicular sounds heard throughout periphery and lateral lobes.”
- Abnormal findings might be documented as: “Decreased air entry heard in left lower lobe with moderate crackles.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=343#oembed-3
Video 3.5: Auscultation of posterior and lateral thorax
If a newborn or young child is sleeping, begin with auscultation. It is difficult to accurately listen to lungs when a client is crying. If a client is crying, consider ways to reduce this. For example, a newborn/young child will feel safer if the parent/care partner is engaged. You could have a young child play with your stethoscope so that it is familiar, or ask them to take a big breath and pretend they are blowing out birthday candles.
Absence of air entry and stridor are considered urgent situations. You should notify another provider like a physician or nurse practitioner. If you think the stridor is caused by a foreign body that you can quickly remove, do so. Otherwise, follow the steps of the primary survey (check airway patency, measure respiratory rate, work of breathing, and oxygen saturation, assess pulse rate/rhythm, blood pressure, assess level of consciousness). If the oxygen saturations are low, apply oxygen if you are permitted to do so. With the presence of crackles and wheezes or decreased air entry, you should rely on the primary survey to determine whether there is a risk of clinical deterioration. You should also consider whether the wheezing is new onset and could be caused by a severe allergic reaction (i.e., anaphylaxis) and requires immediate intervention. If not, and the client is stable, you can move the head of the bed up to assist with breathing and continue the focused assessment on the respiratory system. Abnormal findings should be reported.
Posterior and Lateral Thorax - Palpation
23
The steps in palpating the posterior and lateral thorax are as follows (see Video 3.6):
1. Begin by using the dorsa of your hands to compare temperature bilaterally from the apex to the bases. Temperature should be equal bilaterally and typically warm to touch.
2. While comparing bilaterally, use the finger pads of your dominant hand, palpate the posterior and lateral thorax from the shoulders and axillary area to the bottom of the thoracic cage for pain, moisture, deformities, masses, swelling, and crepitus.
While doing so:
- Ask the client if they have any pain. Remember to use other words that may resonate with them, such as tenderness. Pain can be associated with many different underlying pathologies, so you should further assess the pain and other related cues that provide information about the pathology and the required intervention.
- Note any moisture.
- Note the location, size, and description (hard, soft) of any deformities, masses, or swelling.
- Note the location of any crepitus. Crepitus feels like a crackling under the skin similar to popping bubble wrap. It is an acute condition related to subcutaneous emphysema in which air shifts out of the lungs and into the subcutaneous tissues as a result of traumatic, surgical, or infectious causes. It usually resolves when the acute condition is treated. However, it is important to monitor the client for any signs of respiratory distress and desaturation and if the crepitus worsens (expands in size across the chest). New onset crepitus should be examined further, and any additional respiratory changes should be assessed. The physician/nurse practitioner should be notified of the findings.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=345#oembed-5
Video 3.6: Palpation of posterior and lateral thorax
3. Assess for tactile vocal fremitus, which is a vibration felt on the chest wall produced by the sounds of vocalization (speech) transmitting through lung tissue. See Video 3.7. This assessment is not commonly performed, but it can provide information about pathological conditions that cause consolidation in the lung tissue (e.g., tumour, pneumonia) or increased amounts of air (e.g., pneumothorax, emphysema). Combined with other potential cues, the findings from this assessment will point to whether further diagnostic testing is required.
- Place the ulnar or palmar surface of your fingers on about three to five locations on each side of the posterior thorax and about three locations on the right lateral thorax and two locations on the left lateral thorax (again, the number of locations depends on the size of the thorax). See Figure 3.13 for the pattern. The ulnar and palmar surface of fingers are used because they are most sensitive to vibrations.
- Begin at the apex of the lungs (near the shoulders) or just under the axilla and continue down to the base of the lungs (at the bottom of the thorax cage).
- Ask the client to say a word that produces a low-frequency sound (e.g., “foodie” or “coin”) each time you place your hands on the thorax. You may need to ask them to speak a bit louder than normal. The best words to have them say are ones that have two vowels within a single syllable because this produces a low frequency. If you are interested, a history of the words used can be found at: https://onepagericu.com/blog/tactile-fremitus-lost-in-translation
- Note the equality of fremitus in comparison from the left to the right side. The vibrations should be equal. The vibrations will be more difficult to feel as you get closer to the bases because you are further away from the larynx.
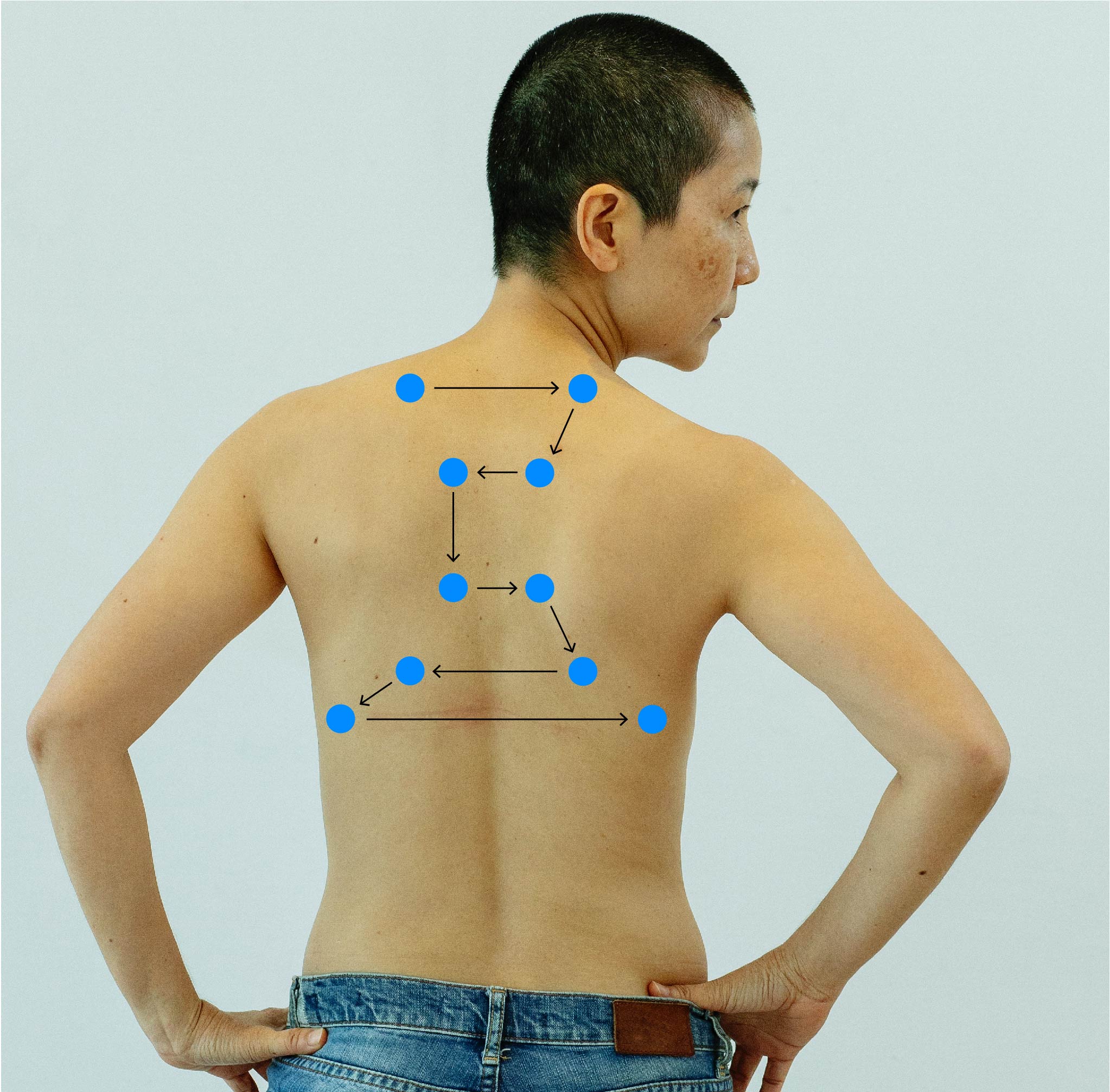
Figure 3.13: Pattern for palpation of tactile vocal fremitus
Photo by Michelle Leman from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=345#oembed-6
Video 3.7: Palpation for tactile vocal fremitus
4. Note the findings
- Normal findings might be documented as: “Upon palpation of posterior chest wall, client reports no pain, temperature warm to touch, equal bilaterally, no moisture, masses, swelling, or deformities, equal tactile fremitus.
- Abnormal findings might be documented as: “Upon palpation of posterior chest wall, client reports pain inferior to scapula at scapula line, a small protrusion noted at same location, temperature warm to touch, equal bilaterally, perspiration noted, equal tactile fremitus.”
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=345#h5p-19
Posterior and Lateral Thorax – Percussion
24
The steps in percussing the posterior and lateral thorax are as follows (see Video 3.8):
1. Ensure the client is in an upright position, and perform indirect percussion to evaluate the elicited sounds.
- The lung is an air-filled organ, so the normal percussion note over the lungs of older children, adolescents, and adults is resonance, which is a low-pitched and hollow sound. With very young children under the age of about 5, you will hear a lower-pitch and booming sound (this is described as hyperresonance).
- Listen for any abnormal percussion notes such as dull notes that can occur when the lung tissue is filled with fluid or solid matter (e.g., a tumour close to the chest wall, pneumonia, pleural effusion, atelectasis) or hyperresonance with lung conditions that lead to hyperinflation of part or all of a lung (e.g., emphysema, pneumothorax). Percussion does not elicit reliable data when a client is overweight or obese because the adipose tissue modifies the normal resonance to a dull note. However, the notes typically don’t change with a client who is underweight. Keep in mind that you should not percuss over ribs or the heart. If you do, the sound elicited over the heart (a dense organ) will be a dull high-pitched sound that quickly stops and over the ribs (composed of bone and cartilage will be a flat high-pitched sound that stops promptly with a very short duration). If abnormal percussion sounds are noted, describe the sound and identify the location. Then, perform a complete focused assessment on the respiratory system and check for other related cues.
2. Percuss in about four to eight locations on each side of the posterior thorax and then at three locations on the right lateral thorax and at two locations on the left lateral thorax. See Figure 3.14 for the percussion pattern. Remember that the number of locations depends on the size of the thorax; less locations are needed on a client with a smaller thorax (e.g., infants). Also remember that the posterior thorax is primarily lower lobes.
3. On the posterior thorax, begin at the shoulders at the scapular line. As you move down the thorax, place your finger close to the vertebral line to avoid percussing over the bone of the scapula. Toward the bottom, percuss close to the vertebral line and then move laterally.
- Avoid percussing over ribs because this will elicit a flat note and does not provide you with any important information. You can rock your finger back and forth to ensure you are in an intercostal space. Typically, you will skip the percussion step when the client has a muscular chest or a lot of adipose tissue as this will modify the normal resonant sound to a flat sound. However, a client who is underweight will typically still have a resonant sound.

Figure 3.14: Percussion pattern for posterior thorax
Image by Claudio_Scott from Pixabay (image was cropped and illustrated upon for the purposes of this chapter)
4. On the lateral thorax, begin percussing inferior to the axilla and percuss in about three locations on the right side and then two locations on the left side (see Figure 3.15).
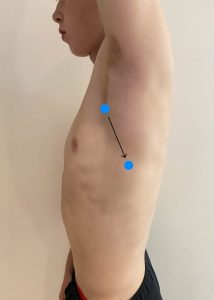
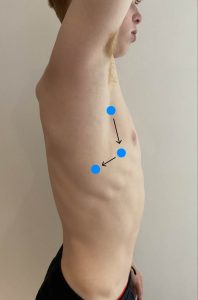
Figure 3.15: Percussion pattern for lateral thorax
5. Note the findings
- Normal findings might be documented as: “Resonance heard through lungs on posterior and lateral thorax.”
- Abnormal findings might be documented as: “Resonance heard throughout except hyperresonance heard in left lower lobe on posterior and lateral thorax.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=347#oembed-3
Video 3.8: Percussion of posterior and lateral thorax (NOTE: percuss down to just below the bottom of the thorax)
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=347#h5p-20
Anterior Thorax - Inspection
25
Inspection of the anterior thorax involves the following steps:
1. Inspect for symmetry, observable deformities, masses, swelling, and shape of the thorax (see Figure 3.16 as a reminder for landmarks).
- Compare the left side of the thorax to the right side of the thorax. Are the clavicles and ribs on each side symmetrical upon observation? Are the ribs sloping downwards? Is the trachea and sternum midline? (note which side, if trachea is deviated [i.e., pulled to one side]).
- Do you notice any deformities, masses, or swelling? (note location and describe)
- Observe the costal angle which is the angle between the costal margins inferior to the xiphoid process. Normally, it is about 90 degrees.
- An abnormal finding is when the angle flattens out. This happens with chronic lung conditions associated with hyperinflation of the lungs (e.g., emphysema). This abnormal finding is often associated with ribs that flatten out and an anteroposterior to transverse diameter that is no longer 1:2, but rather is closer to 1:1 resembling a barrel chest.
2. Inspect for skin colour.
- Is the skin colour consistent across the anterior thorax?
- Do you notice any skin discolouration?
3. Note the findings
- Normal findings might be documented as: “Symmetrical anterior thorax, downward sloping ribs, trachea and sternum midline, no thorax deformities, masses, or swelling, costal angle 90 degrees. Consistent skin colour across anterior thorax, no discolouration”
- Abnormal findings might be documented as: “Tracheal deviation to the right side. Costal angle 170 degrees, horizontal ribs with a 1:1 anteroposterior to transverse diameter.”

Figure 3.16: Anatomical landmarks of thorax
Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
Upon inspection, the findings of most concern are usually a new onset of tracheal deviation or asymmetrical lung expansion. These cues are suggestive of decreased ventilation to one side of the lungs possibly caused by pneumothorax, atelectasis, or pleural effusion. If the client is showing other signs of respiratory distress, notify the physician/nurse practitioner immediately. Otherwise, complete a primary survey followed by a focused assessment of the respiratory system so that you can provide a complete report of the relevant cues to the physician/nurse practitioner.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=349#h5p-21
Anterior Thorax - Auscultation
26
Auscultating the anterior thorax involves the following steps (see Video 3.9):
1. Perform hand hygiene and cleanse the stethoscope.
2. Ensure the client is in an upright position and ask them to take a big breath in and out through the mouth each time they feel the stethoscope on their chest.
3. Place the stethoscope’s diaphragm on the chest in about three to six locations on each side of the anterior thorax so that you listen to all lung lobes. Ensure you have a complete seal. See Figure 3.16 for stethoscope placement pattern. Remember the number of locations depends on the size of the thorax; fewer locations are needed on a client with a smaller thorax (e.g., infants). Also remember that the anterior thorax has more upper lobes and that the right lung has three lobes while the left lung has two lobes.
- On the anterior thorax, begin at the lung apices, which are supraclavicular, moving from one side to the other side. As you move down the thorax, place your stethoscope close to the sternal line to avoid listening over the breast tissue. You may need to ask the client to reposition their breasts to place the stethoscope flat against the thorax. Toward the bottom, listen close to the sternal line and also move laterally.
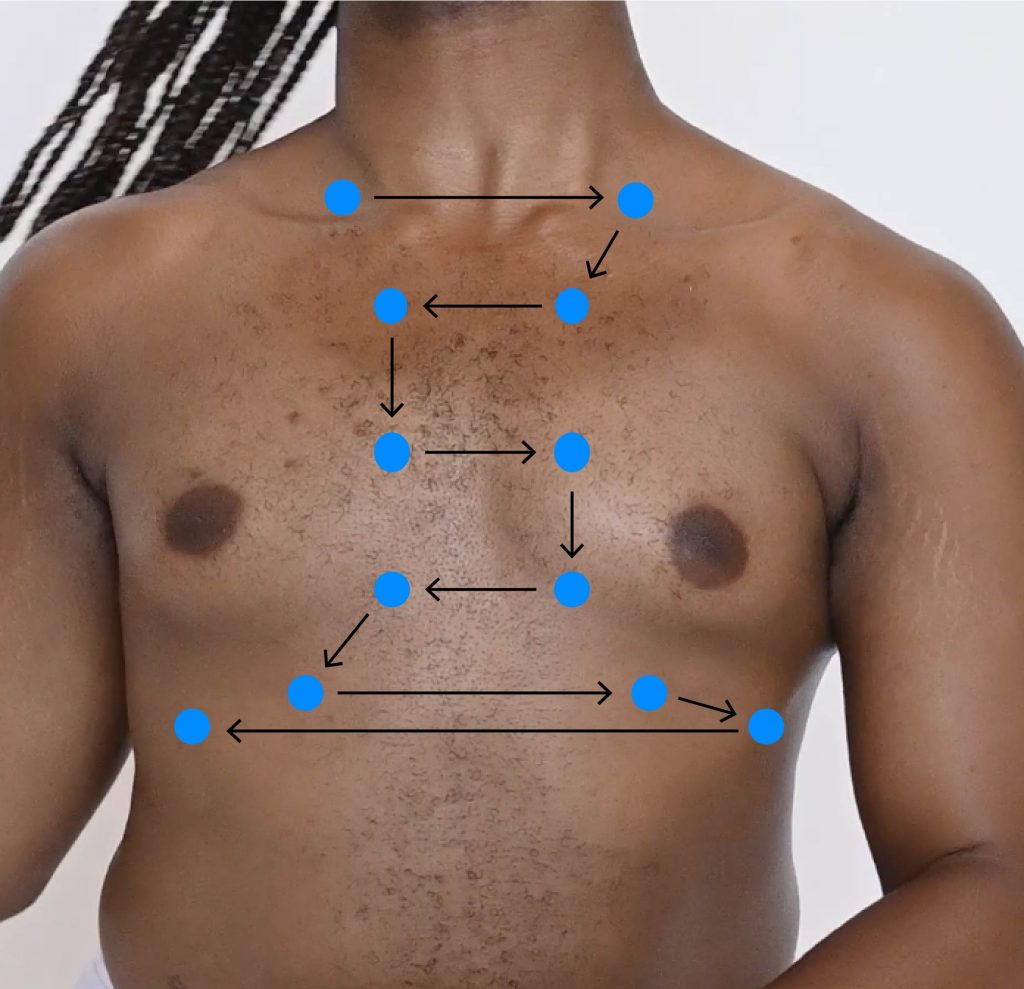
Figure 3.17: Stethoscope placement pattern when auscultating anterior thorax
Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
4. In each location, listen to one full respiration (inspiration and expiration) and compare air entry bilaterally.
5. Listen for the following:
- Air entry quality and equality.
- Quality: Note whether it is good, decreased, or absent.
- Equality: Note whether air entry is equal bilaterally.
- Identify the location of normal breath sounds including bronchial, bronchovesicular, and vesicular.
- If you place your stethoscope over the tracheal region, you should hear bronchial sounds (loud harsh sounds).
- Bronchovesicular breath sounds are moderate in loudness; inspiration is equal to the expiration phase, and heard on the upper thorax close to the sternum and near the bronchi.
- Vesicular breath sounds are quiet and low-pitched; inspiration is longer than the expiration phase, and heard in the periphery of the lung fields and near the smaller airways in an older child and adult. (Note: in young children particularly under two and threes of age, vesicular sounds are typically not heard because of their small thoraxes. Rather, you hear bronchovesicular).
- Identify clear air entry or the presence, quality, and location of any adventitious sounds.
6. Note the findings
- Normal findings might be documented as: “Good air entry, equal bilaterally, no adventitious sounds throughout all lobes on anterior thorax. Bronchovesicular sounds heard in upper lobes close to sternum. Vesicular sounds heard throughout peripheral lung field.”
- Abnormal findings might be documented as: “Absent air entry in right lower lobe anteriorly with mild wheezing heard upon expiration in the upper lobes bilaterally.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=351#oembed-3
Video 3.9: Auscultation of anterior thorax
For a client with breast tissue, you may need to have them reposition their breast so that you can place the stethoscope flat on their chest. This repositioning is also important when you palpate and percuss. It may feel awkward for the client to perform this action, so some nurses demonstrate on themselves over their own uniform to show the client what they would like them to do. Depending on where the breasts are positioned on the thorax, you may need to ask the client to reposition their breasts laterally and up or down. If the client is unable to do so, you may ask permission to reposition their breast. In this case, do so with the ulnar aspect of your hand. Avoid grasping or cupping the breast with your hand as this can be misinterpreted as a sexual motion. Always ask permission and inform the client what you will be doing in order to apply a trauma-informed approach and support the therapeutic nurse-client relationship.
The priorities of care related to auscultation of the anterior thorax are the same as those for the posterior thorax. Absence of air entry and presence of stridor are considered urgent situations: you should call for assistance and notify the physician or nurse practitioner. If you think the stridor is caused by a foreign body that you can quickly remove, do so. Otherwise, follow the steps of the primary survey (check airway patency, measure respiratory rate, work of breathing, and oxygen saturation, assess pulse rate/rhythm, blood pressure, assess level of consciousness). If the oxygen saturations are low, apply oxygen if you are permitted to do so. With the presence of crackles and wheezes, use the primary survey to determine whether there is a risk of clinical deterioration. Also consider whether the wheezing is new onset and could be caused by a severe allergic reaction (i.e., anaphylaxis) and requires immediate intervention. If not, and the client is stable, you can move the head of the bed up to assist with breathing and continue the focused assessment of the respiratory system.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=351#h5p-22
Anterior Thorax - Palpation
27
Palpation of the anterior thorax involves the following steps (see Video 3.10):
1. Begin by using the dorsa of your hands to compare temperature bilaterally from the apex to the bases.
2. While comparing bilaterally, use the finger pads of your dominant hand to palpate the anterior thorax from the apices to the base for pain, moisture, deformities, masses, or crepitus. Avoid palpating over breast tissue. You may need to ask the client to reposition their breasts so that you can palpate the thorax.
While doing so:
- Ask the client if they have any pain.
- Note any moisture or the location, size, and description of any deformities, masses, and swelling.
- Note the location and extent of any crepitus.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=353#oembed-5
Video 3.10: Palpation of anterior thorax
3. Next, assess for tactile vocal fremitus (see Video 3.11).
- Place the ulnar surface of your hands or the base of the palmar aspect of your fingers on about three to five locations on the anterior thorax on each side (see Figure 3.17). Begin at the apex and move down to the base of the lungs.
- Ask the client to say “foodie” or “coin” each time you place your hands on the thorax.
- Note the equality of fremitus in comparison from the left to the right side. Remember that the vibrations will be more difficult to feel as you get closer to the bases because you are further away from the larynx.
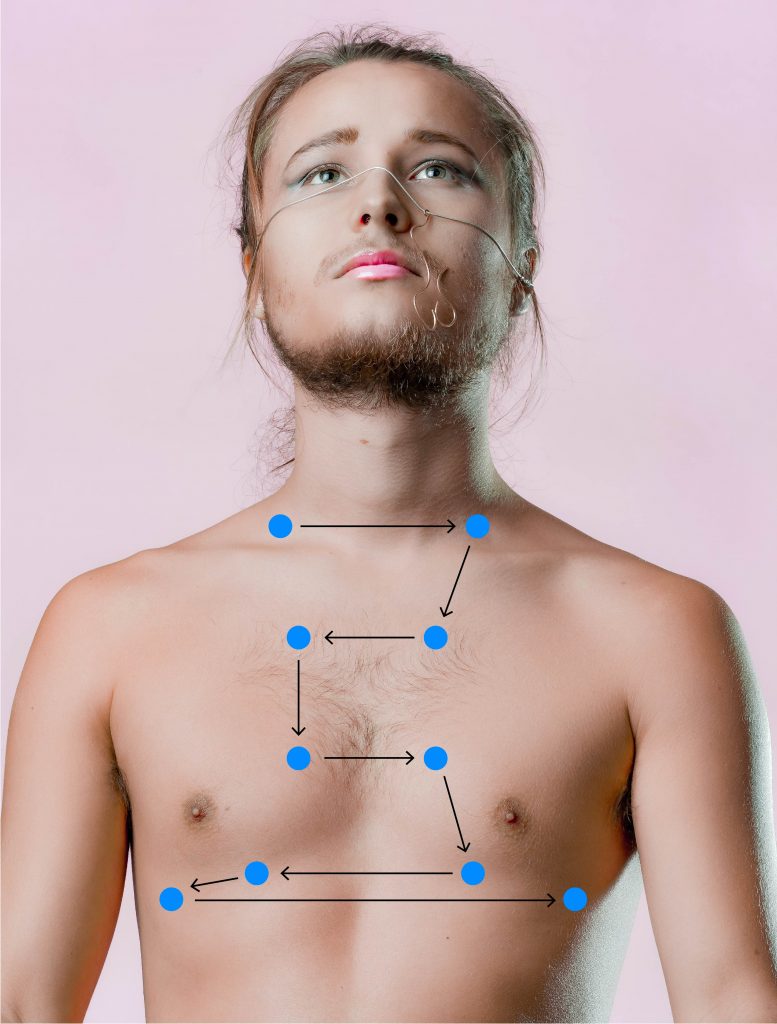
Figure 3.18: Pattern for palpation of tactile vocal fremitus on anterior thorax
Photo by Cottonbro from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=353#oembed-6
Video 3.11: Palpation for tactile vocal fremitus of anterior thorax
4. Note the findings
- Normal findings might be documented as: “Upon palpation of anterior chest wall, client reports no pain, temperature warm to touch, equal bilaterally, no moisture, swelling, masses or deformities, equal tactile fremitus.”
- Abnormal findings might be documented as: “Upon palpation of anterior chest wall, crepitus felt in neck and upper lobe area, perspiration noted.”
Anterior Thorax - Percussion
28
Percussion of the anterior thorax involves the following steps (see Video 3.12):
- Ensure the client is in an upright position, and then perform indirect percussion to evaluate the elicited sounds.
- Percuss in about four to eight locations on each side of the anterior thorax. See Figure 3.18 for the percussion pattern.
- On the anterior thorax, begin at the apices and move down to the bases, comparing side to side. In the supraclavicular region, start at the midclavicular line. As you move inferior to the clavicle, you should shift medially slightly, and then stay close to the sternum to avoid the breast tissue. Toward the bases, percuss close to the sternal line and move laterally.
- Keep in mind that the elicited sound will become dull as you percuss over the heart (second to fifth intercostal space on left side). Also, avoid percussing over breast tissue as this will elicit a dull sound, and avoid percussing over clavicles and ribs because this will elicit a flat note. To avoid the ribs, rock your finger back and forth to ensure you are in an intercostal space. Typically, you will skip the percussion step when the client has a muscular chest or a lot of adipose tissue as this will modify the normal resonant sound to a flat sound.
4. Note the findings
-
- Normal findings might be documented as: “Resonance heard throughout lungs on anterior thorax.”
- Abnormal findings might be documented as: “Dominant sound of resonance heard throughout lungs on anterior side except an area of 3 cm2 on left sternal border between clavicle and second rib.”
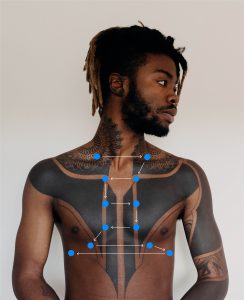
Figure 3.19: Percussion pattern for anterior thorax
Photo by Seyi Ariyo on Unsplash (image was cropped and illustrated upon for the purposes of this chapter)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=355#oembed-3
Video 3.12: Percussion of anterior thorax
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=355#h5p-20
Attribution Statement: The description of percussion and the technique is taken and modified from: https://pressbooks.library.ryerson.ca/ippa/chapter/percussion/
Health Promotion and Disease Prevention: Considerations and Interventions
29
Health promotion and disease prevention are important components of a healthy respiratory system. To determine appropriate interventions, you should carefully consider all of the collected data, both subjective and objective. As part of subjective data collection, you should inquire about risk factors, social determinants, and other considerations.
The inquiry part is integrated throughout the assessment. Many of the probing questions may be asked when doing the subjective assessment. However, some of the questions will be formulated based on your critical reflection of data collected during the subjective and objective assessment. It is this data that will inform your clinical judgment and the health promotion needed for a specific patient.
Handwashing and Immunization: Self-Care Behaviours
Handwashing and immunization are two important factors that affect respiratory health. Regular handwashing is important in healthcare and work settings, when returning home, prior to making and eating food, and before and after elimination.
Probing questions related to handwashing and immunization include:
- Tell me about when you wash your hands?
- What is involved in washing your hands? (You may need to probe further: What are the steps involved? How long do you do it for?)
- Are you up to date on your vaccines?
- When was your last vaccine? What was it for? (You may need to probe about specific vaccines such as influenza [flu], pneumonia, and COVID-19.)
- Have you had tuberculosis testing and when was your last chest x-ray? (You should ask about the results, if relevant). Asking these questions is important part of screening.
You may need to provide education about proper handwashing practices: when and how. Tell the client that it is important to wash hands frequently, but always when leaving a building, returning home, before and after meals, and before and after using the washroom. Tell them to wet their hands with water, lather with soap for 20 seconds, rinse and dry their hands, and then turn off the tap with their elbow or a paper towel. Consider how to make it fun with children: you could tell them to sing a song that lasts 20 seconds (e.g., Happy Birthday).
With regard to vaccines, consider the recommended schedule based on age and region. In Canada, vaccine schedules are determined by provinces and territories. More information can be found at:
https://ecampusontario.pressbooks.pub/immunizations/chapter/recommended-immunization-schedules-in-canada/
If a client is not up-to-date on their vaccines, you should inquire about the reasons why. If a client is vaccine hesitant, explore further in a non-judgmental manner. Respond to their specific concerns with objective facts and refer to vaccines in a positive way. Vaccine hesitancy can be the result of misinformation, so it is important to assess the client’s knowledge and intervene as necessary. Vaccine hesitancy may also be associated with cultural beliefs, and can also be influenced by the client’s relationships with others. More information about vaccine hesitancy can be found at:
https://ecampusontario.pressbooks.pub/immunizations/part/chapter-5-how-to-respond-to-individuals-with-vaccine-hesitancy/
Smoking and Vaping
First-hand, second-hand, and third-hand smoke are major risk factors that negatively affect the respiratory system. The chemicals in smoke cause inflammation of the blood vessels, and contribute to plaque buildup and narrowing of the blood vessels. Prenatal exposure and exposure to smoke as a child has particularly harmful effects. In addition to the risks of respiratory diseases (e.g., asthma), these children are also predisposed to hypoxia and conditioning the brain to nicotine.
More recently, vaping has become common among adolescents and young adults as well as people trying to quit smoking cigarettes. Vaping involves the inhalation of heated aerosols from a vaping device (e.g., electronic cigarettes, vape pens); the aerosols frequently contain nicotine (Miech et al., 2019). Although vaping aerosols may contain less chemicals than cigarettes, there are still many toxins in vaping that can cause lung damage among other health problems (Park et al., 2021).
Probing questions related to smoking and vaping include:
- Do you smoke cigarettes or any tobacco-related products? Do you vape? If the answer is affirmative, ask probing questions: how much do you smoke (how many packs a day)? How many years? Can you tell me about the reasons that you began smoking? (if they vape, you can ask the same questions, but refer to the word they use).
- If you do not currently smoke, have you ever smoked? If the answer is affirmative, ask similar probing questions, including why the client quit.
- If relevant: Have you ever tried quitting? If the answer is affirmative, ask probing questions: What made you want to quit? How long did you quit for? Did you use any strategies to help you quit?
- If relevant: Have you ever thought of quitting? If the answer is negative, respond in a non-judgmental way: “If you ever want to discuss quitting let me know; there are many resources to help you.”
Client interest in quitting smoking/vaping and collaborative intervention are both important for a successful outcome. The intervention must be tailored to the client. Many options are available: counselling, cognitive-behavioural therapy, support groups, pharmacology treatments (e.g., nicotine replacement therapy), smartphone applications, and short text message services. Sometimes even a brief discussion about the risks and a recommendation to quit smoking or vaping is sufficient.
You should consider both relational and structural health promotion approaches related to smoking and vaping. For example, a client’s success in cessation can be affected by their intimate and physically close relationships with family, friends, and work colleagues. Another issue to consider is that access to smoking or vaping cessation resources can be costly and are not necessarily covered by provinces and territories. Many primary care clinics offer group support and counselling at no charge, so it can be helpful to encourage clients to access these resources. You may also advocate for healthy social policy around smoking and vaping cessation and support and participate in the development of educational campaigns and resources about how smoking affects health.
Indoor and Outdoor Pollution
Indoor and outdoor air pollution can affect respiratory health and exacerbate respiratory conditions. They may include motor vehicle emissions, living close to a highway, radon or asbestos in the home, chemicals such as glue, paint, asbestos, and other household or workplace products, and air quality/smog/ozone.
Probing questions related to pollution include:
- Tell me about any indoor and outdoor air pollution you are exposed to?
- Do you have any concerns about how indoor or outdoor pollution is affecting your health?
- Have you noticed that your breathing is affected in any specific indoor or outdoor spaces or on hot days? (Air pollutants and humidity associated with hot weather can aggravate breathing problems).
- Do you wear a mask when using chemicals?
Any client concerns about exposure to pollutants should be addressed. Some clients need education about safe storage and use of chemicals such as household cleaning products, and keeping windows closed and avoiding exercise on days when the outdoor air quality is low. You might recommend hard-surfaced floors or rugs, because carpets can trap pollutants.
Nurses play an important role in the underlying structures that influence healthy environments and pollution. Because the environment has such important effects on health and wellbeing, the Canadian Nurses Association (2017) has developed a position statement about Nurses and Environmental Health. In addition to intervening with actions focused on individual behaviours, nurses can be involved in larger structural approaches involving education campaigns, healthy social policy, and scientific research related to the environment.
Diet
A healthy diet is important for respiratory health because nutrients and hydration are the fuel the lungs need to breathe and function. Water is a main component of the lungs, and water is essential for the delivery of oxygen throughout the body. Normal fluid losses occur with respiration, and hyperpnea increases this fluid loss, so adequate hydration is essential to effective respiratory functioning. A healthy diet is also important to help maintain an ideal body weight. When a person is obese, the lungs work harder to breathe deep because of the excess weight pushing against the thorax.
Probing questions related to diet include:
- Tell me about your usual diet?
- What have you eaten in the last 24 hours? Is that your usual diet?
- How much fluids do you typically drink in a day? What fluids do you drink (e.g., water, caffeinated beverages, alcohol)?
- Do you live in an area where fresh food and drinking water is difficult to access?
- Do you have enough money to buy healthy food?
You may assess a client’s familiarity with Health Canada’s Food Guide (Government of Canada 2021) and discuss how they might draw upon it to guide their food choices: https://food-guide.canada.ca/en/. Be aware that this new guide still has a Eurocentric element to it; you should collaborate with the client about its relevance in the context of their cultural food practices. A snapshot of the guide is now available in dozens of languages: https://www.canada.ca/en/health-canada/services/canada-food-guide/resources/snapshot/languages.html. Many resources have also been developed related to healthy eating and food safety for Indigenous People:
https://www.sac-isc.gc.ca/eng/1581522106156/1581522147811
Some key elements to consider are:
- Water should be the drink of choice: hydration can help keep mucus thin.
- High intake of fruit and vegetable.
- Canada’s Food Guide recommends a dinner plate with half vegetables/fruit, one-quarter protein, and one-quarter whole grains.
Some respiratory-related conditions require specific diets. For example, clients with cystic fibrosis often require increased caloric intake to maintain a healthy weight and enzymes to support the pancreas. In clients with COPD, it is important to also maintain a healthy weight and ensure nutrients such as Vitamin D, C, and E (Berthon & Wood, 2015).
From a structural health promotion approach, consider a client’s access and financial ability to purchase healthy food. These are elements of food security, and the rising cost of food globally has made it difficult to ensure everyone is food secure. In many remote regions of Canada’s North, access to nutritious food is limited in terms of availability, and even when available, the costs are excessive.
Activity
A sedentary lifestyle that involves limited activity/exercise is a risk factor that contributes to respiratory conditions and the overall health of the lungs. Exercise, including aerobic and strength-training, strengthens the lungs and the respiratory muscles, making the lungs more efficient at transporting oxygen.
Guidelines vary based on age and health, but individuals should generally participate in about 30 to 60 minutes of aerobic activity five to seven times per week.
Probing questions related to activity include:
- Do you have any concerns about your level of activity or exercise?
- Tell me about your daily pattern of activity? What activities are you involved in?
- What exercise do you engage in? How long do you engage in this type of exercise? How many days of the week do you participate in exercise? If the client plays sports, ask about their use of protective equipment, if relevant.
Collaborate with the client to create an activity/exercise care plan that is specific to their needs and goals. Start at a realistic and attainable level, depending on the client’s physical capabilities and energy level, and then begin to increase the time and duration of the physical activity. Many interventions are available to support clients to achieve their activity goals: community walking groups, fitness apps, and joining a local gym or group activity. The participACTION website is a helpful resource related to activity guidelines: https://www.participaction.com/en-ca. Consider activity interventions from a structural health promotion approach, considering the financial costs associated with many of these resources.
Stress and Distressing Emotions
Stress and distressing emotions are subjective and can affect a person physically, mentally, socially, and financially.
Stress and other negative emotions affect the respiratory system. Stressful states such as anxiety and anger stimulate the sympathetic nervous system and stimulate the body to breathe faster. This can exacerbate existing respiratory conditions such as asthma.
Probing questions related to stress and negative emotions include:
- Tell me about any stress that affects your breathing? Have you had anxiety or panic attacks affect your breathing? If the client’s answer is affirmative to either question, probe further with questions such as:
- Tell me more?
- How does it affect your breathing?
- How often do you experience this?
- What do you do when you experience this?
When considering interventions for a client, consider their daily patterns of living and any disruptions to these patterns, which can be stressful.
Various strategies can help reduce stress, including:
- Engaging in regular physical activity.
- Getting adequate sleep.
- Spending time with family and friends.
- Taking time for personal interests and hobbies.
- Practicing relaxation techniques such as meditation, deep breathing exercises, and tai chi.
- Using pursed lip breathing techniques: this involves taking a slow deep breath in through the nose for two counts and then pursing the lips while breathing out for four counts. It helps with stress and also increases oxygenation and reduces carbon dioxide.
Use relational and structural health promotion perspectives to further assess a client’s stress and how best to act. Stress does not exist in a vacuum: how it is experienced, perceived, and managed is affected by relationships with others. All clients occasionally experience stress, but structural aspects influence how a client may be more at risk for stress. For example, racism is a major determinant that leads to highly stressful experiences, so use of an anti-racist approach to stress and stress management will help you understand how the client is influenced and how best to support them. Other determinants of health related to socioeconomic status can influence access to resources to cope with stress. When collaborating with clients to develop stress management techniques, you must be aware of these broader structural influences.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=357#h5p-23
References
Berthon, B., & Wood, L. (2015). Nutrition and respiratory health feature review. Nutrients, 7(3), 1618-1643. https://doi.org/10.3390/nu7031618
Canadian Nurses Association (2017). Nurses and environmental health. https://www.cna-aiic.ca/~/media/cna/page-content/pdf-en/nurses-and-environmental-health-position-statement.pdf
Government of Canada (2021). Canada’s food guide. https://food-guide.canada.ca/en/
Miech, R., Johnston, L., O’Malley, P., & Bachman, J. (2019). Adolescent vaping and nicotine use in 2017-2019 – US national estimates. New England Journal of Medicine, 380(2), 192-193. https://doi.org/10.1056/NEJMc1814130
Park, J., Alexander, L., & Christiani, D. (2021). Vaping and lung inflammation and injury. The Annual Review of Physiology, 84(18). https://doi.org/10.1146/annurev-physiol-061121-040014
Clinical Judgment – Case Study
30
A 13-year-old client comes to the emergency department with breathing difficulties. The client is accompanied by their father, and has a history of asthma, diagnosed four years ago. On arrival, the client’s symptoms include increased work of breathing, shortness of breath, coughing and wheezing. Vital signs: respiration rate: 30 breaths per minute, heart rate: 118 beats per minute, O2 saturations: 91%, blood pressure: 110/60 mm Hg, and tympanic temperature: 38.1ºC. The client reports the symptoms are not related to usual triggers (e.g., overexercising, playing in cold air, scented products). The father says the child was up all night coughing and is therefore very fatigued this morning. Upon auscultation, decreased air entry bilaterally to bases, wheezing in the upper quadrants. No accessory muscle tugging. The client states their chest feels tight when coughing and that they started to feel nauseous this morning. Diaphoresis noted on face and neck areas. Slight grey discolouration around lips.
Watch the following 5-minute video to learn more about how asthma works with your respiratory system: https://youtu.be/PzfLDi-sL3w
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=359#h5p-24
- Common symptoms to assess related to the respiratory system include dyspnea, coughing, wheezing, congestion, and chest pain.
- The objective assessment of the thorax is best performed on the client in an upright position on the bare skin.
- A trauma-informed approach to the objective assessment is necessary considering that areas of the chest are being exposed.
- The objective assessment should begin with a brief scan combined with components of the primary survey so that potential signs of clinical deterioration are recognized and acted upon.
- Following the brief scan, the objective assessment includes inspection, auscultation, palpation, and percussion.
- Health promotion interventions should be developed with the client to address what is important to them.
Chapter 4 - Cardiovascular System
IV
By Dr. Jennifer Lapum, Michelle Hughes, Mahidhar Pemasani, Paul Petrie, Sita Mistry, and Siobhan Doyle
- Apply subjective assessment skills.
- Apply objective assessment skills.
- Use clinical judgment.
- Integrate health promotion interventions into actions.
- Integrate an inclusive approach to cardiovascular assessment.
Introduction to the Cardiovascular System
The cardiovascular system is important because it is responsible for the provision of blood, oxygen, and nutrients to the body’s tissues and organs. If this system is not working properly, it provides sub-optimal perfusion of these elements to body tissues. Lack of perfusion can affect all body systems and tissues as a result of pathophysiological processes related to hypoxemia, hypoxia, and electrolyte imbalances. As a nurse, your assessment of the cardiovascular system provides information about the functioning of this system and potential cues that require your action.
Cardiovascular System Components
The main components of the cardiovascular system include:
- The heart (two atriums, two ventricles, and four valves).
- The main vessels (aorta, pulmonary artery, pulmonary vein, and superior and inferior vena cava).
- The coronary arteries.
- The carotid arteries and jugular veins (typically considered part of the peripheral vascular system but also included in this chapter). See Figure 4.1.
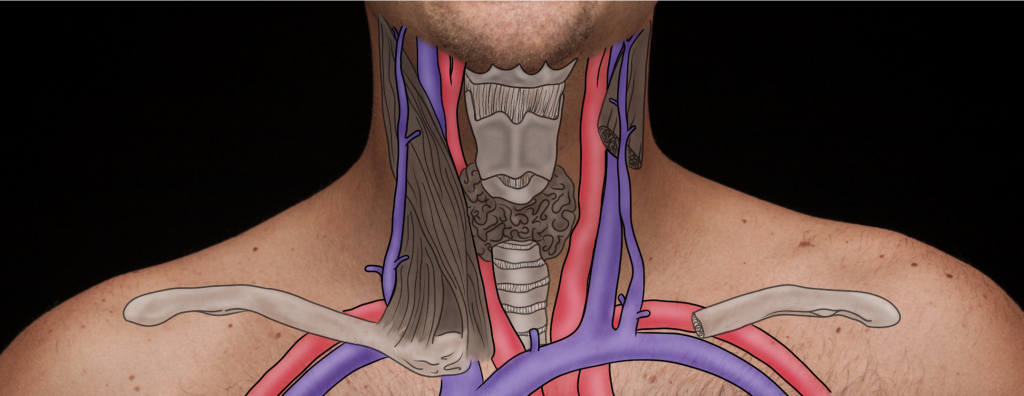
Figure 4.1: Carotid arteries and jugular veins
Photo by engin akyurt on Unsplash (image was cropped and illustrated upon for the purposes of this chapter)
You have probably already learned about the anatomy and physiology of the heart; see Video 4.1 for is a quick overview of how the heart works:
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=30#oembed-3
Video 4.1: Overview of how the heart works
The cardiovascular system is interconnected and influences many other body systems, so it is rarely assessed in isolation. When nurses are attempting to make sense of the cues that are relevant and of concern, they commonly assess other body systems: respiratory, peripheral vascular, and skin.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=30#h5p-25
Subjective assessment of the cardiovascular system involves asking the client about their health and symptoms that might be related to pathologies that affect the heart. A full exploration of these pathologies is beyond the scope of this chapter, but common cardiovascular diseases and conditions include hypertension, coronary artery and valvular diseases, heart rhythm disorders, heart failure, and congenital or acquired structural diseases of the heart.
Common symptoms or cues that may be related to the cardiovascular system include pain, dyspnea, arrhythmias, coughing/wheezing, and edema. See Table 4.1 for guidance on the subjective health assessment. Many of the questions in this table align with the PQRSTU mnemonic. Probing of these symptoms is done in the order of relevance, as opposed to being sequentially aligned with the PQRSTU mnemonic.
You should also ask about any medications the client is taking: name, dose, frequency, reason it was prescribed, and how long they have been taking it.
You should also include questions focused on health promotion. Depending on the context, you may ask these questions and engage in a discussion during a subjective assessment or after an objective assessment. A section on “Health Promotion Considerations and Interventions” is included later in this chapter after the discussion of objective assessment.
Many common cardiovascular symptoms are related and are caused by the same issue. For example, pain associated with the heart is often related to cardiac ischemia, which is commonly caused by atherosclerosis of coronary arteries as well as other conditions such as cardiac valve disease, heart failure, and pericarditis. When tissue such as the cardiac muscle does not receive sufficient oxygen-rich blood, this can lead to chest pain, dyspnea, and fatigue. Other common cardiac symptoms, such as fatigue, shortness of breath, and chest pain, can sometimes be related to valve stenosis/prolapse.
Table 4.1: Guidance on the subjective assessment
|
Symptoms
|
Questions
|
Clinical Tips
|
|
Cardiac pain refers to pain associated with the heart and can be described in many ways such as crushing, pressure, squeezing, tightness, and heaviness in the chest. It is often referred to as chest pain.
It can sometimes be confused with heartburn, but the etiology and treatment of both are different. Therefore, subjective questions are needed to differentiate between these.
Cardiac pain may be felt in the chest, but also in other locations such as the jaw, neck, arms particularly the left arm, upper back, and abdomen. This type of referred pain occurs because of the sharing of neural pathways.
|
Do you have pain in your chest? Have you ever experienced pain in your chest?
Additional probes if the response is affirmative:
Region/radiation: Where is the pain located? Does it move around or do you feel it anywhere else?
Quality/quantity: Can you describe what it feels like? How bad is it?
Severity: Can you rate it on a scale of 0 to 10, with 0 being no pain and 10 being the worst pain you have had?
Timing/treatment: When did it begin? What were you doing when it began? Is it constant or intermittent? Have you tried treating it with anything?
Provocative/palliative: What makes it worse? Is it worse when you are breathing deeply? Does it occur after eating? What makes it better?
Understanding: Do you know what is causing the pain?
|
Apply a cultural humility approach when you consider the meaning of “pain.” Some people may reserve the word to describe severe sensations, so if their symptom is mild they may not refer to it as pain. Others may associate pain with vulnerability and use alternative words to describe it. Therefore, if the response is initially “no,” try rephrasing the question using words such as discomfort, tenderness (e.g., Do you have any sensations in your chest?).
Pain of cardiac origin is a critical finding and requires immediate action. It is considered a first-level priority of care. You should ask a colleague to notify the physician while you keep the client at rest, assess pulse, blood pressure, and oxygen saturations. Depending on the setting and if appropriate, adhere to existing directives such as order an electrocardiogram and blood work, administer oxygen, initiate intravenous, and give nitroglycerin and morphine. If you are in a home setting and/or do not have access to these treatments, the client can chew and swallow acetylsalicylic acid (usually low-dose ASA, 81 mg); this can be helpful to prevent the enlarging of the blood clot.
|
|
Dyspnea refers to difficulty breathing and can be described as shortness of breath, a feeling of breathlessness, not being able to get sufficient air or catch your breath.
|
Do you have any difficulty breathing? Have you experienced any difficulty breathing?
Additional probes if the response is affirmative:
Quality/quantity: What does the difficulty in breathing feel like? How bad is it?
Provocative/palliative: Is there anything that makes your breathing worse? Is it worse when you are lying down? Is there anything that makes your breathing better? Does it feel better when you are sitting up?
Severity: Can you rate your difficulty breathing on a scale of 0 to 10, with 0 being no difficulty breathing and 10 being the most difficulty breathing you have had?
Timing/treatment: When did the difficulty in breathing begin? Have you treated it with anything?
Understanding: Do you know what is causing it?
|
People find the sensation of not being able to catch their breath particularly disturbing because it feels like they are suffocating.
As you are assessing the client, consider raising the head of the bed to make it easier for them to expand their lungs and breathe more easily. However, this decision may be influenced by whether the client’s condition is stable. If they are showing signs of clinical deterioration and their blood pressure is low, lower the head of the bed to increase the amount of blood returning to the heart.
Assess the client’s respiration rate, breathing effort, oxygen saturation, and then assess pulse, blood pressure, and temperature, followed by auscultation of lungs.
|
|
Arrhythmias refer to irregular heart rhythms such as tachycardia or bradycardia.
These arrhythmias can feel like the heart skipping a beat, a palpitation, or a fluttering of the heart.
|
Do you have any fluttering of your heart or palpitations? Have you ever experienced any fluttering of your heart or palpitations?
Additional probes if the response is affirmative:
Timing: What were you doing when it started? Is it constant or intermittent?
Provocative: Is it worse when you are feeling stressed or anxious?
Other: Do you have any other associated symptoms (dizziness, difficulty breathing, sweating, pain, blurred vision)?
|
Perform a primary survey if you are concerned about clinical deterioration.
Assess apical pulse rate and rhythm and blood pressure.
|
|
Coughing or wheezing are common symptoms of heart disease particularly when it affects the lungs. In individuals with heart failure, the blood can back up into the lungs, affecting breathing. Fluid can leak into the lungs causing congestion. Depending on the cause, the client may have expectorate (sputum production from coughing) or hemoptysis (sputum that has blood in it).
|
Do you have any coughing or wheezing? Have you experienced any persistent coughing or wheezing recently?
Additional probes if the response is affirmative:
Timing: When did the coughing and/or wheezing begin? How often are you coughing and/or wheezing?
Quantity: How bad is the coughing and/or wheezing?
Other: Do you have any mucus production when coughing? If so, what colour is it?
Provocative/palliative: Is there anything that makes the coughing and/or wheezing better or worse?
|
Until the origin is ruled out, consider it transmissible. You and the client should both wear a mask. Additionally, you should consider putting on a face shield.
Follow a process similar to one you would use for a client with dyspnea.
|
|
Peripheral edema is swelling that occurs from excess fluid in the tissues. When it is cardiac-related, it is usually caused by the heart not pumping adequately and blood backing up causing swelling. It is most easily noticed in peripheral locations such as the feet and legs because gravity pulls the fluid downward into these dependent position, but it may also be observed in the sacrum, abdomen, hands, and arms.
|
Have you noticed any swelling or puffiness in your feet or ankles (or any other areas)? Have you noticed that your shoes fit tight on your feet?
Additional probes if the response is affirmative:
Region: Where is the swelling?
Timing: When did the swelling begin? Is the swelling worse at a particular time of day?
Provocative/palliative: Does anything make the swelling worse or better?
Other: Have you noticed any associated colour changes to the skin? Do you have difficulty walking? Have you noticed any skin ulcers on your feet or legs? Do you have increased urination at night? Have you noticed a recent and rapid weight gain in the last week?
|
Assess whether the edema is acute or chronic and unilateral or bilateral. This will help you focus your questioning. If it is acute and unilateral, it may be a localized issue such as deep vein thrombosis (DVT) or an injury. If it is chronic and bilateral, it is more likely to be a systematic issue such as heart failure.
Nocturia and edema are often related symptoms. At night when a person lies down, gravity no longer retains the fluid in the peripheries. As a result, the fluid returns to the veins and some is filtered by the kidneys, producing an increase in urine. Since blood is returning to the veins and being pumped to the heart, the edema can also lessen.
Edema and rapid weight gain are also sometimes related. Rapid weight gain can be suggestive of increased fluid retention (leading to edema) and is often associated with heart failure. A 2–3 lb (.9 to 1.3 kg) weight increase in 24 hours is a cue that requires immediate action.
Complete a focused assessment on respiratory, cardiovascular, peripheral vascular, and skin.
|
|
Other cardiovascular related symptoms can include fatigue, light-headedness, diaphoresis, nausea, decreased appetite, and colour changes such as cyanosis.
|
Always ask one question at a time.
Have you experienced fatigue (light-headedness, sweating, nausea, decreased appetite, skin colour changes)?
Use variations of the PQRSTU mnemonic to assess these symptoms further if the client’s response is affirmative.
|
These symptoms can be related to other body systems and non-cardiac issues. Therefore, it is important that these symptoms be explored specifically if there were affirmative responses to the other common cardiac-related symptoms.
|
|
Personal and family history of cardiovascular issues. These may include risk factors, conditions, and diseases.
|
Do you or your family members have high blood pressure or high cholesterol? Have you or your family members ever had a heart attack? Do you or your family members have heart failure? Do you or your family members have any issues associated with the valves of the heart? Are you aware of any other personal or family history of cardiac issues that I may have not mentioned?
Additional probes if the response is affirmative include further exploration using the PQRSTU mnemonic. Also ask about age of diagnosis, and if relevant, age of death of family members.
|
The biological and non-biological nature of family may be important to explicate when asking questions, considering that the risk factors may be influenced by genetics and/or culture. Although there is a genetic role to some cardiac conditions and diseases, it is also important to consider culture in terms of family traditions and practices have a large role to play (e.g., eating habits, activity/exercise, smoking). With some clients who have high cholesterol, there can be a genetic component leading to familial hypercholesterolemia. This is an inherited condition (the gene is present at birth) that leads to hypercholesterolemia (high levels of cholesterol in the blood). Thus, the age that a person or their family member develops hypercholesterolemia as well as hypertension is important to assess.
It is important to inquire about high blood pressure in current or past pregnancies. High blood pressure can be associated with complications for the women and the fetus. Thus, it is measured at each prenatal care visit.
|
Many cardiovascular symptoms are cues for action. Chest pain could signify angina, which requires immediate action: failure to do so could result in a myocardial infarction (heart attack). Acting quickly when a client has angina can reduce cardiac muscle damage and prevent death. In this case, all of the following actions are important:
- Notify the physician/nurse practitioner.
- Take the client’s vital signs: pulse, respirations, blood pressure, and oxygen saturation.
- Keep the client at rest, preferably lying in bed in case they deteriorate.
- If you have standing orders in your healthcare setting, you may also apply oxygen, order an electrocardiogram (ECG) and bloodwork, give morphine intravenously, and provide the prescribed/protocol dose nitroglycerin spray.
Angina and other symptoms (shortness of breath, arm numbness, change in vision) may be associated with a condition called hypertensive crisis, in which the blood pressure is extremely high (greater than 180/110 mm Hg). This requires immediate intervention because it can lead to severe consequences (myocardial infarction or stroke). Therefore, you should notify the physician/nurse practitioner and continue to monitor vital signs and additional cues. In addition, it is vital to monitor blood pressure and pulse with any cardiac-related symptoms. See further information about high blood pressure and hypertension here: https://pressbooks.library.ryerson.ca/vitalsign2nd/chapter/hypertension/
Currently, there is a gender bias related to recognizing and acting on this angina promptly; as a result, women’s health outcomes are negatively affected. Some of the reasons underlying this issue are systematic, particularly in terms of the perception that heart disease is a man’s issue, as well as physiological and cultural differences in how pain presents in women and limited clinical trials and research focused on women.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=366#h5p-26
Objective assessment of the cardiac system includes assessing the carotid arteries, the jugular veins, and the heart.
Typically, you will complete an objective assessment after the subjective assessment, but in urgent situations, objective assessment and associated interventions may become the priority of care.
Remember to do all assessments on bare skin.
A trauma-informed approach to cardiac assessment is important because areas of the chest will need to be assessed and exposed. Maintain privacy by closing the door and/or curtains. Ask the client if they would like a family member or friend present or another healthcare provider. Provide a drape to the client and only expose the necessary areas of the chest. Always ask permission to touch. And last, explain what you are doing throughout the assessment. Sometimes it is helpful to show on your own chest (over your uniform) where you will be palpating and placing the stethoscope.
Contextualizing Inclusivity – Chest Binding
An inclusive approach to health assessment is vital because clients need to feel accepted for who they are. Some non-binary and transmasculine clients may wear a chest binder because they feel uncomfortable or distressed about having breast tissue. Binders are garments designed to flatten the appearance of the chest wall. They come in different forms and can extend from the chest down to the diaphragm or to the hips: they may look like a sports bra or tank top, and some clients may use compression bandages.
The binder needs to be removed to adequately assess the heart. You may or may not be aware of whether the client you are assessing wears a chest binder, so you can apply an inclusive approach by acknowledging the vulnerability that clients may feel. Provide step-by-step instructions so that they are prepared, and ask non-judgmental questions like “Assessing your heart requires me to assess on the bare skin of your chest. Is there anything that would impede me from doing so?” You can also ask if they have any questions before beginning.
You should also assess the binder for proper fit: a good fit allows for normal chest expansion and deep breathing.
Assessment of the carotid arteries involves auscultation followed by palpation. This assessment provides information about cardiac function and the quality of blood flow through the artery.
Unobstructed blood flow is silent, whereas partial obstruction of blood flow (due to carotid stenosis) creates turbulent blood flow, leading to vascular sounds. These sounds are called bruits: blowing/swooshing noises. Following auscultation, if you do not hear bruits, proceed to palpating the carotid pulses. Be aware that complete obstruction of blood flow will also be silent, as there is no blood flowing through the artery.
This assessment is done in the seated position or in the high-fowlers position with the client looking straight ahead. Make sure they do not flex or extend their neck.
Auscultation of Carotid Arteries
1. Cleanse the stethoscope. See Video 4.2.
2. Ask the client to breathe in, breathe out, and then hold their breath.
- This is important because normal tracheal breath sounds can resemble a bruit and limit the nurse’s ability to hear the bruit. Note that some clients are unable to hold their breath for long: tell them to breathe if they feel they need to or if they become lightheaded.
3. With light pressure, place the stethoscope’s bell over the right carotid artery in the middle third of the neck, just medial to the sternomastoid muscle, but closer to the muscle than the trachea. This location is anatomically determined, see Figure 4.2.
- The bell should be used because vascular sounds are low-pitched.
- Usually, listening at one location on each side of the neck is sufficient. Some practitioners listen to three locations on the neck, but this is usually not needed because sound radiates. If you have concerns, you can listen to three locations on each side of the neck: at the base of the neck closer to the origin of the carotid artery; in the middle third of the neck just medial to the sternomastoid muscle, but closer to the muscle than the trachea; and inferior to the angle of the mandible.
4. Repeat the steps two and three on the left carotid artery.
5. Note the findings
- Normal findings might be documented as: “No carotid bruit present, bilaterally.”
- NOTE: You may hear the beating of the heart because sound travels.
- Abnormal findings might be documented as: “Carotid artery bruit present” (on left or right side or bilaterally).
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=370#oembed-5
Video 4.2: Auscultation of the carotid arteries
Do NOT palpate the carotid artery if you hear a bruit when auscultating the carotid arteries. A bruit can be a critical finding and is suggestive of carotid stenosis and partial obstruction of the artery. It is therefore important to not palpate (compress the artery) when the blood flow is already compromised. You should measure the client’s vital signs (specifically pulse, blood pressure, oxygen saturation, respiration) and continue the cardiac assessment. Then, report your findings to the physician/nurse practitioner.
Palpation of Carotid Arteries
1. First, if you hear a bruit when auscultating the carotid arteries, do not palpate the carotid artery. Only proceed with palpation if you do not hear a bruit. See Video 4.3.
2. Place the pads of your three fingers gently over ONE carotid artery (right or left) in the middle third of the neck, just medial to the sternomastoid muscle. Then, repeat on the opposite artery.
- Do NOT palpate the left and right carotid arteries at the same time, because this can compromise blood flow superior to the location you are palpating (the brain).
- Do NOT place the pads of your finger high on the neck, because this area is the location of the baroreceptors of the carotid sinus. These receptors are medial to the sternomastoid muscle, inferior to the angle of the jaw, and just superior to the thyroid cartilage. They play a role in mediating heart rate and blood pressure, and increased pressure on this area can lead to bradycardia and a drop in blood pressure.
3. Palpate for the following:
- Force (strength of pulsation). Pulse force is recorded using a four-point scale:
-
- 3+ Full, bounding
- 2+ Normal/strong
- 1+ Weak, diminished, thready
- 0 Absent/non-palpable
(Adapted from: Vital Sign Measurement Across the Lifespan, 2nd Canadian edition)
- Symmetry (compare force between left and right side).
- Quality (describe the pulsation) in terms of the wave form. The carotid pulsation is described as a quick upstroke (one cursory/brisk outward movement felt against your fingers) and a slow downstroke (a more gradual inward movement away from your fingers).
4. Note the findings
- Normal findings may be documented as: “2+ carotid pulsation equal bilaterally, smooth contour with a quick upstroke and gradual downstroke.”
- Abnormal findings may be documented as (example): “1+ carotid pulsation bilateral with dicrotic upstroke and gradual downstroke” (reduced amplitudes can be common in conditions with low stroke volume, while dicrotic upstrokes can be common with increased peripheral vascular resistance, for example in situations of heart failure).

Figure 4.2: Carotid artery anatomy
Photo by engin akyurt on Unsplash (image was cropped and illustrated upon for the purposes of this chapter)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=370#oembed-6
Video 4.3: Palpation of carotid arteries
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=370#h5p-33
Assessment of the jugular veins involves inspection of the pulsation. This assessment is performed because it provides information about the central venous pressure (CVP), which is the pressure in the vena cava near the right atrium and is an estimation of the right atrial pressure. Assessment of the CVP provides information about fluid status and functioning of the right ventricle.
When inspecting the jugular veins, you are noting whether there is elevated CVP as reflected by distention of the veins in the neck. Elevated CVP can be indicative of fluid retention, right ventricle contractile dysfunction that can be associated with heart failure, pericarditis, pulmonary hypertension, and tricuspid stenosis. Low CVP can be indicative of volume depletion (e.g., hemorrhage, dehydration).
You can assess CVP and other heart pressures with an invasive procedure called pulmonary artery catheterization. However, this would only be done in intensive care when the client is critically ill. A non-invasive way to assess the CVP is by inspecting the jugular veins
Inspection of Jugular Veins
1. Assist the client into a supine position with the head of bed in a position at least 30 degrees and no higher than 45 degrees. See Video 4.4.
- With normal CVP (not elevated), the jugular pulsation will not be visible if you raise the head of the bed to 90 degrees. With severely elevated CVP, you can raise the head of the bed to 90 degrees and still see the jugular pulsation.
2. Remove the client’s pillow so their head is laying flat against the bed in a neutral position. You may leave the pillow if it is flat (not fluffy). The important point is that the head, neck, and thorax are on the same plane and the neck is not flexed.
3. Stand on the right side of the bed and ask the client to gently turn their head to the left.
- It is assessed from the right side because the right jugular vein is more directly attached to the superior vena cava leading to the right atrium.
4. Use tangential lighting to highlight pulsations.
5. Begin by inspecting the right external jugular pulsation, as it is most visible. The vein should be flat or not visible; a bulging vein can suggest high CVP.
- The vein is superficial to the sternomastoid muscle and runs from anterior to the mastoid process to the medial portion of the clavicle. As it moves down to the clavicle, it becomes lateral to the sternomastoid muscle and then turns 90 degrees to join the superior vena cava. See Figure 4.3 as a reminder of the anatomy.
6. Next, inspect the right internal jugular pulsation at the sternal notch, the base of neck supraclavicular area, and up the neck as needed. The right internal jugular pulsation provides the most accurate assessment of the CVP because it attaches more directly to the superior vena cava. Note the location and the wave quality.
- A normal jugular pulsation is visualized around the sternal notch or the supraclavicular area. (The right internal jugular vein is underneath the sternomastoid muscle and runs from anterior to the mastoid process to the medial portion of the clavicle. It begins medial to the muscle at the mastoid process and then runs underneath the muscle as it moves down to the clavicle)
- The wave quality of a normal jugular pulsation is a double wave that is diffuse (diffuse means that it is spread out as opposed to in a pinpointed areas).
NOTE: Do not confuse the carotid artery pulsation with jugular venous pulsation. See Figure 4.3.
7. Note the findings
- Normal findings may be documented as: “Right external jugular vein is flat with no distension. Double diffuse pulsation of right internal jugular vein at sternal notch.”
- Abnormal findings may be documented as: “Bulging right external jugular vein. Accentuated double pulsation of right internal jugular vein just inferior to the ear lobe.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=372#oembed-3
Video 4.4: Inspection of the jugular pulsation
It is important to ensure your assessment is focused on the jugular pulsation and not the carotid pulsation. Unlike the carotid pulsation, the jugular pulsation varies with a person’s breathing, it is not palpable, and is not visible when the client is sitting upright unless they are experiencing severe distention. Additionally, the carotid pulsation is visualized as one quick wave in a specific area as opposed to a double diffuse wave.
A distended/bulging jugular vein (see Figure 4.4) is a critical finding in which blood is backing up from the right side of the heart/superior vena cava into the jugular veins; there are many causes such as heart failure, pulmonary hypertension, and tricuspid valve stenosis / prolapse. It is typically associated with other cues such as heart palpitations, chest pain, tachycardia, perspiration, and dyspnea, and other signs of respiratory distress. The priority of care related to this cue is determining the cause and keeping the client stabilized. In addition to notifying the physician/nurse practitioner, you should continue monitoring the client’s vital signs (specifically: pulse, respiration, blood pressure, oxygen saturation) and continue the assessment with a focus on cardiac inspection, palpation, and auscultation. It is important to auscultate the valves to determine the quality of blood flow and presence of murmurs.

Figure 4.3: Jugular vein anatomy
Photo by engin akyurt on Unsplash (image was cropped and illustrated upon for the purposes of this chapter)
Figure 4.4: JVD by Ferencga is used under a Creative Commons Attribution-Share Alike 3.0 Unported license. (taken from: https://pressbooks.bccampus.ca/clinicalproceduresforsaferpatientcaretrubscn/chapter/2-8-head-to-toe-assessment-cardiovascular-assessment/)
Jugular venous pulsation is influenced by blood volume, cardiac function of the right ventricle, and venous compliance. Any condition that causes an increase in right atrial pressure can lead to elevated CVP such as fluid overload, heart failure, pulmonary hypertension, and valve abnormalities (e.g., pulmonic stenosis).
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=372#h5p-34
Assessment of the heart involves inspection, palpation, and auscultation. Always begin with inspection, unless there is an immediate concern to move to auscultation or you suspect clinical deterioration.
The assessment must be performed on skin and never over clothing. You may ask the client if they would like someone present for the exam; some clients may not feel comfortable exposing their chest area and may prefer the presence of a friend, family member, or another healthcare provider.
You should always explain what you are doing and ask permission to touch. Always ensure the client’s privacy. Close the door and curtains and provide appropriate draping, considering that some of the assessment involves exposing parts of the chest. Draping should be provided to clients of all genders and ages.
The assessment is typically performed in a supine position with the client’s head on a pillow. This positioning also facilitates draping and easier landmarking, particularly with a client who has larger breasts that will need to be repositioned to expose assessment areas. For example, repositioning will be easier as larger breasts typically shift laterally in a supine position. You can ask the client to shift their breast tissue laterally and up or down as needed; if the client is unable to do so, you can ask permission to reposition their breast. In this case, always use the ulnar (outside) surface of your hand, as opposed to a grasping or cupping movement.
When performing an objective assessment, you will need to physically landmark several locations on the chest to inspect and palpate the precordium, palpate the apical impulse, and auscultate the apical pulse and cardiac valves. See Figure 4.5 and Video 4.5. The physical location where you assess is not always aligned with the anatomical location. For example, auscultation of cardiac valves corresponds with the direction of blood flowing out of the valve as opposed to where the valve is anatomically located.
2nd Intercostal space at right sternal border: Location of where the aortic valve is best heard because the flow of blood out of the valve is directed toward this area. This is also the location of the base of the heart.
2nd Intercostal space at left sternal border: Location of where the pulmonic valve is best heard because the flow of blood out of this valve is directed toward this area. This is also the location of the base of the heart.
5th Intercostal space at left sternal border (or 4th intercostal space in a child): Location of where tricuspid valve is best heard because the flow of blood out of this valve is directed toward this area. Note that in a child, this is located at the fourth intercostal space. Some practitioners assess the 4th intercostal space even in adults. Keep in mind that sound travels.
5th Intercostal space, left midclavicular line or just medial to the midclavicular line (or 4th intercostal space in a child): Location of where the mitral valve is best assessed because the flow of blood out of this valve is directed towards this area (the mitral valve is also called the bicuspid valve). This location is also considered the apex of the heart because it is where maximum impulse against the chest wall occurs as a result of systolic contraction of the left ventricle. Additionally, it is where the apical impulse and apical pulse are assessed.
Left sternal border: Location between the 2nd and 5th intercostal space close to the left sternal border.
NOTE: Certain pathophysiological processes will modify these locations. For example, an enlarged heart or congenital disorders may affect the anatomy of the heart and/or the location of the heart.
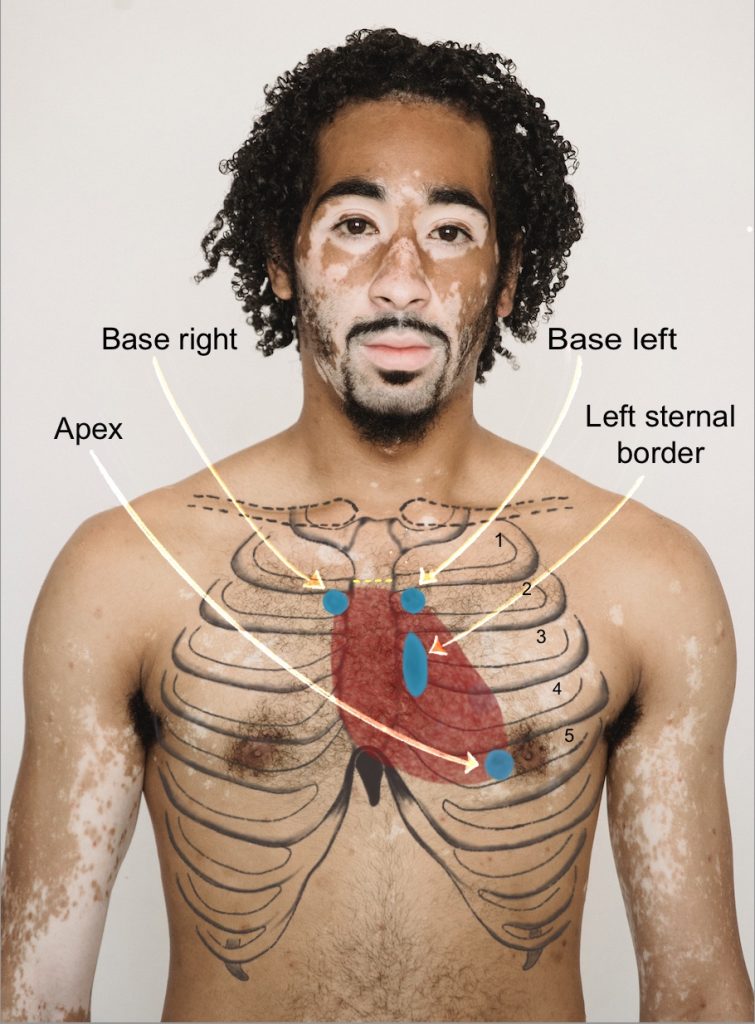
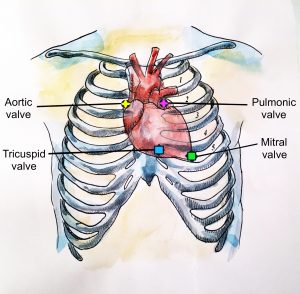
Figure 4.5: Landmarks
Image on left side: Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
Image on right side: Illustration by Hillary Tang from https://pressbooks.library.ryerson.ca/vitalsign2nd/chapter/apical-pulse/ (image was cropped and illustrated upon for the purposes of this chapter)
Techniques for landmarking on adults:
- There are approaches that you can begin with. The first approach is: Place your fingertips on the manubrium and slide your fingers down to the sternal angle. You will have reached the sternal angle when you feel a small ridge. The sternal angle is attached to the second rib. Slide your fingers over to the rib on the right sternal border and slide your fingers down into the space below the second rib – this is the 2nd intercostal space. This location is considered the base of the heart and where the aortic valve is best assessed. The alternative approach is: On the right side, place your index and middle fingers on the clavicle, slide down until you feel the first rib. Then, slide them into the 1st intercostal space and down over the second rib. Then, slide fingers down into the 2nd intercostal space at the right sternal border. This location is considered the base of the heart and where the aortic valve is best assessed.
- Follow this same space across the sternum into the 2nd intercostal space of the left sternal border. This location is considered the base of the heart and where the pulmonic valve is best heard.
- Now slide your fingers down the chest wall feeling for each rib and each intercostal space below the rib until you reach the 5th intercostal space at the left sternal border. This is the location of where the tricuspid valve is best heard. Stay close to the sternum because the ribs are easier to feel.
- Follow the 5th intercostal space out to the left midclavicular line or just slightly medial. This is the location of the apex of the heart, the location where you palpate the apical impulse, and the location where you auscultate the apical pulse and the mitral valve.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=374#oembed-3
Video 4.5: Landmarking the heart
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=374#h5p-29
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=374#h5p-3
Inspection of the Precordium
38
The precordium is the region on the chest wall that overlays the heart area. The base of the heart is located in the region of the second intercostal space and the apex is located in the region of the fifth intercostal space on the left side. As you inspect the chest wall, you will collect data that provides information about cardiac function.
Inspection of Precordium
1. Place the client in supine position with their head on a pillow.
2. Provide draping.
3. Use tangential lighting with a penlight across the heart area.
4. Inspect the base of the heart, left sternal border, and apex of heart. You may do this in sequence so that you are only exposing the area that you are assessing and then move on to the next area. See Figure 4.6 and Video 4.6.
5. Observe for the presence or absence of impulses against the chest wall and note the location.
- Pulsations: These are gentle flickers observed on the skin of the chest wall. They can be considered normal when observed on clients with thin chest walls. Otherwise, these are cues that require further assessment because they may be suggestive of increased cardiac workload associated with conditions such as an enlarged heart.
- Heaves: These are a more forceful movement (a thrust) observed on the skin over the chest wall. These cues require further assessment because they also may be suggestive of increased cardiac workload such as an enlarged heart.
6. Note the finding
- Normal findings might be documented as: “No cardiac impulses observed against chest wall.”
- Abnormal findings might be documented as (example): “Gentle pulsation observed at apex.” or “Heave observed at apex.”

Figure 4.6: Location of the base of the heart, left sternal border, and apex of heart
Photo by Armin Rimoldi from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=376#oembed-3
Video 4.6: Inspection of precordium
Impulses observed on the chest wall should always be assessed further because they are suggestive of some sort of increased workload of the heart and/or vasculature (such as the aorta). A heave can be associated with cardiac hypertrophy (enlargement of the heart muscle) or a dissecting aorta (a tear in the inner arterial wall that can lead to a rupturing of the aorta). These can be caused by many conditions such as hypertension, valvular disease, septal defects, and infarction. Your assessment can contribute to the database about whether the impulse is benign, such as may appear with a client who has a thin chest wall, or whether the impulse may have a pathophysiological cause.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=376#h5p-30
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=376#h5p-31
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=376#h5p-4
Palpation of the Precordium
39
Palpation of the precordium involves palpating the chest wall and palpating the apical impulse.
Palpation of Chest Wall for Pulsations
Palpation of the chest wall provides information about the quality of cardiac blood flow.
Palpation for pulsations involves the following steps (see Video 4.6):
1. Maintain the client in a supine position and continue to use draping as needed.
2. Palpate the base of the heart, the left sternal border, and the apex.
3. Use one of two techniques to palpate:
- Use the metacarpophalangeal surface of your fingers starting at the base of the heart. Leave them in place as long as you need to, but usually about two to three seconds and then move onto the sternal border and then the apex. (This is the most common technique).
OR
- Use the ulnar surface of your hands starting at the base of the heart. Place your ulnar surface in several locations because its surface is smaller than your metacarpophalangeal surface. Leave them in place as long as you need to, but usually about two to three seconds and then move onto the sternal border and then the apex
4. Identify presence of any pulsations that feel like a vibratory sensation.
Tip: Place your fingertips over your trachea and stick your tongue out and say “ahhh.” The vibrations that you feel on your fingertips are similar to what a thrill feels like on the chest wall.
- Healthy blood flow does not produce a vibratory sensation.
- The presence of any vibratory sensations are abnormal; turbulent blood flow can create a vibratory sensation (typically referred to as a thrill) felt on the chest wall. If you feel a thrill, you should auscultate for a murmur and expect other subjective findings associated with an incompetent valve (not opening and closing correctly). You should conduct a full cardiac and vital sign assessment and notify the physician/nurse practitioner.
5. Note the findings
- Normal findings might be documented as: “Absence of vibratory sensations.”
- Abnormal findings might be documented (example): “Thrill palpated at second intercostal space left sternal border.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=378#oembed-5
Video 4.6: Palpation of precordium
Palpation of Apical Impulse
Palpation of the apical pulse provides information about the location and the workload of the heart. You are specifically palpating for a physical pulsation over the apex of the heart. This involves the following steps (Video 4.7):
- Maintain the client in a supine position and continue to drape.
- Physically landmark the expected location of the apex. In adults, this is the fifth intercostal space at the left midclavicular line or just midline to the midclavicular line; in children, it is the fourth intercostal space at the left midclavicular line.
- Place the finger pad of your index finger at this location in the intercostal space. Use the finger pad (not the fingertip) because it is more sensitive to pulsations. Thus, you will need to keep your hand/wrist/forearm low so that your hand/wrist/forearm are parallel to the client’s chest.
- Ask the client to hold their breath after taking a large breath in and out. You should feel the pulsation quite quickly if it is palpable.
- If you do not feel a pulsation, help the client into a left lateral position. This positioning rotates the apex of the heart and accentuates the impulse against the chest wall. Usually, you can leave your finger in place when re-positioning the client.
- Note the findings
-
- Normal findings might be documented as: “Gentle tap of apical impulse, short duration, one smooth pulsation, 1–2 cm2 at apex.” Also note that it is normal not to feel an apical impulse in many clients as well. In this case, note “No apical impulse felt after re-positioning client in left lateral position.”
- Abnormal findings might be documented as: “Double systolic impulse lateral to left midclavicular line with sustained forceful thrust lasting throughout systole.” (This is just one example of an abnormal finding.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=378#oembed-6
Video 4.7: Palpation of apical impulse (NOTE: Not clearly seen in the video, ensure that you place your index finger at the left mid-clavicular line).
You might feel what is perceived as an abnormal apical impulse for many reasons. The heart might be displaced and/or have an accentuated impulse and extended duration with conditions such as left ventricular hypertrophy (enlargement of the left ventricle muscle), volume overload, and heart failure. The apical impulse can be accentuated with exercise, anxiety, fever, and other conditions when higher cardiac outputs are needed. Also, the apical impulse can shift laterally and up with pregnancy to accommodate the growing uterus.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=378#h5p-32
Auscultation of the Heart
40
Auscultation of the heart involves auscultating the apical pulse followed by auscultating the valves of the heart. You must always cleanse the stethoscope prior to auscultating. After you have cleansed it, do not set it down on the table or wrap it around your neck because this will contaminate it.
Extraneous noises can be heard when in a noisy environment or with a client who has a hairy chest. Thus, it is important to reduce environmental noise if possible and keep your stethoscope still when you press it against the chest.
Auscultation of the Apical Pulse
41
Auscultation of the apical pulse involves assessing the rate and the rhythm. This is best done at the apex, which is landmarked at the 5th intercostal space (for adults) and the 4th intercostal space (for children) at the left midclavicular line. See Figure 4.7.
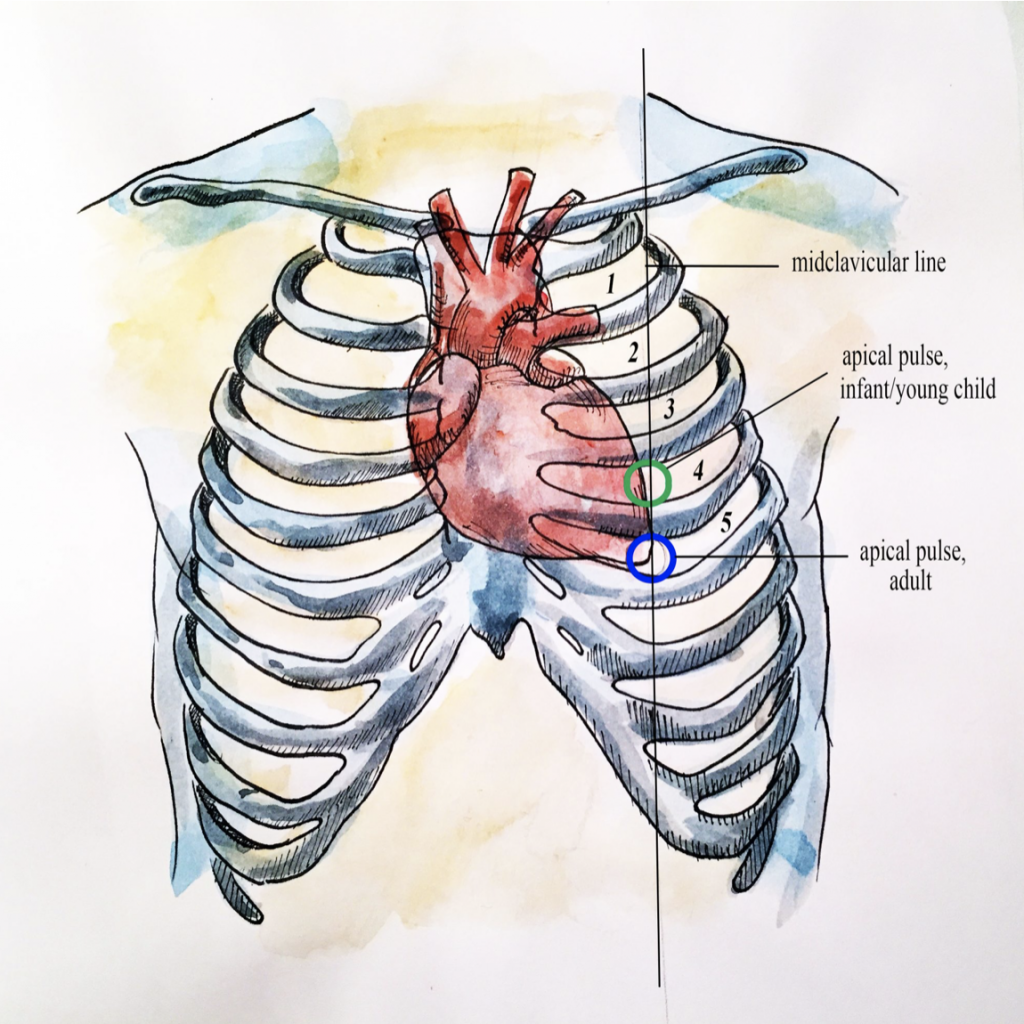
Figure 4.7: Location of apical pulse
Illustration by Hillary Tang from https://pressbooks.library.ryerson.ca/vitalsign2nd/chapter/apical-pulse/ (image was cropped and illustrated upon for the purposes of this chapter)
Auscultation of the apical pulse involves the following steps (see Video 4.8):
1. Keep the client in a supine position and continue to drape.
- This procedure can also be completed in a sitting position.
2. Cleanse the stethoscope.
3. Physically landmark the location of the apical pulse.
4. Place the diaphragm of the stethoscope at the correct location with a complete seal.
5. Count the rate for one minute and report beats per minute.
- One beat is considered one cardiac cycle (systole and diastole) and it sounds like “lub dub.” Lub correlates with the closure of the AV valves and is referred to as S1; it signals the beginning of ventricular contraction (systole). Dub correlates with the closure of the SL valves and is referred to as S2; it signals the beginning of ventricular relaxation (diastole).
- Apical pulses are typically counted for a full minute to assess for any irregularities.
6. Note the rhythm (e.g., regular or irregular rhythm).
- Normally, the rhythm is regular which means there is an even tempo with equal intervals between beats.
- If the rhythm is irregular, note whether it is a regularly irregular rhythm or an irregularly irregular rhythm.
- Regularly irregular rhythm: a regularity to the irregular rhythm, for example three regular beats and one missed beat and then this pattern is continually repeated.
OR
-
- Irregularly irregular rhythm: an irregularity to the irregular rhythm, for example there is no pattern to the irregular rhythm. For example, you might hear two beats in a row, 1 missed beat, three beats in a row, 1 missed beat, 1 beat etc… This irregular rhythm is more concerning. When it is irregularly irregular, it is an erratic rhythm in which the heart is not always fully contracting at systole and filling with blood at diastole. This type of rhythm is highly specific to atrial fibrillation, in which the atria quiver. This can result in blood clots and decreased stroke volume and cardiac output. As a result, it can also lead to the heart not optimally perfusing blood to the periphery.
- If the rhythm is irregular, check for a pulse deficit. A pulse deficit is when the radial pulse is less than the apical pulse, meaning that you will feel less palpable pulses at the radial site compared to the number of beats heard when auscultating the apical pulse. Normally there is no pulse deficit when a heart is perfusing the periphery. Experts suggest that a pulse deficit of more than 10 should be investigated further particularly when associated with other symptoms. To assess for a pulse deficit, use the following steps:
- While auscultating the apical pulse, also palpate the radial pulse. You can usually do this at the same time and note whether they are equal.
- If they are unequal, count the apical pulse for one minute, and then count the radial pulse for one minute. Next, subtract the radial pulse from the apical pulse to obtain the client’s pulse deficit. For example, if the apical pulse is 90 beats per minute and the radial pulse is 72 beats per minute, you would calculate the pulse deficit as 18 beats per minute (90 – 72 = 18), meaning that those 18 times that the heart contracts, the blood is not being perfused to the periphery.
7. Note the findings
- Normal findings might be documented as (example): “Apical pulse 82 beats per minute with a regular rhythm.”
- Abnormal findings may be documented as (example): “Apical pulse 134 beats per minute with an irregularly irregular rhythm.”
See Audio 4.1 to listen to a normal apical pulse. Listen for the “lub dub.” And then listen again, and count the pulse and report the beats per minute. (Find the answer at the bottom of this page)
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=382#h5p-67
Audio 4.1: Normal apical pulse
(Attribution statement: taken from https://wtcs.pressbooks.pub/nursingskills/chapter/9-3-cardiovascular-assessment/)
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=382#oembed-3
Video 4.8: Auscultation of apical pulse
ANSWER: The apical pulse rate in Audio 4.1 is 64 beats per minute.
Notify the physician/nurse practitioner if a client has an irregularly irregular rhythm and is showing signs of bradycardia or tachycardia. Additionally, a pulse deficit is of concern because it is suggesting that the heart is not perfusing the periphery. Thus, you should perform a full cardiac assessment. Unless the client is showing signs of clinical deterioration and requires prompt intervention, you should first complete a full cardiac assessment so that you can provide a full report of the relevant cues and share recommendations for actions.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=382#h5p-59
Auscultation of the Cardiac Valves
42
Auscultation provides information about the functioning of the cardiac valves, for example whether they are opening and closing appropriately and the quality of blood flow through the valves. Cardiac valves include the atrioventricular valves (AV) (tricuspid and mitral) and the semilunar valves (SL) (aortic and pulmonic). Remember, auscultate them at the location that corresponds with the flow of blood out of the valve, not at their anatomic location.
Biological background of heart sounds
You need to know what you are listening for when auscultating the valves. First, you are listening for heart sounds (“lub dub”). As described above, these sounds are related to the closing of the heart valves and referred to as S1 (lub) and S2 (dub). In a healthy heart with no valvular pathology, the opening of these valves is silent.
- S1 is the closing of the AV valves including the tricuspid valve and the mitral valve. Although the mitral valve closure occurs immediately prior to the tricuspid valve closure because of the route of electrical charges in the heart (i.e., myocardial depolarization), the closing of these valves are generally heard at the same time in the healthy heart – lub.
- S2 is the closing of the SL valves including the aortic valve and pulmonic valve. Although the aortic valve closure occurs immediately prior to the pulmonic valve closure because of the route of electrical charges in the heart, the closing of these valves are generally heard at the same time in the healthy heart – dub.
Recall what you learned in biology:
- S1 involves the closing of the AV valves, so it is considered the beginning of systole (contraction of the ventricles ejecting blood into the pulmonary artery and the aorta).
- When the AV valves close, all four cardiac valves remain closed momentarily (it’s called isovolumetric contraction) and then the semilunar valves (aortic and pulmonic) open while the ventricles contract.
- Then, the semilunar valves close (S2); this is considered the end of systole and the beginning of diastole (relaxation of the ventricles filling with blood)
- When the semilunar valves close, all four cardiac valves are closed momentarily (this is called isovolumetric relaxation) and then the AV valves open and the ventricles fill with blood (i.e., diastole).
Auscultating cardiac valves
The steps involved in auscultation of the cardiac valves are (see Video 4.9):
1. Keep the client in a supine position and use draping.
- You can do this assessment with the client in a sitting position, but it is generally easier to do in a supine position because you can drape the client without struggling to hold the drape in place. Also, you might have to ask a client who is sitting to reposition their breasts to auscultate the valves; this is easier in a supine position as larger breasts will typically shift laterally in a supine position.
- NOTE: if you have specific cardiac concerns, you should also listen for murmurs in the left lateral position and in the sitting position with the client leaning forward slightly. This positioning can help you hear any murmurs that might be present.
2. Cleanse the stethoscope.
3. Follow the pattern in Figure 4.8 to auscultate the cardiac valves.
- Particularly when you have concerns, some practitioners will move their stethoscope around several locations at each site.
- Remember, it is important to physically landmark the location of the valves immediately before you auscultate them.
-
- Landmarking for these valves is important. For a reminder about landmarking, go back to The Heart page to watch the video.
4. Auscultate all four valves with the bell, and then begin again and auscultate all four valves with the diaphragm.
- Heart sounds are typically classified as low-pitched, but you should use both the bell and diaphragm to distinguish sounds because some may be better heard with the diaphragm versus the bell. For example, S1 is lower in pitch than S2 and some abnormal heart sounds are higher in pitch.
- At each location, listen as long as you need to complete the assessment, but for at least two to three full cardiac cycles (including systole and diastole). You may need to listen longer if you hear abnormal sounds.
- S1 and S2 – (lub dub) Are they clear and distinct sounds? Or do you hear split sounds associated with S1 and S2? This can occur when the tricuspid and mitral valve do not close at the same time or the aortic and pulmonic do not close at the same time.
- Murmurs are a whooshing sound associated with turbulent blood flow that can occur when a valve is not opening and closing appropriately. See Audio 4.2 to hear what a murmur sounds like. When a valve is not working properly, this can lead to regurgitation of blood. Sometimes a murmur is caused by heightened blood flow such as during pregnancy or exercise. Assess whether murmurs are present or absent; if you hear a murmur, the main characteristics to be evaluated are:
- Timing with the cardiac phase. Is it associated with S1 or S2?
- Grading of the loudness of the sound (see Table 4.2). Murmurs that are grade 4 and above are associated with a palpable thrill.
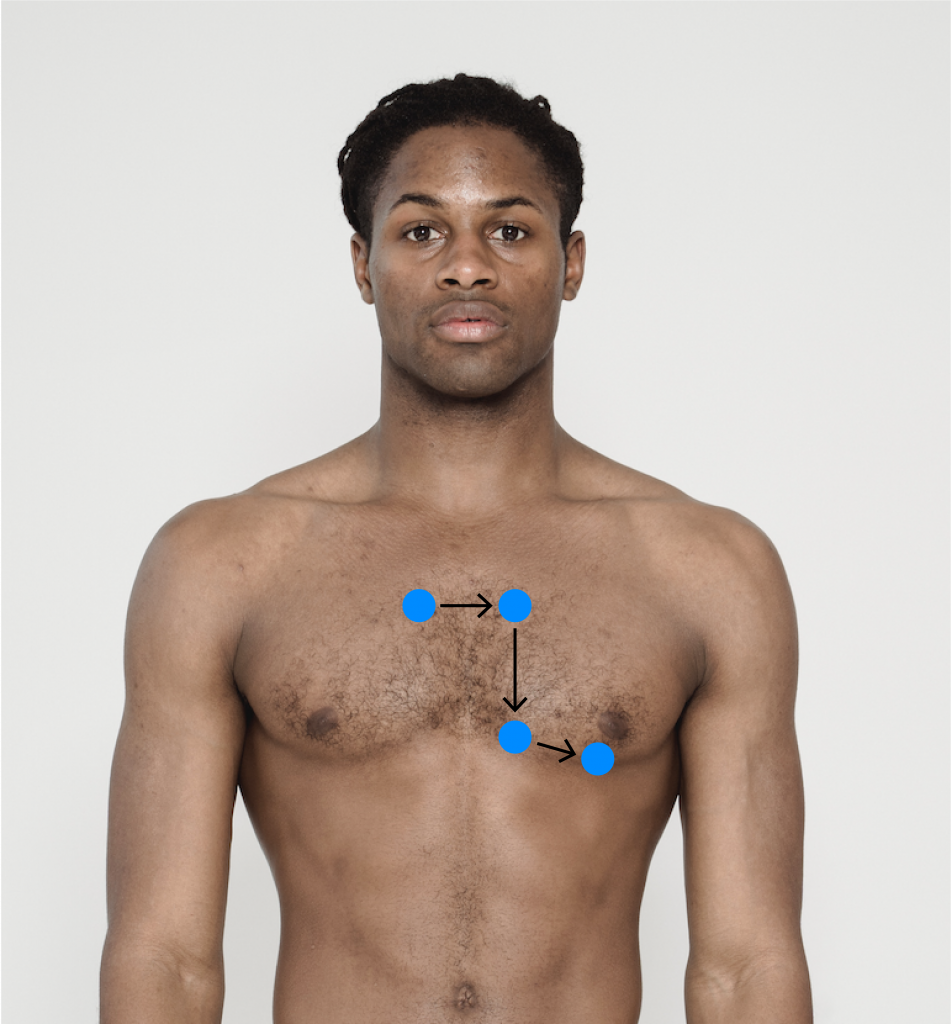
Figure 4.8: Pattern for auscultation of cardiac valves
Photo by Mike Jones from Pexels (image was cropped and illustrated upon for the purposes of this chapter)
5. Note the findings
- Normal findings might be documented as: “Clear S1 and S2, no split sounds, no murmurs.”
- Abnormal findings might be documented as: “Clear S2, no split sounds, grade II murmur heard best on S1, at the apex.” (This is just one example of an abnormal finding that could be associated with mitral regurgitation.)
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#h5p-67
Audio 4.2: Normal S1/S2 sounds
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#h5p-68
Audio 4.3: Murmur
(Attribution statement: taken from https://wtcs.pressbooks.pub/nursingskills/chapter/9-3-cardiovascular-assessment/)
Table 4.2: Levine’s murmur scaled (adapted from Silverman & Wooley, 2008).
| Grade 1 |
Faint/difficult to hear (not heard right away) |
| Grade 2 |
A faint murmur heard immediately |
| Grade 3 |
Moderately loud murmur |
| Grade 4 |
Loud murmur |
| Grade 5 |
Very loud murmur. Can be heard if only the edge of the stethoscope is in contact with the skin. |
| Grade 6 |
Loudest possible murmur. The murmur can be heard with the stethoscope just removed from the chest and not touching the skin. |
See Video 4.10 for an in-depth understanding of heart sounds: the main point is that heart sounds can change based on cardiac pathologies. Heart Sounds | Complete Cardiac Sounds with Audio | Heart Sounds Made Easy.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#oembed-5
Video 4.9: Auscultation of cardiac valves
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#oembed-6
Video 4.10: Heart sounds
The cardiac valves may be associated with many issues, most commonly regurgitation/prolapse and stenosis. Regurgitation is leaking or backflow of blood through the valve; this is sometimes caused by prolapse in which the valve does not close completely. Stenosis involves narrowing of the valve, which limits/restricts blood flow through the valve.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#h5p-35
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=384#h5p-36
Reference
Silverman, M., & Wooley, C. (2008). Samuel A. Levine and the history of grading systolic murmurs. The American Journal of Cardiology, 102(8), 1107-1110. https://doi.org/10.1016/j.amjcard.2008.06.027
Health Promotion and Disease Prevention: Considerations and Interventions
43
Health promotion and disease prevention are important components of a healthy cardiovascular system. To determine appropriate interventions, you must carefully consider all available subjective and objective data. Part of your subjective data collection will include inquiring about risk factors, social determinants, and other considerations.
The inquiry part is integrated throughout the assessment. Many of the probing questions may be asked when doing the subjective assessment. However, some of the questions will be formulated based on your critical reflection of data collected during the subjective and objective assessment. It is this data that will inform your clinical judgment and the health promotion needed for a specific patient.
Smoking
First-hand, second-hand, and third-hand smoke are major risk factors that negatively affect the cardiovascular system. The chemicals in smoke cause inflammation of the blood vessels and contribute to plaque buildup and narrowing of the blood vessels.
Probing questions related to smoking include:
- Do you smoke cigarettes or any tobacco-related products? If the client’s answer is affirmative, ask probing questions: How much do you smoke? How many packages of cigarettes do you smoke a day? How many years have you smoked? Can you tell me about the reasons that you started smoking?
- If you do not currently smoke, have you ever smoked? If the client’s answer is affirmative, ask similar probing questions as above, including the reason that they quit.
- Have you ever tried quitting? If the client’s answer is affirmative, ask probing questions: Tell me about what made you want to quit? How long did you quit? Did you use any strategies to help you quit?
- Have you ever thought of quitting? If the client’s answer is negative, make a non-judgemental comment like: “If you ever want to discuss quitting, let me know, there are many resources to help you.”
The effectiveness of health promotion is influenced by client interest and collaborative intervention because these factors are important in producing a successful outcome in smoking cessation. Each intervention must be tailored to the client, and could include counselling, cognitive-behavioural therapy, pharmacology treatments (e.g., nicotine replacement therapy), smart-phone applications, and short text message services. Sometimes a brief discussion about risks and a recommendation to quit smoking is sufficient. You might also choose to be involved in developing public health educational campaigns and resources about how smoking affects health as a population-based prevention strategy.
Contextualizing health promotion related to smoking from a sociocultural perspective will help you understand who might be more vulnerable or at risk. For example, the prevalence of smoking is higher among individuals with lower socio-economic status and lower education attainment, and those experiencing racial and ethnic discrimination (Wang & Wu, 2020). These populations are less likely to have access to resources pertaining to smoking cessation, so it is important to consider interventions as they relate to the social determinants of health, rather than using a one-size-fits all approach (Brady, 2020).
Contextualizing Inclusivity – Tobacco
Tobacco plays an important part in traditional and spiritual practices in many Indigenous communities (CAN-ADAPTT, 2010). Many, but not all, Indigenous peoples use it for ceremonial and medicinal purposes (CAN-ADAPTT, 2010). Nurses should recognize and distinguish between tobacco use for traditional purposes and misuse, and questions to the client should be culturally sensitive and respectful of these differences (CAN-ADAPTT, 2010).
Diet
An unhealthy diet is a risk factor that contributes to cardiovascular disease, such as a diet high in saturated and trans fats, cholesterol, sodium, and alcohol. It is best for clients to choose water and reduce caffeine and alcohol intake. Clients with heart failure are sometimes recommended to limit all types of fluids.
Probing questions related to diet include:
- Tell me about your usual diet?
- What have you eaten in the last 24 hours? Is that your usual diet?
- Have you had any recent changes in your life that have affected your diet?
- Do you add sugar and salt to your food?
- How much fluid do you typically drink in a day? What fluids (e.g., water, caffeinated beverages, alcohol)?
You may want to assess a client’s familiarity with Health Canada’s (2019) Food Guide and discuss with them how to use it: https://food-guide.canada.ca/en/. This new food guide still has a Eurocentric bias, so you should collaborate with the client about its relevance in the context of their cultural food practices. It is now offered in dozens of languages that you can refer clients to: https://www.canada.ca/en/health-canada/services/canada-food-guide/resources/snapshot/languages.html and many resources are available about food safety for Indigenous People: https://www.sac-isc.gc.ca/eng/1581522106156/1581522147811
Some key elements of Canada’s Food Guide are:
- Be mindful of eating patterns.
- Choose water as the drink of choice.
- A dinner plate should be one-half vegetables/fruit, one-quarter protein, and one-quarter whole grains.
- Make time to enjoy eating meals with others.
- Cook when possible, as opposed to eating processed meals and purchasing fast foods.
- Reduce sodium, saturated and trans fats, and sugar, and monitor portion sizes.
Canada’s guidelines now suggest that there are health risks associated with any level of alcohol consumption, although negligible with two drinks or less weekly (Paradis et al., 2022). Although some previous research had suggested some positive benefits to alcohol, this is now being disputed indicating that drinking alcohol of any kind does not decrease risks of heart disease, and high levels of consumption increase risk for coronary artery disease, myocardial infarction, heart failure, hypertension, and stroke (Paradis et al., 2022).
Many types of diets can be heart healthy, but some research points especially to the benefits of the Mediterranean diet and DASH diet. The American Heart Association (2020) recommends the Mediterranean diet as heart healthy: it includes plenty of fruits and vegetables, grains, potatoes, legumes, nuts, and seeds, olive oil, along with small amounts of dairy, eggs, fish, and poultry. The Heart and Stroke Foundation of Canada (n.d.) recommends the DASH (Dietary Approaches to Stopping Hypertension) diet as heart healthy and helpful to lower blood pressure: it is rich in vegetables, fruit and low-fat dairy foods and lower in saturated fat, total fat and cholesterol. The two diets are very similar and may be used in combination; the Mediterranean diet typically emphasizes more fish and less dairy products than the DASH diet.
Healthy eating involves behavioural actions but also relational and structural actions. First, an individual needs access to healthy food and the financial capacity to purchase it; this is referred to as food security. The rising cost of food globally has made this a challenge, and in many remote regions of Canada’s North, access to nutritious food is limited in terms of availability; even when available, the costs are excessive.
Socioeconomic status is known to affect food purchasing: individuals from socioeconomically disadvantaged communities – those with lower household income and lower levels of education – purchase fewer healthy foods like fruits and vegetables (Turrell et al., 2002). Therefore, health promotion efforts should focus on narrowing socioeconomic differences in food purchasing. Nurses can work in partnership with disadvantaged individuals and tailor a health promotion approach to their particular needs and attend to structural and economic barriers (Turrell et al., 2002). For example, you could direct clients to organizations that partner with vulnerable communities to support access to healthy foods, skill development, and capacity-building in terms of community-led initiatives (Turrell et al., 2002). You could also advocate on behalf of these communities for more effective social policy to address food insecurity (Turrell et al., 2002).
Activity
A sedentary lifestyle with limited activity/exercise is another risk factor that contributes to cardiovascular disease.
Probing questions related to activity are:
- Do you have any concerns about your level of activity or exercise?
- Tell me about your daily pattern of activity? What activity are you involved in?
- What exercise do you engage in? How long do you do this type of exercise? How many days a week do you exercise? If a client plays sports, ask about their use of protective equipment.
You can collaborate with clients to create an activity/exercise care plan that is specific to their needs and goals. Start at a realistic and attainable level, depending on physical capability and energy level, then slowly increase the timing and level of activity. Many interventions are also available to support clients to achieve their activity goals: community walking groups, fitness apps, local gyms, and group activities. The participACTION website is a helpful resource for activity guidelines: https://www.participaction.com/en-ca
Nurses should use a relational health promotion approach when addressing activity. A community of support can promote activity, so you should assess the client’s access to support (e.g., friends, family, acquaintances) who may have similar activity interests or goals. A structural approach to health promotion can also help address and eliminate inequities. For example, some clients may not be able to afford gym memberships or sports registration fees. Additionally, those in urban areas may have more access to specific activities or rehabilitation programs than those living in rural or remote regions, including in the North. You will need to consider these factors and tailor activity programming to each client. You could also advocate for policies to address these inequities.
Sleep
Adequate sleep is important for restoration of the body and mind: 6–8 hours is usually considered adequate sleep. Pulse and blood pressure lower during deep sleep, known as non-rapid eye movement, which is important for cardiovascular health. Lack of sleep quality and quantity has been linked to cardiovascular-related illnesses such as hypertension, obesity, myocardial infarction, and stroke.
Probing questions related to sleep include:
- How much sleep do you get each day/night? How many hours? Do you rest during the day?
- Do you have any concerns about your sleep?
- Tell me about your sleep routine? What do you do before you go to bed? Do you take any medications to help you sleep?
- Do you wake up during the night? If so, why? Are you able to fall back to sleep?
- Do you feel rested when you wake up?
One behavioural intervention is a sleep journal. Ask the client to record how much sleep they get. If less than recommended, address potential triggers that may be disrupting the client’s sleep, such as stress or pain. Limiting screen time two hours prior to bedtime can also be helpful. Additionally, you may want to discuss with the client the potential for naps.
The physical and social environment affects sleep. Siengsukon (2020) describes that sleep may be affected by the following:
- Living in an unsafe or noisy neighbourhood.
- Not having access to private transportation and needing to get up early to commute via public transportation.
- Living in congregate or multigenerational housing might mean that clients share bedrooms or beds.
- Being a caregiver for a spouse or parent can also interfere with sleep, as does living with someone who works long hours or shift work.
It is important to note that many of these physical and social factors influencing sleep are associated with race, ethnicity, and socioeconomic status (Siengsukon, 2020).
Stress
Stress is subjective and can have emotional, physical, mental, social, and financial effects; it is a risk factor for cardiovascular-related illnesses. Stress is usually caused by a combination of multiple stressors. How a person may talk about themselves, their life and their situation can indicate potential concerns and areas that need further assessment.
Probing questions related to stress could include:
- Tell me about the stress in your life?
- Have you experienced stress recently? Physically? Emotionally?
- Have you had any recent changes in your life? (tell me more).
- How does stress affect you?
- How do you handle this stress?
- Tell me about the coping strategies you use?
Stress management and coping strategies may include:
- Regular physical activity.
- Getting adequate sleep.
- Spending time with family and friends.
- Taking time for personal interests and hobbies.
- Practicing relaxation techniques such as meditation, deep breathing exercises, and tai chi.
From a relational and structural health promotion perspective, it is important to be aware that stress does not exist in a vacuum: how it is experienced, perceived, and managed is affected by relationships with others. All clients experience stress sometimes, but structural factors influence whether a client is more at risk for stress or able to manage stress. For example, racism is a major determinant that can lead to highly stressful experiences. You can use an anti-racist approach to stress and stress management to understand how the client is being influenced by racism and how best to support them. Socioeconomic status can also influence a person’s access to resources to cope with stress. When collaborating with clients to develop stress management techniques, you must be aware of these larger structural influences.
Weight and blood pressure
Obesity and high blood pressure are linked to cardiovascular-related illnesses, so clients should monitor their weight and blood pressure.
Probing questions may include:
- Are there any recent changes in your life that may have affected your weight or blood pressure?
- Have you had any recent changes in your weight?
- Do you have any concerns about your weight?
- When was the last time you had your blood pressure taken?
- Do you know what your blood pressure normally is?
In collaboration with the client, discuss any disruptions in daily patterns and explore possible ways to address these – and facilitate weight loss and lowering of blood pressure if relevant. Many interventions related to diet, activity/exercise, and stress will help with weight and blood pressure. Nurses can also advocate on behalf of clients and take actions to develop and advance equitable healthy public policies.
References
American Heart Association (2020). What is the Mediterranean diet? https://www.heart.org/en/healthy-living/healthy-eating/eat-smart/nutrition-basics/mediterranean-diet
Brady, K. T. (2020). Social determinants of health and smoking cessation: A challenge. The American Journal of Psychiatry, 177(11), 1029-1030. https://doi.org/10.1176/appi.ajp.2020.20091374
CAN-ADAPTT. (2011). Canadian Smoking Cessation Clinical Practice Guideline. Canadian Action Network for the Advancement, Dissemination and Adoption of Practice-informed Tobacco Treatment, Centre for Addiction and Mental Health. https://www.nicotinedependenceclinic.com/en/canadaptt/PublishingImages/Pages/CAN-ADAPTT-Guidelines/CAN-ADAPTT%20Canadian%20Smoking%20Cessation%20Guideline_website.pdf
Health Canada (2109). Canada’s Dietary Guidelines for health professionals and policymakers. https://food-guide.canada.ca/en/guidelines/
Heart & Stroke Foundation of Canada (n.d.). The DASH diet to lower high blood pressure. https://www.heartandstroke.ca/healthy-living/healthy-eating/dash-diet
Paradis, C., Butt, P., Shield, K., Poole, N., Wells, S., Naimi, T., Sherk, A., & the Low-Risk Alcohol Drinking Guidelines Scientific Expert Panels. (2022). Update of Canada’s Low-Risk Alcohol Drinking Guidelines: Final Report for Public Consultation. Ottawa, Ont.: Canadian Centre on Substance Use and Addiction.
Siengsukon, C. F. (2020). The link between social determinants of health, sleep, and cardiovascular disease. Cardiopulmonary Physical Therapy Journal, 31(1), 5-10. https://doi.org/10.1097/CPT.0000000000000130
Turrell, G., Hewitt, B., Patterson, C., Oldenburg, B., & Gould, T. (2002). Socioeconomic differences in food purchasing behaviour and suggested implications for diet-related health promotion. Journal of Human Nutrition and Dietetics, 15(5), 355-364. https://doi.org/10.1046/j.1365-277X.2002.00384.x
Wang, G., & Wu, L. (2020). Healthy people 2020: Social determinants of cigarette smoking and electronic cigarette smoking among youth in the United States 2010-2018. International Journal of Environmental Research and Public Health, 17(20), 7503. https://doi.org/10.3390/ijerph17207503
Clinical Judgment – Case Study
44
A 34-year-old male client arrives in the emergency department with his partner. The partner is crying, stating the client tried to stand after dinner, and then fell to the floor holding his chest. Upon assessment, the client was experiencing shortness of breath, had a racing heartbeat, voiced slight chest discomfort and said he felt a fluttering sensation in his chest. He also said he has lower back pain. RR: 28 bpm, HR: regular irregular rhythm 146 bpm, BP: 132/86 mmHg, O2: 97%. The client is diaphoretic and states he feels lightheaded, dizzy, and is afraid he’s going to faint.
After reading the following scenario, perform a primary survey of the client. Remember your ABCDEs! The goal is to determine whether urgent interventions are needed and act on signs of clinical deterioration.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=388#h5p-37
- Common symptoms to assess related to the cardiovascular system include chest pain, dyspnea, arrhythmias, coughing/wheezing, and edema.
- The objective assessment of the cardiovascular system is always performed on bare skin and involves a combination of positions including sitting upright, head of bed at 45 degrees, and supine.
- A trauma-informed approach to the objective assessment is necessary considering that areas of the chest are being exposed.
- The objective assessment includes auscultation and palpation of the carotid arteries, inspection of the jugular pulsation, and inspection, palpation, and auscultation of the heart.
- Health promotion interventions should be developed in collaboration with the client to address what is important to them.
Chapter 5 - Gastrointestinal System
V
By Dr. Jennifer Lapum, Michelle Hughes, Dr. Erin Ziegler, Evan Accettola, Alexis Andrew, and Sita Mistry
- Apply subjective assessment skills.
- Apply objective assessment skills.
- Use clinical judgment.
- Integrate health promotion interventions into actions.
Introduction to Gastrointestinal System
The gastrointestinal system (also called the GI system) is important to assess because it is responsible for nutrition, digestion, absorption, hydration, and defecation. You may also have heard it referred to as the digestive system. As a nurse, your assessment of the GI system provides information about how the system is functioning and potential cues that require action.
GI System Components
As per Figure 5.1, the main components of the GI system include:
- The upper GI tract (oral cavity, esophagus, stomach, and the first part of the small intestine [i.e., the duodenum]).
- The lower GI tract (small and large intestine, rectum, anus).
- The accessory glands and organs (salivary glands, liver, pancreas, gallbladder) and lymphatic organs and tissue (tonsils, spleen, appendix).
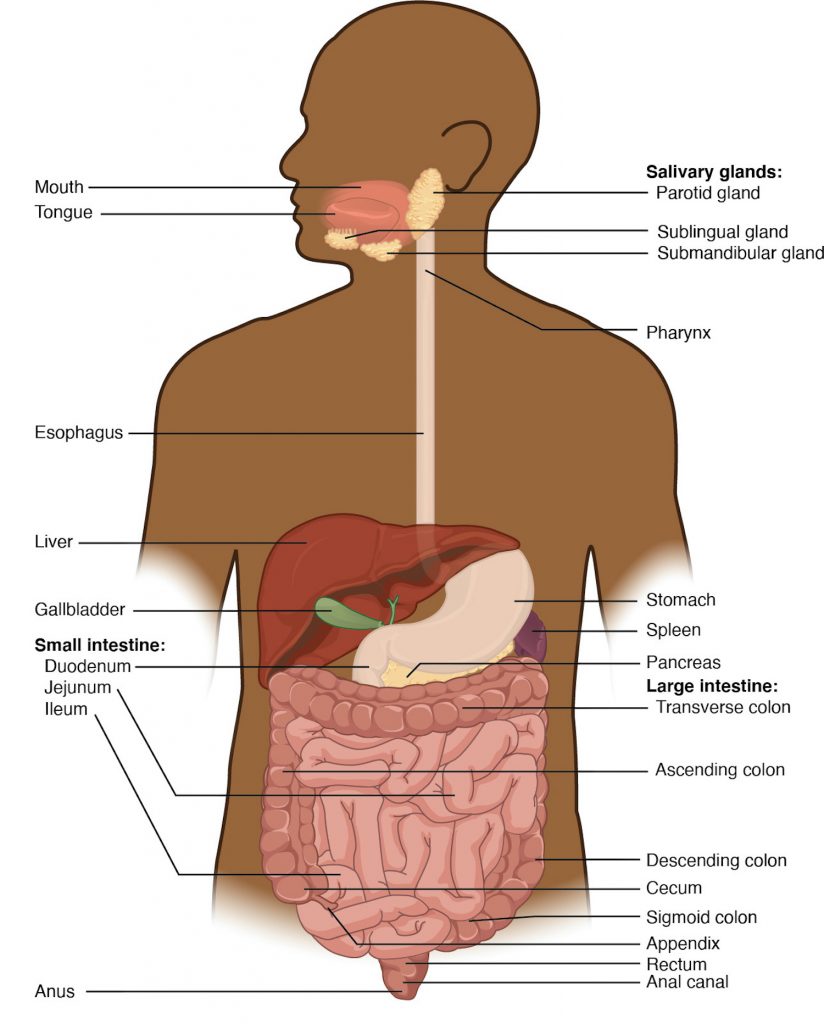
Figure 5.1: GI tract
(Attribution statement for image at bottom of page)
You have already learned about the anatomy and physiology of the GI system; See Video 5.1 for a quick overview:
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=658#oembed-3
Video 5.1: Overview of the GI system. (Attribution taken from: https://www.khanacademy.org/science/high-school-biology/hs-human-body-systems/hs-the-digestive-and-excretory-systems/v/meet-the-gastrointestinal-tract)
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=658#h5p-58
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=658#h5p-56
Attribution statement for Figure 5.1 – Image from: J. Gordon Betts, Kelly A. Young, James A. Wise, Eddie Johnson, Brandon Poe, Dean H. Kruse, Oksana Korol, Jody E. Johnson, Mark Womble, Peter DeSaix, Anatomy and Physiology, OpenStax, Apr 25, 2013, Houston, Texas. Section URL: https://openstax.org/books/anatomy-and-physiology/pages/23-1-overview-of-the-digestive-system. Licenced under Creative Commons CC BY 4.0.
Subjective assessment of the GI system involves asking questions about the health of the client and symptoms related to pathologies of the associated organs and glands. Although a full understanding of these pathologies is beyond the focus of this chapter, common issues associated with the GI system include dental cavities, gastroesophageal reflux disease (GERD), cancer, ulcers, hepatitis, ascites, ileus, irritable bowel syndrome, constipation, hernias, and hemorrhoids.
Ulcers have emerged over the last century as a common condition. For decades, researchers believed the cause was related to increased acid production, foods, and stress. In the early part of this century, researchers found that Helicobacter pylori (H. pylori) bacteria are a common cause of gastric and duodenal ulcers (Ahmed, 2005; Kusters et al., 2006). Since then, there has been a major shift in both diagnostics and treatment, including testing for H. pylori and use of medications including antibiotics and proton pump inhibitors. Correct treatment is important considering that untreated ulcers can lead to perforation of the gastric or intestinal wall (depending on location) followed by peritonitis and possible hemorrhage.
Common symptoms that can be related to the GI system include pain, nausea and vomiting, appetite changes, bowel patterns changes including diarrhea and constipation, bloating, and flatulence. See Table 5.1 for guidance on a subjective health assessment related to common symptoms, questions, and clinical tips. Many of the questions in this table align with the PQRSTU mnemonic. You should consider asking questions in order of importance, thus you do not follow the sequential order of PQRSTU.
You should also ask about any medications (prescribed, over the counter, or illicit) the client is taking, including the name, dose, frequency, reason for taking, and how long they have been taking it. Many types of medications can cause GI upset (nausea, vomiting, constipation, diarrhea).
Always use questions focusing on health promotion during an assessment. Depending on the context, you might ask these during the subjective assessment or after an objective assessment. A “Health Promotion Considerations and Interventions” section is provided later in this chapter after the discussion of an objective assessment.
Table 5.1: Common symptoms, questions, and clinical tips
|
Symptoms
|
Questions
|
Clinical tips
|
|
Dysphagia is difficulty related to swallowing and can involve difficulty related to swallowing saliva, food, and/or fluids. It can be caused by a variety of conditions that can be associated with structural issues (inflammation) or neural issues (stroke).
|
Do you have any current or recent difficulty swallowing?
If the client’s response is affirmative, additional probes may include:
Quality/quantity: Tell me about the difficulty. What does if feel like? How bad is it?
Region: Where do you feel it (e.g., in the throat area or lower in the upper esophageal area)?
Understanding: Do you know what is causing it? Do you have any related symptoms (e.g., pain, swollen glands, excessive saliva, drooling)?
Timing: When did it begin? What were you doing when it began? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is it aggravated or associated with eating or drinking? Is there anything that makes it better (e.g., position)?
Treatment: Have you treated it with anything? Do you take any medications for it?
|
New onset of dysphagia requires immediate action because it can lead to clinical deterioration and complications such as choking or aspiration pneumonia. If a client is experiencing new onset dysphagia, it is important to restrict food or fluids until it has been fully assessed. If possible, have the client sit upright (e.g., high fowler position) or raise the head of the bed.
|
|
Oral lesions, discolourations, and bleeding gums.
|
Do you currently have or have you had any chronic issues with sores/ulcers in your mouth, discolouration of your mouth, or bleeding gums?
If the client response is affirmative, additional probes may include:
Region: Where is it located?
Quality/quantity: Tell me about it. How bad is it?
Timing: When did it begin? What were you doing when it began? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Treatment: Have you treated it with anything? Do you take any medications for it?
Understand: Do you know what is causing it or what it is related to?
|
The first action is to inspect the mouth so that you can provide an objective assessment.
Interventions will depend on the cause. For example, bleeding gums may be caused by brushing too hard or increased vascularity associated with pregnancy; they can also be caused by gum disease, so you may need to refer the client to a dentist.
|
|
Xerostomia is dry mouth; it can be mild and easily treated or severe and affecting a client’s quality of life, health, and overall wellbeing. It can be associated with dehydration, certain medications, cancer treatments such as radiation therapy, and alcohol and drug use.
|
Do you currently have a dry mouth or have you had any chronic issues with dryness in the mouth?
If the client’s response is affirmative, additional probes may include:
Quality/quantity: Tell me about your dry mouth. What does it feel like? How bad is it?
Timing: When did it begin? Is it constant or intermittent?
Understanding: Do you know what is causing it or what it is related to?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Other questions may include: How much fluids do you drink per day? Are you taking any medications or radiation therapy? How much alcohol do you drink per day? Do you take any drugs? Do you smoke?
Treatment: Have you treated it with anything? Do you take any medications for it? Tell me about how much fluids you drink per day
|
Interventions will depend on the cause.
Older adults are at risk for xerostomia due to decreased intake of fluids as well as increased usage of medications and certain medical conditions that affect the functioning of the salivary glands.
It may be as simple as encouraging the client to drink more water, limit sodium, limit alcohol and drug use, and use sugar-free gum or lozenges.
You should also ask about smoking, which can further aggravate symptoms related to dry mouth.
If a client has chronic dry mouth, inspect their mouth for associated symptoms such as cracked lips, gum disease, tooth decay, and oral lesions. You should also assess whether it is affecting the client’s nutrition or other elements of daily life such as wearing dentures, especially when the client is an older adult.
|
|
Mouth pain or sensitivities can involve a sore throat, tooth pain or sensitivities, and jaw pain.
|
Do you currently have or have you had any issues with mouth pain or sensitivities such as a sore throat, tooth pain or sensitivities, or jaw pain?
If the client response is affirmative, additional probes may include:
Region: Where is it located?
Quality/quantity: Tell me about it. How bad is it?
Timing: When did it begin? What were you doing when it began? Is it constant or intermittent?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Treatment: Have you treated it with anything? Do you take any medications for it?
Understand: Do you know what is causing it or what it is related to?
|
These symptoms require an objective assessment to assess further GI signs, or signs related to other systems.
First, assess whether the jaw pain might be cardiac-related. Angina is a critical finding that requires immediate intervention and can radiate to the jaw area. In order to determine this, you should assess what brought the pain on. For example, was there a physical injury? If not, are there other related factors and symptoms.
Another common cause of jaw pain is bruxism, which can be caused by stress. These types of symptoms and tooth pain and sensitivities usually require referral to a dentist.
|
|
Upper and lower GI pain can be associated with many conditions. This is an unpleasant sensation that is described subjectively in a ways such as tenderness, achy, discomfort, burning, or sharp pain.
|
Do you have any current or recent pain in the esophageal or abdominal region (or unpleasant sensations such as tenderness)?
If the client’s response is affirmative, additional probes may include:
Region: Where do you feel the pain/sensation? Does it radiate anywhere?
Quality/quantity: Tell me about it. What does it feel like? How bad is it?
Timing: When did it begin? What were you doing when it began? Is it constant or intermittent?
Severity: Can you rate it on a scale of 0 to 10 with 0 being no pain and 10 being the worst pain you have had?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Treatment: Have you treated it with anything? Do you take any medications for it?
Understand: Do you know what is causing it or what it is related to?
|
With children, always tailor questions to their developmental stage. With infants and pre-verbal or non-verbal children, you may need to focus on objective assessment such as behavioural and physiological signs of pain.
Remember that GI pain is sometimes cardiac-related (angina). You must rule out this possibility because it can be a critical finding that requires urgent intervention.
|
|
Nausea and vomiting (emesis) are common symptoms associated with many conditions. Nausea is an uneasiness/queasy feeling in the stomach associated with the urge to vomit. Vomiting (emesis) is the emptying of the GI tract (usually the contents of the stomach/esophagus) through the mouth. When associated with pregnancy, this is called hyperemesis gravidarum (morning sickness).
|
Do you have any current or recent nausea and vomiting?
If the client’s response is affirmative, additional probes may include:
Timing: When did it begin? When was the last time? What were you doing when it began? Is it constant or intermittent? Is it associated with eating?
Quality/quantity: Tell me about it. What does the nausea feel like? How bad is it?
If the client indicates vomiting, ask: How much do you vomit? Is it undigested food? What colour is it? Is there blood in it?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Treatment: Have you treated it with anything? Do you take any medications for it? (If so, do they help?)
Understand: Do you know what is causing it or what it is related to? Do you have any other related symptoms (e.g., stomach pain, fever)?
|
Nausea and vomiting are usually not serious, and are often associated with a bacterial or viral infection. However, they may be associated with a more serious condition such as appendicitis, a concussion, or an intestinal blockage.
Hematemesis is a serious concern that suggests GI bleeding. It is important to assess the colour, as this can help determine where the bleeding is coming from and whether it is active bleeding or old, dried blood. For example, bright red suggests active bleeding from the upper GI system. You might also visualize vomit that has dark brown or black specks in it resembling coffee grounds, which is suggestive of bleeding.
It is important to determine the cause and severity of the nausea and vomiting. Antiemetics are a class of drugs used to prevent and treat nausea and vomiting. Many types are available, including dimenhydrinate (Gravol).
Assess the client for risk of dehydration, particularly among children or older adults or when vomiting is frequent with large quantities. Common signs of dehydration include dry mouth, cracked lips, decreased skin turgor, tachycardia, increased thirst, decreased urine output, delirium, and in infants, sunken fontanelles.
|
|
Changes in bowel patterns can include constipation or diarrhea. These changes can be short-term or chronic and can be associated with many health conditions and other factors such as diet.
Constipation refers to decreased frequency in bowel movements (BMs) (less than three per week) and difficulty having a BM (having to strain to push stool out, hard stool). Diarrhea refers to soft, loose, watery stools that are not formed and are frequent (three or more a day).
|
Tell me about your normal bowel patterns?
Probing questions may include: How often do you have a bowel movement? What is the consistency (soft or hard)? What colour is it? Have you ever noticed mucus or blood in it? Do you have any concerns about your bowel patterns? Do you take any medications to help you have a bowel movement (such as a stool softener or laxative)? Have you had any recent or frequent diarrhea or constipation?
If the client has concerns about their bowel patterns or has reported a problem such as diarrhea or constipation, probe further with questions such as:
Timing: When did it begin? When was the last time? Is it constant or intermittent? Is it associated with eating?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Treatment: Have you treated it with anything? Do you take any medications for it (if so, do they help)?
Understand: Do you know what is causing it or what it is related to? Do you have any other related symptoms (e.g., stomach pain)?
|
Remember that normal bowel patterns vary from client to client.
Some people, particularly older children/adolescents and young adults, may feel embarrassed to talk about bowel patterns. Try to normalize the discussion using statements like “I like to speak with all clients about their bowel patterns because it can provide information about your health.”
An inclusive approach to assessment involves age- and culturally-appropriate terms. For example, not everyone will know what a BM is, so you may need to use words like “poop” or “number two.”
Blood in the stool can appear as bright red or black/dark brown. Assessing the colour helps determine the cause, which can be something mild to something as severe as colorectal cancer. A focused assessment is important.
If a client has constipation or diarrhea, choose an appropriate action based on the severity. Dietary changes and hydration are often helpful, but in some cases, severe constipation could be related to a bowel obstruction and requires urgent intervention. This may be associated with other symptoms such as abdominal pain and a distended abdomen.
Severe diarrhea can lead to dehydration, which is a serious issue and needs to be treated with rehydration with fluids and electrolytes. Chronic and severe diarrhea could be related to digestive disorders (e.g., lactose intolerance, Crohn’s disease, ulcerative colitis, celiac) or viral (e.g., norovirus), bacterial (e.g., clostridium difficile [C. diff.]), or parasites (e.g., giardia) Contact isolation is required when a client has or is suspected to have infectious diarrhea.
|
|
Appetite changes are common symptoms associated with the GI system.
These changes can involve a decrease or increase in appetite (for foods or fluids), and can be physiologically or psychologically related.
|
Have you had any recent appetite changes (such as decreased or increased appetite)?
If the client’s response is affirmative, additional probes may include:
Quality/quantity: Tell me about the changes? How bad have the changes been?
Timing: When did these changes begin? Are the changes in appetite constant or intermittent? What was going on in your life when these changes began?
Provocative/palliative: Is there anything that makes the appetite changes worse? Is there anything that makes the appetite changes better?
Treatment: Have you treated the appetite changes with anything? Do you take any medications for it?
Understand: Do you know what is causing the appetite changes or what they are related to?
|
Changes in appetite can be a sensitive issue for some clients. Use a non-judgmental approach when asking questions, and use words that the client uses when asking additional probes (e.g., when did you begin feeling like not eating?).
Prompt intervention is needed if a newborn is not eating, as adequate nutrition is important to growth and development, and they can also dehydrate easily.
|
|
Other GI-related symptoms can include fatigue, unintended weight loss, fever, rectal pain/bleeding/pruritus, and lymph node swelling.
|
Only ask one question at a time. For example: Have you experienced fatigue (appetite changes, unintended weight loss, fever, rectal pain/bleeding, lymph node swelling)?
If the client’s response is affirmative, use variations of the PQRSTU mnemonic to assess the symptoms further.
|
Keep in mind that many of these GI-related symptoms can be related to other body systems. Thus, these symptoms require further investigation to determine whether they are related to the GI system. You should assess the severity of rectal bleeding to determine whether prompt intervention is required.
|
|
Personal and family history of GI conditions and diseases.
As noted earlier, common issues associated with the GI system include dental cavities, acid reflux, ulcers, cancers, hepatitis, ascites, constipation, and hernias.
|
Do you have any chronic conditions or diseases associated with your GI system? Do you have a familial history of conditions or diseases related to the GI system?
If the client’s response is affirmative, begin with an open-ended probe: Tell me about the condition/disease?
If the client has a personal history, additional probing questions might include:
Timing: When did it occur? When were you diagnosed?
Quality/quantity: How does it affect you? What symptoms do you have?
Treatment: How is it treated? Do you take medication?
Provocative/palliative: Is there anything that makes it worse? Is there anything that makes it better?
Understanding: Do you have any concerns about how the condition or disease is affecting you?
|
Some clients may not be familiar with the word gastrointestinal (GI). If so, use words such as the mouth, esophagus, stomach, liver, bowels/intestines.
Some GI-associated diseases have a genetic component, but environmental and cultural factors (family traditions and personal practices) are more likely for many symptoms (e.g., diarrhea, constipation, hepatitis).
|
Blood can appear in the stool for various reasons; this requires a focused and prompt assessment so that you can attempt determine the cause. Start by asking when it began and what the client has noticed (e.g., colour, amount, associated symptoms).
- If the colour is bright red, this suggests active bleeding and is usually associated with the lower GI system, possibly related to the rectal area or the lower/distal portion of the colon. The objective assessment should begin by inspecting the perianal region to check for any bleeding around the anus, possibly caused by hemorrhoids.
- Sometimes the bleeding is difficult to notice because it is darker in colour. Melena is black sticky stool (often referred to as tar-like) and can be caused from bleeding higher in the GI tract. You might visualize dark brown or black specks in stool resembling coffee grounds.
- If the stool is red and resembles a jelly-like substance, this could indicate intussusception. It is a serious GI condition in which a part of the intestine folds into itself, causing obstruction of the bowel and constriction of blood supply. It is rare in adults, but a common cause of intestinal obstruction in infants and toddlers. It is often associated with severe abdominal pain, lethargy, nausea, and vomiting.
Sometimes what looks like blood in the stool is not actually blood. Diet (e.g., beets, black licorice) and certain medications (e.g., iron medications) can change the colour of stool.
Some blood is not visible to the naked eye. This is called “occult blood” and can only be determined by testing a stool sample for blood. In Ontario, a fecal immunochemical test (FIT) is routinely recommended when someone is at “average risk” (over age 50 and no first-degree relative diagnosed with colorectal cancer) or at “increased risk” (family history of colorectal cancer) (Cancer Care Ontario, n.d.).
If you identify blood in the stool, your action should be based on its severity and associated symptoms. Act promptly if the amount of blood is concerning or if the client shows signs of clinical deterioration. It’s always best to do a primary survey to determine the potential of deterioration.
Certain symptoms associated with the GI system are cues that require action. Urgent intervention is required when the cues suggest clinical deterioration or the potential for clinical deterioration. For example, urgent intervention is required with:
- New onset dysphagia (can be associated with stroke and/or can lead to complications).
- Severe diarrhea and/or vomiting (particularly with signs of dehydration or when vomiting indicates hematemesis).
- GI pain (may suggest angina) or right lower quadrant pain (may suggest appendicitis).
- GI pain in infants (may suggest intussusception).
If you encounter a cue that suggests clinical deterioration, ask a colleague to call the physician/nurse practitioner while you perform a primary survey and a focused objective assessment. For example, assess the client’s respiration rate, work of breathing, oxygen saturation, and then pulse, blood pressure, and temperature, followed by auscultation of lungs.
Any evidence of bleeding requires intervention. However, the severity (e.g., the amount and whether it is active bleeding) will determine how prompt the intervention needs to be. Additionally, when a care partner or parent indicates that an newborn/infant has had a decreased number of wet diapers, you should conduct further assessment as this could be a sign of dehydration.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=664#h5p-57
References
Ahmed, N. (2005). 23 years of the discovery of Helicobacter pylori: Is the debate over? Annals of clinical Microbiology and Antimicrobials, 4(1). https://doi.org/10.1186/1476-0711-4-17
Cancer Care Ontario (n.d.). Guidelines & advice: Colorectal cancer screening recommendations summary. https://www.cancercareontario.ca/en/guidelines-advice/cancer-continuum/screening/resources-healthcare-providers/colorectal-cancer-screening-summary
Kusters, J., van Vliet, A., & Kuipers, E. (2006). Pathogenesis of Helicobacter pylori infection. Clinical Microbiology Reviews, 19(3), 449-490. https://doi.org/10.1128/CMR.00054-05
Objective assessment of the GI system includes:
- Inspection and palpation related to the oral cavity.
- Inspection, auscultation, palpation, and percussion of the abdomen.
- Inspection and palpation of the perianal region.
Be aware of the environmental temperature in the room and the temperature of your hands. Room temperatures are not easily modified, so try to limit exposing the client and keep them covered. Draping is particularly important when assessing the abdomen and perianal region. Before touching the client, warm your hands by rubbing them together and warm the stethoscope before placing it on the client’s body.
Oral Cavity - Inspection and Palpation
Usually the client is positioned sitting upright; newborns or young children can be held by their parent/caregiver. Wear gloves because this assessment involves contact with body fluids from the mucus membranes. You will also need a tongue depressor and a penlight.
Inspection of Lips
Inspect the lips for swelling, colour, lesions, or malformations. Also inspect the lips for moisture and texture, which are interrelated.
The steps for this are as follows:
1. Identify any presence and location of swelling and redness.
- These two findings are often associated. You must respond immediately if you suspect the swelling is associated with anaphylaxis. For example, do they have allergies, such as food or bees, or have they recently had a vaccine? Do they have other signs of anaphylaxis (e.g., hives, pruritus, dyspnea, dysphagia, tachycardia, hypotension)?
2. Note the colour.
- Lip colour varies based on the client’s skin colour. It can range from pink to brown tones. Note any lip discolouration (e.g., redness, cyanosis, pallor). Cyanosis can appear as a grey/white shade in people with darker skin (Lewis, 2020; Sommers, 2011) or as a dusky bluish/purple shade in people with lighter skin (Lewis, 2020). Pallor can appear as a grey shade in people with darker skin (Lewis, 2020) or as a generalized pale discolouration in people with lighter skin.
3. Identify the presence, location, size, and description of any lesions and malformations, including the colour and presence of any discharge.
- If you identify a lesion, ask the client whether they have noticed it, how long they have had it, whether they know the cause, and if they have treated it with anything.
- A common lesion on the lips is herpes simplex virus (cold sore) which appear as small, fluid-filled blisters, see Figure 5.2. Another common malformation of the lip is a cleft lip (which is sometimes associated with a cleft palate). These are important to assess and act upon because they can affect a client’s breathing, speaking, and sucking and swallowing associated with eating. They are often surgically repaired at a young age. Further information and images for cleft lip and palate can be found at: https://www.cdc.gov/ncbddd/birthdefects/cleftlip.html
4. Note the moisture and texture.
- Are the lips moist or dry? Moist lips are smooth with no cracking. Dry lips are chapped and/or may have fissures. Chapped lips are flaky and sometimes red, with “flakes” or “scales” of skin peeling away from the lips. Fissures are usually called “cracked lips.”
5. Note the findings.
- Normal findings: “Lips are moist with no cracking, lesions, or swelling, pink in colour with generalized brown tones, no discolouration.”
- Abnormal findings: “Lips are dry with cracking, a red lesion on upper lip left of midline 3mm x 3 mm with a slight serous discharge.”
Figure 5.2: Herpes simplex virus (cold sore) on the lower lip.
(Attribution: Photo Public Domain, https://commons.wikimedia.org/w/index.php?curid=8011415)
Inspection of Oral Mucosa
Systematically inspect all parts of the mucosa. Shine a penlight in the mouth to illuminate the area. You can ask the client to pull their top lip up and then their bottom lip down, or use a gloved hand or tongue depressor to perform this action so you can inspect the mucosa on the inside of the lips.
Most clients can open their mouth wide and tip their head back so that you can observe the palate and also put the tip of their tongue behind their front teeth so that you can observe the floor of the mouth and under the tongue. You can use a tongue depressor to expose the buccal mucosa. To expose the pharynx, ask the client to stick their tongue out and say “ahhh” or pretend to yawn. You may need to use the tongue depressor to press the tongue down. If so, avoid using it in the middle of the tongue as this may elicit a gag reflex.
Inspection of the mucosa of the oral cavity includes observing the insides of the lips and the buccal mucosa (inside of checks), the tongue, the floor of mouth (under the tongue) and the hard and soft palate, the pharynx, and salivary glands. See Figure 5.3 for anatomical locations of the oral cavity.
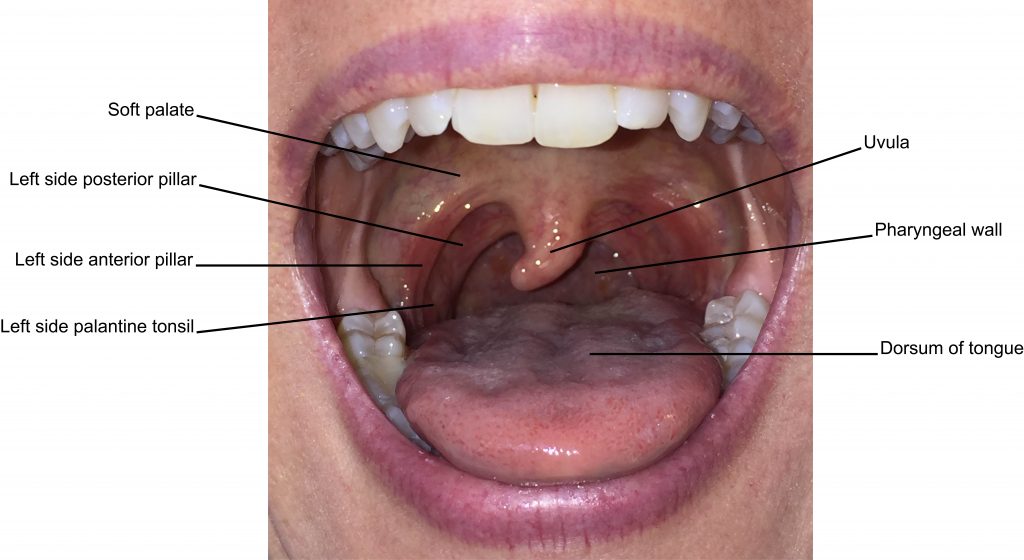
Figure 5.3: Anatomical locations of oral cavity
Use the following steps:
1. Note moisture or dryness.
- The whole oral cavity should be moist. Dry mucous membranes are often a sign of dehydration. However, you should also assess if the client may be a person who breathes through their mouth and not their nose. You will notice tiny ductal openings (about 1 mm in size) of the salivary glands. These glands produce saliva for the mouth and include the parotid (ductal opening on the buccal mucosa near the upper second molar), the submandibular (ductal opening at the base of the ventral surface of the tongue on both sides of the frenulum), and the sublingual (several ductal openings on both side of the floor of the mouth).
2. Inspect the mucosa of the lips and buccal mucosa for colour, lesions, swelling, and nodules.
- The mucous membranes, including the mucosa of the lips and buccal mucosa, are pink in colour. Any discolourations (e.g., cyanosis or pallor) should be described and the location noted. Cyanosis can appear as a grey/white shade in people with darker skin (Lewis, 2020; Sommers, 2011) or as a dusky bluish/purple shade in people with lighter skin (Lewis, 2020). Pallor appears as a grey shade in people with darker skin or as a generalized pale discolouration in people with lighter skin.
- The mucosa of the lips and buccal mucosa are intact with a smooth surface. Note the description and location of any lesions, swelling, or nodules. Palpate any lesions, swelling, or nodules and identify the consistency (e.g., soft or hard).
3. Inspect the tongue, floor of the mouth, and hard and soft palate for colour, lesions, swelling, nodules, and malformations.
- Note the colour and any discolourations along with the location. The tongue is normally pink with a dotted surface that is most readily seen on the dorsal and posterior side. The small and hard palate are a lighter pink in which the hard palate (directly behind the upper front teeth) has a slight white shading. The ventral surface of the tongue is highly vascular, and you will observe veins under the tongue.
- The mucosa is normally intact with a smooth texture except the hard palate, which has a ridged surface. Note the description and location of any lesions, swelling, nodules, or malformations. Palpate any lesions, swelling, or nodules and identify the consistency (e.g., soft or hard). One of the most common malformations at birth is a cleft palate.
- While doing so, observe for halitosis, which refers to a bad odour. It is important to recognize that “stale” smelling breath is not necessarily a concern and also to understand that this can be embarrassing for clients. Therefore, it is important to approach the situation in a sensitive manner. There are many causes of halitosis that should be assessed. For example, common causes are dehydration, bacteria associated with poor oral care, diabetes, tobacco, and recent ingestion of foods such as garlic, onion and coffee.
4. Inspect the pharynx for colour, swelling, lesions, and nodules, and describe the tonsils.
- Note the colour and any discolourations (such as redness or white patches) along with the location.
- Identify the presence, location, and description of any swelling, lesions, or nodules.
- Note the size of both the left and the right tonsil. Sometimes tonsils have been surgically removed so they may not be present. But, usually tonsils are just visible to view. Many “scales” are used to grade tonsil size, but there is no one standardized scale. Therefore, it is better to describe the size such as:
- Tonsils are not present.
- Tonsil(s) is visible between the anterior and posterior pillar, but not enlarged.
- Tonsil(s) is enlarged at halfway between the anterior pillar and the uvula.
- Tonsil(s) is enlarged and touching the midline of the mouth or the uvula. (If both tonsils are enlarged, you may describe them as touching each other).
5. Note the findings.
- Normal findings might be documented as: “Moist oral cavity. Pink mucosa with no discolouration, lesions, nodules, or swelling. Tonsils are visible but not enlarged.”
- Abnormal findings might be documented as: “Dry mucous membranes of oral cavity. White, raised patches on the tongue, buccal mucosa, soft palate, and pharynx.”
Teeth and Gums
Assessment of the teeth and gums includes inspection and palpation. Use a penlight to illuminate the back of the mouth. Begin by asking the client to smile to expose the teeth, and use a tongue depressor or your gloved finger to expose the gums and the back teeth. Remember: your assessment of the teeth and gums does not replace a routine dental assessment.
Assessment of the teeth and gums involves the following steps:
1. Inspect the colour of the teeth.
- Tooth enamel is white, so you should note any discoloration. When enamel begins to erode, teeth may have a yellowish colour, which reflects the underlying layer, and even a brown colour. Enamel erosion and tooth discolouration can be caused by many things including smoking, diet (e.g., red wine, coffee/tea), bruxism, decay, and acids introduced into the mouth as a result of bulimia. Some mild erosion is associated with aging due to exposure to cultural factors such as diet.
2. Inspect for missing, chipped, or broken teeth.
- Note the presence and location.
3. Inspect for missing or loose fillings.
- Note the presence and location.
4. Inspect the gums for colour, swelling, and bleeding.
- Identify the presence and location of any discolouration such as redness, swelling, or bleeding. Healthy gums have a pink colour similar to the buccal mucosa, with no swelling or bleeding.
5. Palpate for loose teeth and palpate the gums for pain.
- Use your gloved finger to palpate for the presence of any loose teeth, and note the location.
- Next, use your gloved finger to palpate the gums for pain while using the tongue depressor to pull the buccal mucosa out. Ask the client if they feel any pain or tenderness and note the location.
6. Note the findings.
-
Normal findings might be documented as: “White teeth with no loose, missing, chipped or broken teeth. Gums are pink in colour with no swelling, bleeding, or pain.”
- Abnormal findings might be documented as: “Slight yellow discolouration of the teeth. Second molar on upper right side loose with swelling of the gum and mild bleeding.”
Respond immediately if a client has swollen lips consistent with other signs of anaphylaxis (e.g., hives, pruritus, dyspnea, dysphagia, tachycardia, hypotension). If so, did they just receive a vaccine or were they exposed to an allergen (e.g., a food or bee sting) that they are allergic to? If so, call for help and notify the physician/nurse practitioner immediately. If you are permitted to do so, administer epinephrine. Continue to monitor the client because anaphylaxis is life-threatening.
If the client shows signs of cyanosis or pallor, perform a primary survey to assess for clinical deterioration. Usually a client with discolourations in lips or mucous membranes will have other respiratory- or cardiovascular-related cues such as dyspnea, low oxygen saturation, tachypnea, and/or angina.
If the client has dry and cracked lips and dry mucous membranes with no other signs of dehydration, increasing fluid intake will usually resolve the issue. This could involve administering a rehydration solution that contains electrolytes; other forms of fluid intake can include ice chips (or popsicles for children), especially if the client is nauseated.
Further assessment and intervention may be needed if signs of more advanced dehydration are observed: poor skin turgor, oliguria, dark urine, altered level of consciousness, tachycardia, and hypotension. With newborns and infants, you should assess for sunken fontanelles, decreased wet diapers, and drowsiness. An infant may also show reduced or absent tears when crying. For a hospitalized client with signs of advanced dehydration, perform a primary survey to assess for signs of clinical deterioration, increase intravenous fluids to rehydrate, and treat any other related symptoms such as diarrhea, vomiting, and fever. Report any cues that suggest clinical deterioration to the physician/nurse practitioner.
Lesions, nodules, discolourations, and enlarged tonsils are not usually urgent priorities for treatment, but you should complete a focused assessment (subjective and objective) to document them and report your findings to the physician/nurse practitioner. If tonsils are enlarged, you should assess the colour and the presence of exudate. If tonsils are touching the uvula or each other, you should assess for any breathing or swallowing issues. These associated symptoms require prompt intervention. Any issues associated with teeth (particularly loose, broken, or chipped teeth or missing or loose fillings) and gums usually require referral to a dentist. You should be concerned when the client indicates they have a lesion in their mouth that will not heal or a lump. These can sometimes be associated with oral cancers, which are commonly found on the floor of the mouth, inferior side of tongue, the buccal mucosa or the soft palate. A common cause of oral cancers is tobacco use.
This image shows a throat infection called tonsillitis. Evidence of the infection is shown through swelling, redness and white patches (pus) on the tonsils. This pus consists of dead bacteria, white blood cells, and cellular debris
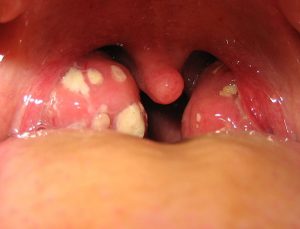
Image from: This work has been released into the public domain by its author, Michaelbladon at English Wikipedia. This applies worldwide. Michaelbladon grants anyone the right to use this work for any purpose, without any conditions, unless such conditions are required by law.
Activity: Check Your Understanding
Abdominal assessment involves inspection, auscultation, palpation, and percussion. This order of physical assessment is important to preserve normal bowel sounds when auscultating. For example, pressing on the abdomen can modify bowel sounds by increasing peristalsis (wave-like contractions of the intestines).
Before beginning, ask the client to empty their bladder and bowel so that fullness will not influence the findings.
This assessment is best accomplished in the supine position because this allows any air in the abdominal region to rise to the surface area. The client should lie flat with their head on a pillow. Some clients may find it difficult to lie completely flat; if so, you can slightly elevate the head of the bed (about 10 degrees). To ensure the abdominal musculature is relaxed, ask the client to have their arms resting beside their body and their knees bent with either their feet placed flat on the bed or a pillow placed under their knees. For a newborn or young child, you can ask someone (care partner, parent, healthcare provider) to hold them on their lap.
Always do the assessment on bare skin.
Contextualizing Inclusivity – Discomfort in Exposing Abdomen
Some clients are uncomfortable exposing their abdomen. For example, they may feel uncomfortable because of body image issues associated with weight, modesty related to cultural or religious beliefs, or a new ostomy such as a colostomy or an ileostomy. Ostomies are surgically created openings onto the abdomen that allow stool to bypass a damaged/diseased part of the intestine and leave the body.
It is important that you create an inclusive environment that is judgment free and recognizes the client’s potential discomfort. For example, you may begin the assessment with the following: “I need to assess your abdomen on the bare skin. Is that okay?” (wait for the client to give consent).
Inspection of the abdomen provides information about the client’s GI system, particularly the intestines, as well as the liver and the abdominal cavity overall. Refer to Figure 5.4 for the quadrants and regions: a horizontal and a vertical imaginary line bisects the umbilicus to help you visualize the four quadrants. Note any abnormalities of the abdomen using these quadrants and regions.
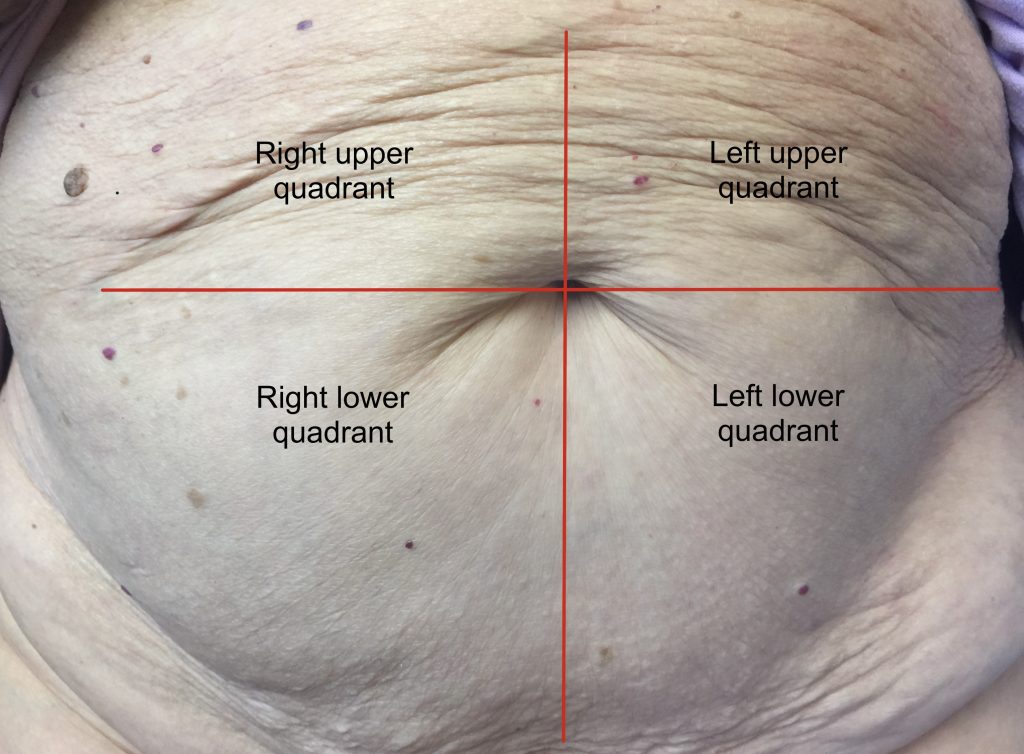
Figure 5.4: Abdominal quadrants
Inspecting the abdomen involves the following steps:
1. Before inspecting the abdomen, note the client’s level of consciousness, facial expression, and assess for the presence of jaundice.
- Clients are usually alert with a relaxed expression, although some may be nervous/anxious. Be attentive to any non-verbal signs of pain such as grimacing or guarding, and continue to observe the client’s expression throughout the assessment. In addition to providing information about non-verbal signs of pain, this can also sometimes help you assess whether further support or guidance is needed.
- Jaundice is associated with high levels of bilirubin in the blood. It is included in the abdominal assessment because it can be associated with diseases of the liver, pancreas, gallbladder, and bile duct. Clients with jaundice have a yellowish discolouration of the sclera and sometimes the skin. An inclusive approach to evaluating jaundice is to inspect the sclera of the eyes, because the melanin in skin influences how jaundice appears. Clients with lighter skin may have yellow discolouration of the skin beginning in the face and transmitting to the rest of the body, but relying on assessment of the skin alone is an example of how health assessment practices can be non-inclusive or racist.
2. Ask the client to expose their abdomen so you can observe from the epigastric (inferior to xiphoid process) down to the hypogastric region (superior to the pubic bone).
3. Note any stoma bags, tubes, drains, incisions, scarring, dressings, or medical equipment (e.g., monitors). NOTE: If you observe discharge/bleeding on a dressing, outline it with a marker/pen and observe whether it increases in size. However, if it is significant quantity, you should investigate the cause and perform a primary survey.
4. Use tangential lighting and observe all four quadrants.
- Observe the profile view (side view) while standing on the client’s right side. Standing on this side will help you visualize any peristaltic movement, which will move away from you. These movements are the waves caused by the gastrointestinal tract (e.g., large intestine contractions). Peristalsis movement is usually not observable on the abdomen. You may see it in a client who is thin; otherwise, visible peristalsis is a cue that should act as a concern and can suggest an intestinal blockage. In a newborn, observable peristalsis may be associated with pyloric stenosis (narrowing of the opening between the stomach and the intestines), but this condition is associated with other symptoms such as projectile vomiting.
- Next, position yourself so that your eyes are at about the level of the abdomen at the side, and also view the abdomen from the end of the bed. This will allow a full view of the abdomen so you can compare the left and right sides of the full abdomen (including the umbilicus) and assess symmetry.
5. Note any potential signs of observable pain. (Remember: if you suspect pain, always ask the client.)
- Observe for signs of pain may include facial expressions, behavioural changes (e.g., complete stillness or restlessness or guarding) or physiological changes (e.g., holding their breath, shallow breathing).
- In pre-verbal children (or other non-verbal clients), signs of pain may include groaning, grimacing, shallow breathing, irregular rhythm of breathing, and tachypnea. Newborns and infants may flex their hips and knees, moving their legs up to their chest.
- Note that a client may be experiencing pain even if you do not observe signs of it. Clients with chronic pain often do not exhibit behavioural signs of pain.
6. Note the abdominal shape.
- Identify the presence of symmetry or asymmetry and any bulging.
- The abdomen should be symmetrical and the umbilicus should be midline. Note the location of any asymmetry. If you suspect asymmetry, you can ask the client to take a deep breath in and out; this can accentuate any asymmetry or potential bulges. If the client is able to, you can also ask them to hold their head and upper shoulder area off the bed (like a little sit-up) or onto their elbows as this maneuver can accentuate any asymmetry or bulges. You could also ask them to cough; this can increase the intra-abdominal pressure and accentuate a hernia if present.
- If you observe any bulging, further assess the area and note the location. Inspect the umbilicus for bulging, which can sometimes appear as an everted umbilicus. Normally, an umbilicus is inverted. Although an everted umbilicus can be normal, so always inquire if it is new. If you observe bulging, ask the client if they have noticed it, when it began, whether they know what it is, and ask about any associated pain. At the end of the overall inspection, you can gently palpate it to assess its consistency (soft or hard) and the presence of pain.
- Identify the contour (i.e., the abdominal curve).
- The normal contour of the abdomen is typically flat or rounded.
- A concave contour (inward curve of the abdomen that looks sunken in) is concerning because it can be associated with dehydration and malnutrition, and sometimes with anorexia nervosa and cancer. In newborns, it can also suggest a congenital anomaly in which the abdominal contents have shifted elsewhere, such as up into the thorax.
- A distended abdomen is an enhanced outward contour, which can have many causes.
- The outward contour of the abdomen is typically enhanced when a client has increased air, fluid, and/or content inside the intestines, or outside the intestines within the peritoneal cavity. Distension may be associated with constipation, bowel obstruction, or irritable bowel syndrome. Severe malnutrition associated with protein deficiency and water retention can also distend the abdomen so it looks bloated. Another cause is ascites, which is the accumulation of fluid in the peritoneal cavity. Ascites has many causes, but most commonly liver cirrhosis associated with hepatitis or chronic alcohol use. In rare cases, a tumor might cause distension. Keep in mind that an infant normally has a protuberant abdomen that sticks out because of muscles that are not developed – don’t confuse this with distension. A distended abdomen is firm to touch.
7. Note skin colour, discolouration, integrity, and swelling.
- Skin colour varies based on a client’s racial background and should be consistent across the abdomen and the umbilicus. If you observe a discolouration (e.g., redness), describe it and the location. No swelling should be present and the skin should be intact; describe and note the location of any swelling or damaged skin (e.g., an open ulcer). Examine the umbilicus, which may become infected from a piercing. Note any scars, which may indicate past surgeries.
8. Note the presence of peristaltic movement.
9. Note the findings.
- Normal findings might be documented as: “Abdomen flat, symmetrical with no bulging, swelling, discolouration. Skin intact.”
- Abnormal findings might be documented as: “Client grimacing with shallow irregular breathing. Abdomen distended.”
Signs associated with an intestinal blockage is a priority of care because it may indicate the need for surgical intervention. Pain, constipation, vomiting, and abdominal distention are possible signs of a blockage. If any are present, notify the physician/nurse practitioner after performing a primary survey with a complete set of vital signs and a full abdominal assessment. It is especially important to auscultate and palpate the abdomen, because absent bowel sounds or a distended/firm and painful abdomen are associated with blockages.
All abnormal signs observed upon inspection require a full abdominal assessment. If you observe signs of pain, begin with a subjective assessment. Any asymmetry, bulging, abnormal contour, swelling, and lesions should be reported to the physician/nurse practitioner.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=672#h5p-43
Auscultation of the abdomen as it relates to the GI system is performed to assess for intestinal function, specifically bowel sounds. Bowel sounds are produced by the movement of fluid, gas, and contents through the intestines.
As a nurse, auscultating for bowel sounds with the stethoscope’s diaphragm is a common part of health assessment. The diaphragm is best for detecting high-pitched sounds such as bowel sounds. Bowel sounds are sometimes loud enough to hear without a stethoscope.
Auscultation of the abdomen follows inspection, so the abdomen is already exposed. When conducting auscultation, begin in the right lower quadrant and progress clockwise to the right upper quadrant, left upper quadrant, and the left lower quadrant. Figure 5.5 presents the pattern of auscultation. Always begin in the right lower quadrant because this is the location of the ileocecal valve, which is a muscular sphincter that allows contents to move from the ileum of the small intestine to the cecum of the large intestine.
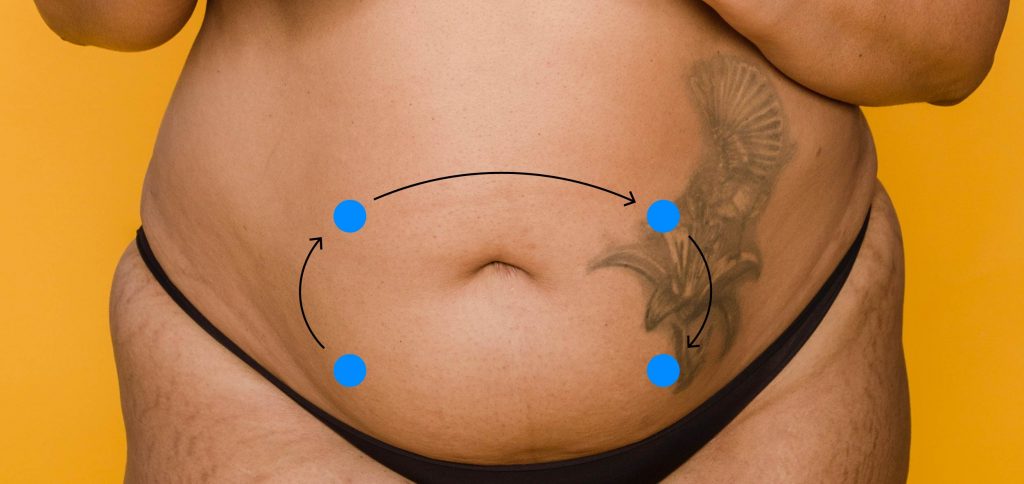
Figure 5.5: Pattern of auscultation.
Photo by Laura Tancredi from Pexels (image was cropped and illustrated upon for the purposes of this chapter) Assess the presence, frequency, and quality of bowel sounds.
- Presence. Normally, bowel sounds are present in all four quadrants. This means that peristalsis is occurring and contents are moving through the intestines. Only document the absence of bowel sounds after listening in each quadrant for five minutes. Absent bowel sounds are a cue that suggest there may be a problem with the movement of contents through the intestines: common causes include peritonitis, a complete bowel obstruction, or perforation of the small or large intestine. However, keep in mind that movements of contents and contraction of the intestines do not always create sound.
- Frequency. If you hear bowel sounds, describe the frequency (i.e., the rate of occurrence, how often do you hear them). You do not need to count the number of bowel sounds; instead, estimate whether they are considered normoactive, hypoactive, or hyperactive.
- Normoactive: 5–30 bowel sounds per minute (about 2 sounds every 5 seconds). Generally, you will only need to listen for a few seconds to estimate this frequency.
- Hypoactive: less than 5 bowel sounds per minute. Because the frequency of hypoactive sounds is less frequent, you will need to listen a bit longer in order to assess them. These sounds indicate that intestinal activity has slowed, which is normal when a person is sleeping. Hypoactive bowel sounds should act as a cue in other situations, which should always be assessed further. For example, bowel sounds may become hypoactive post-surgery due to anesthetic use and with certain medications (e.g., narcotics). Constipation is also a common cause of hypoactive bowel sounds.
- Hyperactive: more than 30 bowel sounds per minute. Again, you will only need to listen for a couple seconds in order to estimate this frequency. These sounds indicate that intestinal activity is quicker than normal. You will often hear hyperactive bowel sounds after a client has just eaten; these sounds may also be associated with diarrhea and early/partial intestinal obstruction.
- Quality. Describe the quality of the bowel sounds (e.g., the description, how they sound). You might describe the quality as high-pitched with a series or mixture of sounds (e.g., gurgling, rumbling, bubbling, and even clicking). You might describe the quality of sounds as irregular (i.e., no specific/constant rhythm). The quality of bowel sounds is typically less important than the presence and frequency, but an extremely high-pitched bowel sound can be a cue suggestive of an early bowel obstruction.
Auscultating the abdomen for bowel sounds involves the following steps (see Video 5.2):
1. Cleanse the stethoscope.
2. With a complete seal and light touch, place the diaphragm of the stethoscope on the abdomen in the right lower quadrant and listen. Next, lift the diaphragm and place it in the next quadrant.
3. Identify the presence and location of bowel sounds.
- Normally, bowel sounds should be present and heard in all four quadrants.
4. Identify the approximate frequency of bowel sounds. You do not need to count them.
5. Identify the quality of bowel sounds.
6. Note the findings.
- Normal findings might be documented as: “Normoactive bowel sounds heard in all four quadrants. High-pitched, gurgling sounds.”
- Abnormal findings might be documented as: “Hypoactive bowels sounds in all four quadrants.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=674#oembed-3
Video 5.2: Auscultating the abdomen
Any abnormal bowel sounds should be investigated. They should not be evaluated in isolation: an abnormal sound should always be considered in the context of other symptoms such as abdominal distention, flatus, pain, nausea, vomiting, diarrhea, and constipation. If a client has absent bowel sounds, consider whether this could be associated with peritonitis, a complete bowel obstruction, or a perforation of the small or large intestine. All of these issues require urgent intervention and are often associated with pain, abdominal distention, nausea, and vomiting. If you suspect one of these conditions, monitor the client closely while conducting a primary survey and complete set of vital signs. Ask a colleague to notify the physician/nurse practitioner.
Normal bowel sounds are usually the same throughout all four quadrants, but abnormal bowel sounds can vary from quadrant to quadrant. For example, hyperactive bowel sounds can be present prior to the location of a partial bowel obstruction, and hypoactive or absent after the location of a partial bowel obstruction. Trends in bowel sound are important to consider; for example, a sudden shift from hyperactive to absent may indicate a crisis situation such as a bowel perforation.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=674#h5p-44
Palpation of the abdomen provides information about the organs associated with the GI system. The palpation technique follows auscultation, so the abdomen is already exposed. Additionally, you should not palpate the abdomen if vascular bruits are present (e.g., aortic, renal, iliac, and femoral).
Remember, always palpate on bare skin.
Palpation of the abdomen involves the following steps (see Video 5.3):
1. If not already, ask the client to bend their needs up and ensure they are draped.
2. Use the pads of your four fingers to gently palpate the abdomen, keeping your fingers together and your wrist and forearm at about the same plane as the client’s body.
- Avoid a more angled position: this will create a feeling that you are poking the client in the abdominal region, which can be uncomfortable and also does not permit you to assess the area as well.
- Only the pads of your fingers should be touching the client during light palpation.
3. Begin in the right lower quadrant and proceed clockwise. If the client indicates they have pain in the right lower quadrant, begin in the right upper quadrant instead and palpate the area with pain last.
4. Press down about one to two centimeters (light palpation) and move your fingers together in a circular motion.
- Sometimes, you will notice voluntary guarding (tense abdominal muscles) as a result of nervousness, pain, cold room temperature or hands of the nurse, or ticklishness. The tenseness of the muscles usually covers the whole abdomen (i.e., bilateral). It can help to ask the client to take a deep breath when you palpate to help them relax the muscles. Remember to use light palpation and do the painful area last. Only expose the abdomen as long as needed so the client stays warm, and warm your hands by rubbing them together. If the client is ticklish, use a sandwich technique: put their hand on top of your palpating hand, and place your other hand over top of both to control the pressure.
5. Lift fingers up together and move on to the next location, ensuring that you palpate every square centimeter of the abdomen in all four quadrants.
6. Assess the following:
- Overall consistency (soft or firm) and associated pain/tenderness. The abdomen is usually soft upon palpation. Note the location of any firmness and any associated pain/tenderness. The consistency of the abdomen is influenced by the amount of adipose tissue or muscle, but these are symmetrical across the abdomen.
- Presence of masses. Describe any masses in terms of location, size (dimensions), shape, consistency (soft or firm), and associated pain/tenderness.
- Presence of swelling. Note the location of any swelling.
- Presence of pain. If the client feels pain/tenderness upon palpation, note the location and ask them to rate the severity on a scale of 0 to 10.
- Presence of rigidity and spasms. Rigidity is involuntary firmness/hardness of the abdominal muscles associated with peritoneal inflammation. This rigidity is felt over the inflamed area; it is not bilaterally symmetrical and not voluntary like guarding. You may also feel spasms which are muscle contractions that are often painful.
7. Note the findings.
- Normal findings might be documented as: “Abdomen soft to touch with no masses, swelling, pain, and rigidity.”
- Abnormal findings might be documented as: “Client noted generalized pain all over abdomen upon palpation, rating it 5/10. Abdomen firm to touch in all quadrants. Left lower quadrant mass, circular in shape, 5 x 5 cm.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=676#oembed-3
Video 5.3: Palpation of the abdomen
If a client has indicated pain/tenderness, palpate that area last. Palpating a painful area of the abdomen first will aggravate the pain and may affect the accuracy of your assessment.
Urgent surgical intervention is required when a client has appendicitis (inflammation of the appendix that is at risk of perforating). In these cases, client usually presents with an increasing level of pain in the right lower quadrant, often beginning in the periumbilical region. This can also be associated with lack of appetite, nausea, vomiting, fever, chills, and muscle rigidity. If you suspect appendicitis, notify the physician immediately. Continue to monitor the client, measure vital signs, do not allow the client to take anything by mouth, and begin an intravenous if there are standing orders. A physician or nurse practitioner may assess for rebound tenderness, which involves palpating in the right lower quadrant and quickly removing one’s hand. Positive rebound tenderness (pain when the assessor removes their hand) is often indicative of appendicitis.
All abnormal findings (e.g., masses, swelling, pain, rigidity) should be further investigated with a focused abdominal assessment. Report any new, worsening, or unexpected findings to the physician or nurse practitioner.
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=676#h5p-45
Percussion of the abdomen involves tapping the body to elicit sounds and determining whether the sounds are appropriate for the underlying structure of the quadrant. This provides information about the overall consistency of the abdomen as well as the size and borders of some of the underlying structures. For example, percussion sounds of the abdomen can tell you whether the underlying structures are:
- Fluid filled with a mixture of air and contents (e.g., intestines, bladder, stomach).
- Fluid results in a tympanic sound (like a drum, usually high pitched with a long duration). General tympany with scattered dullness is the dominant sound heard over the abdomen because of the intestines.
- Dense (e.g., liver, an abnormal mass close to the surface, intestines filled with stool).
- Density results in a dull sound (like a quiet thud, usually high pitched with a short duration).
Expected percussion notes may be influenced by each body’s unique size and shape. For example, some bodies are more muscular and some have more adipose tissue. The expected percussion sounds are influenced by muscle and adipose tissue, which tends to elicit a more flat sound. You may decide to not percuss an abdomen that is extremely muscular or has a lot of adipose tissue, but percussion may still be of clinical utility in certain situations. For example, when the abdomen is distended and filled with air, the percussion note might resemble hyper-resonance; when the abdomen is filled with fluid such as with ascites the percussion note might have more tympanic noise that is not scattered with dullness, depending on the severity of the ascites.
Percussing the abdomen involves the following steps:
1. Use an indirect percussion technique to percuss the abdomen. As shown in Figure 5.6, this technique involves the application of a mediated force using parts of both hands.
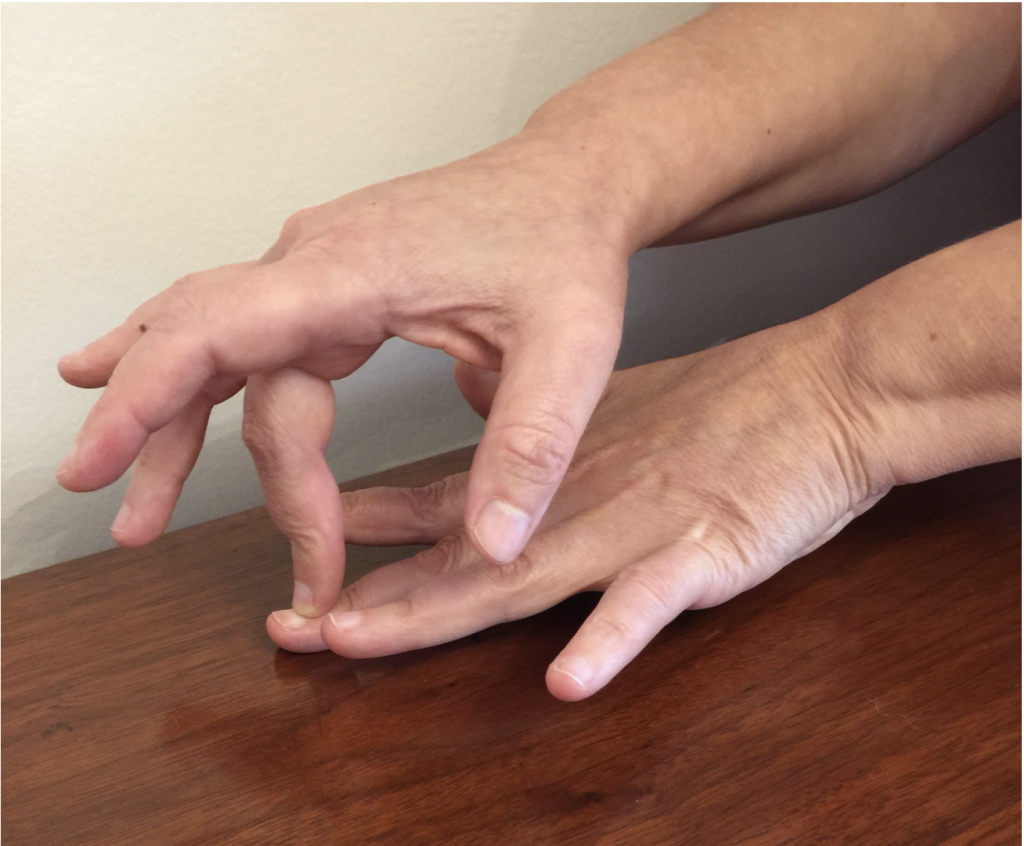
Figure 5.6: Indirect percussion.
2. Perform indirect percussion using a zig-zag pattern (see Figure 5.7) beginning in the right lower quadrant and progressing clockwise. Percuss about three times per quadrant. For indirect percussion (see Video 5.4):
- Non-dominant hand: With your hand parallel to the client’s body, place the distal interphalangeal joint of the pleximeter (middle) finger of your non-dominant hand firmly on the body region to percuss. Because the abdomen is often soft, you must push down relatively firmly with the distal interphalangeal joint. Ensure that only your interphalangeal joint is touching the body (and not the rest of the hand) and that the finger is fully extended.
- Dominant hand: Flex (bend) the pleximeter finger of your dominant hand and with the tip of your finger, tap twice on the distal interphalangeal joint of your non dominant hand. The pleximeter finger of your dominant hand should be at a 90-degree angle to the surface of the client’s body. The motion should be firm and quick with a very short duration. To optimize this motion, the wrist of your non-dominant hand should be relaxed and loose with your forearm parallel to the client’s body.
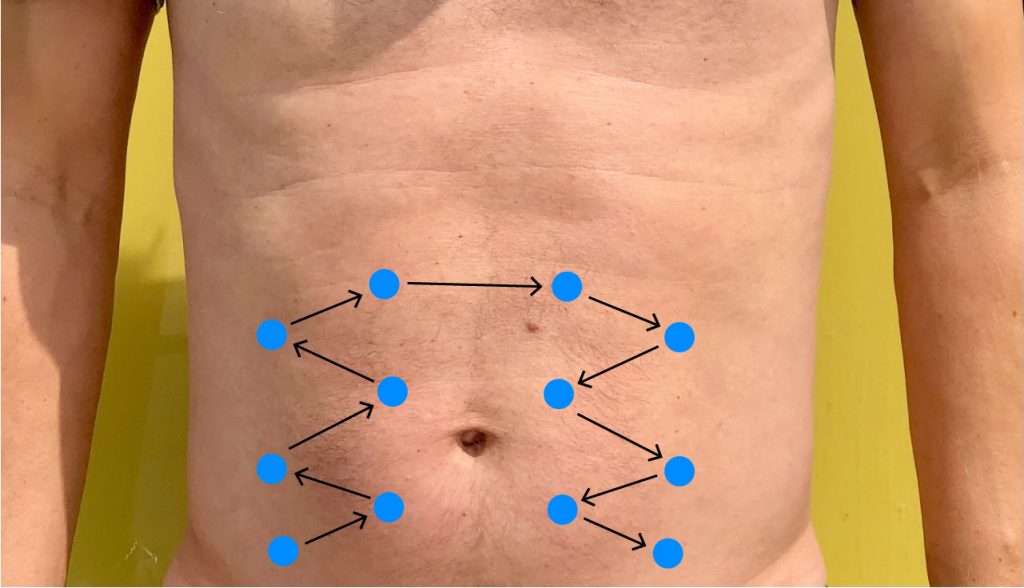
Figure 5.7: Pattern to percuss the abdomen
3. Listen to the quality of the sound and identify the location.
4. Note the findings.
- Normal findings might be documented as: “General tympany with scattered dullness heard in all quadrants. Dullness heard in upper right quadrant over the liver.”
- Abnormal findings might be documented as: “Dullness heard in left lower quadrant with general tympany and scattered dullness in all other quadrants.”
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=678#oembed-3
Film Clip 5.4: Percussing the abdomen
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=678#h5p-46
Perianal Region - Inspection and Palpation
51
The perianal region extends around the anal opening by about five centimetres. Assessment of the perianal region can create feelings of discomfort and nervousness in clients, so you should always employ a trauma-informed approach.
- Explain each step.
- Ask permission to touch.
- Use a drape, and only expose the client as long as needed.
- Avoid words that may be triggering, such as “bed” and “spread your legs.” Instead, use “exam table” and make requests like “move this leg out.”
- Ask the client if they would like to have another person present such as a family member/friend or another healthcare provider.
Positioning for this assessment depends on several factors including age, what is most comfortable for the client, and other parts of the assessment. It is best to use an inclusive approach to assessment: provide the client with options on how to proceed with positioning. Where appropriate, you can provide choices by saying, for example, “I need to exam your anal region. I usually have clients in position XX or XX, do you have a preference or another option?” Specific considerations for positioning include:
- To ensure infants and toddlers are comfortable and safe, involve their caregiver/parent when possible. They are often best positioned in supine position on the exam table or the caregiver’s lap and then the legs (hips and knees) are flexed towards the chest.
- With older children, adolescents, and adults, use a position that is comfortable and familiar for the client. For example, if you are only doing an examination of the perianal region and/or the client is restricted to the bed, you can help the client into a left lateral position. If clients have difficulty maintaining this position, place a pillow between their legs with the right leg flexed.
- A rectal exam is often performed at the same time as genitourinary or prostate exam, so you should use the position required for that to minimize position changes. More importantly, it is important to use a position that is most comfortable for the client and usually gender-affirming. For example, for a cisgender woman, you may use a lithotomy position in which they are in supine position with their legs flexed and abducted, and their feet in stirrups. With a cisgender man, you may use a standing position in which they lean over on a table with toes pointing inward. With transgender and non-binary clients, use a position that is most comfortable for them at that moment: this is usually a position that is gender-affirming. For example, for a transman, you may use a standing position and for a transwoman, you may use a lithotomy position. Be aware that the preferred position may change over time for a non-binary or a trans client, so always ask.
Perianal assessment involves the following steps:
1. Prepare supplies needed (e.g., cover sheet/drape, gloves).
2. Don gloves.
3. Provide options for positioning.
4. Assist the client into position and ensure they are comfortable.
5. Expose the rectal area. If the client is in a left lateral position, place your dominant hand on the right buttock and gently pull it up. If the client is standing, you may need to gently spread the buttocks apart with both of your hands; you may also need to do this if the client is in supine or lithotomy position.
6. Inspect the area for colour. The peri-anal area is slightly darker than the rest of the client’s skin, but the colour in the region should be consistent with no discoloration (e.g., redness, dark brown/purple) or rashes.
7. Inspect the area for lesions or lumps (e.g., a wart).
- If any are noted, palpate them for consistency (soft or hard) and pain.
- If any are noted, identify the location, colour, size, shape, elevation, and whether the area is intact.
8. Inspect the area for discharge. If any is noted, identify the quantity, colour, and consistency.
9. Inspect the area for malformations. (e.g., hemorrhoids). See Figure 5.8 for an image of a hemorrhoid. If any malformations are noted, describe the appearance, location, colour, and size.
- If any are noted, palpate them for consistency (soft or hard) and pain.
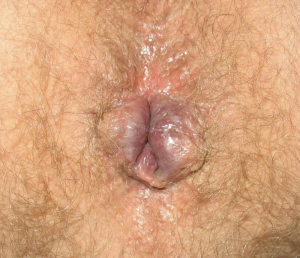
Figure 5.8: Hemorrhoids
Photo by Pachacamac33, Public Domain, from Wikimedia Commons (image was cropped and illustrated upon for the purposes of this chapter)
10. Assess for anal tone by asking the client to try to contract or “draw in” their anus. This can also be achieved by gently touching a cotton ball just lateral from the anus. Observe the external anal sphincter. Normally, a client has “good” anal tone as demonstrated by contraction or puckering of the anus.
- This is important to assess particularly in older clients or clients who may have indicated problems with fecal incontinence. Anal tone can be affected by nerve or muscle damage. There are many causes of this damage, but it is sometimes related to individuals who strain when trying to have a bowel movement. Straining can be associated with constipation and can be treated by health promotion related to diet, sufficient water intake, and routine bowel training.
11. Note the findings.
- Normal findings might be documented as: “Perianal area is consistent in colour with no discolouration, lesions, discharge, or malformations. Good anal tone.”
- Abnormal findings might be documented as: “Perianal area has swollen veins at the anal opening with slight bleeding.”
Activity: Check Your Understanding
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=680#h5p-47
Health Promotion and Disease Prevention: Considerations and Interventions
Health promotion and disease prevention are important components of any assessment, including a GI system assessment. Consider all available subjective and objective data when determining appropriate interventions. As part of subjective data collection, ask the client about risk factors, social determinants, and other considerations.
The inquiry part is integrated throughout the assessment. Many of the probing questions may be asked when doing the subjective assessment. However, some of the questions will be formulated based on your critical reflection of data collected during the subjective and objective assessment. It is this data that will inform your clinical judgment and the health promotion needed for a specific client.
Hand Hygiene
Hand hygiene is necessary to maintain a healthy GI system and prevent unhealthy microorganisms from entering the body. Hand hygiene can decrease the risk of various mouth and other GI-related viruses, such as herpes simplex virus type 1 (e.g., cold sores, fever blisters) and viral gastroenteritis (e.g., stomach flu), parasites on the surfaces of soil, food, and water (e.g., giardia), and bacteria found in the mouth that cause decay (e.g., Streptococcus mutans) or in contaminated food that can cause diarrhea and stomach cramps/pain (e.g., Salmonella).
Probing questions related to hand hygiene include:
- Tell me about when you wash your hands?
- How often do you wash your hands?
- What is involved in washing your hands? (Further probes might include: What are the steps involved? How long do you do it for?)
You may need to educate the client about effective hand hygiene practices such as when to perform it and how to do it. This education should be dependent on the client’s age. For example, you could teach a child to wash their hands along with their favorite song or a fun educational video; with older adults, you could introduce various assistive devices (e.g., nail brush) for clients with limited fine dexterity. Teach clients to perform hand hygiene frequently in healthcare and in work settings, as well as when they arrive at and leave a building, come home, before meal preparation, before and after meals, and before and after using the washroom.
Hand hygiene generally refers to either hand washing with soap and water or hand sanitizing with an alcohol-based hand rub. The mechanical actions of rubbing and creating friction helps to break down and remove various microorganisms from hands, preventing them from entering the mouth and the rest of the GI tract. Clients may require education about specific techniques.
Hand washing technique:
- Rinse hands with warm water, lather with soap for 20 seconds.
- Rinse hands with water.
- Dry hands with a paper towel.
- Turn off the tap with your elbow or the paper towel.
NOTE: Consider how to make it fun with children, for example by singing a song that lasts 20 seconds.
Hand sanitizing technique with alcohol-based hand rub:
- Ensure hands have no soil on them and are visibly clean.
- If there is visible soil, perform hand washing instead.
- Dispense a sufficient amount of gel in hand.
- Rub hands together so that all areas of the hands are covered.
- Rub hands together for about 15 seconds until they are dry.
- If hands dry before 15 seconds, use more hand gel.
Mouth Care and Dental Care
Mouth and dental care is an important part of maintaining the health of the oral cavity of the GI system, particularly the teeth and gums.
Probing questions related to mouth care and dental care include:
- Tell me about any personal mouth and dental care you perform. Probing questions could include:
- How often do you brush your teeth?
- How often do you floss?
- Can you tell me about your brushing technique (e.g., brushing away from gums, type of toothbrush)?
- When was the last time you saw a dentist for a check-up or a hygienist for a dental cleaning? How often do you typically have your teeth cleaned?
- Do you have any concerns about your mouth and dental care?
Begin by addressing any of the client’s concerns about their mouth and dental care. Remember to consider relational and structural approaches to health promotion. For example, children learn how to brush their teeth and maintain a schedule based on support from their parent/caregiver. Thus, it is important that you assess social and familial support related to dental care. Based on your assessment and the client’s needs, you may need to provide health promotion education about mouth and dental care.
The Canadian Dental Association (2021) recommends brushing teeth at least twice a day, flossing once a day, and having a cleaning about every six months. However, there are many inequities associated with dental care, for example geographical access to a dentist when living in rural, remote, and Northern communities. Some communities lack access to clean water, and some water systems are not fluoridated. Almost 30% of the water systems in Ontario are not fluoridated, and this has a significant effect on dental decay. The lack of fluoridated water systems has been identified as a problem for many Indigenous communities (Public Health Agency of Canada, 2017).
Another consideration is the financial costs associated with dental cleanings and dentist appointments. These are not always covered under provincial and territorial health insurance plans in Canada. Ask the client if they are covered under a private insurance plan related to their work or under a family member’s plan or through their post-secondary educational institution. Ontario has a dental care program for children under the age of 17 from low-income families (https://www.ontario.ca/page/get-dental-care) and low-income seniors (65 and older; http://www.cda-adc.ca/en/oral_health/cfyt/dental_care_seniors/flossing_brushing.asp). Some dental schools also provide dental care at minimal cost.
Diet
Diet affects the functioning of the GI system. A healthy diet helps maintain the health of the GI system, fuels the body to function, and maintains an ideal body mass index; a diet high in fibre with adequate hydration helps keep the intestines moving and bowel movements regular. In contrast, an unhealthy diet can lead to malnutrition, obesity, dental decay, altered bowel patterns such as constipation and diarrhea, and can affect other body systems and lead to various health problems such as diabetes, some cancers, cirrhosis, and heart disease.
Check out this video about how the food you eat affects your gut. It was created by Dr. Shilpa Ravella, a gastroenterologist.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=682#oembed-5
https://youtu.be/1sISguPDlhY
Probing questions related to diet could include:
- Tell me about your usual diet?
- What have you eaten in the last 24 hours? Is that your usual diet?
- Do you have any food allergies or intolerances? (Further probes could include: What type of allergies? What is the reaction? (e.g., anaphylaxis, rash) When did the allergy start? How do you treat it?)
- Do you have enough money to buy healthy food?
- Tell me about your cultural practices related to diet?
You could assess the client’s familiarity with Health Canada’s Food Guide (Government of Canada, 2021) and discuss how they might draw upon it to guide their food choices: https://food-guide.canada.ca/en/. Remember that the food guide still includes Eurocentric elements, so you should collaborate with the client about its relevance in the context of their cultural food practices. A snapshot of the food guide is now offered in dozens of languages: https://www.canada.ca/en/health-canada/services/canada-food-guide/resources/snapshot/languages.html and many resources have been developed for Indigenous populations:
https://www.sac-isc.gc.ca/eng/1581522106156/1581522147811.
Informed by Canada’s Food Guide, some key elements to discuss with a client when promoting a healthy diet include:
- Eating patterns and cultural practices.
- Making water the drink of choice.
- Making time to enjoy the meal, eating mindfully, allowing the food to digest.
- How to incorporate fibre, probiotics, fermented foods (e.g., kimchi), polyphenols (e.g., almonds), and a variety of food options to promote gut healthy nutrients.
Assess each client’s lifestyle to understand how it affects their diet and how you can help them adapt to include healthier food choices when possible. Use the relational health promotion approach to learn what food and diet means to the client and how their environment and the people within it can influence their choices. For example, young adults attending college or university may have limited access to healthy food choices due to a prevalence of fast food vendors at their institution. In this sort of situation, when a client lacks access to healthy food resources, nurses can source out and advocate for access to food resources within the client’s community (e.g., food banks, breakfast programs), help the client find accessible food services (e.g., student nutrition program), or help the client find resources for grocery delivery. Nurses need to advocate to ensure the particular needs of each client are being met, using the available socioeconomic and environmental resources. By working in partnership with each client, you can create effective interventions that support the client in achieving a healthy diet.
Smoking, Alcohol, and Cannabis
Smoking or chewing tobacco has negative effects due to the risk of cancer in the mouth, tongue, esophageal, stomach, pancreas, and liver. Alcohol and cannabis can have positive and negative effects on the GI system.
For example, red wine contains polyphenols from the skins of the red grapes. Polyphenols are plant-based compounds that are healthy for intestinal bacteria; evidence suggests that polyphenols have a probiotic effect on intestinal bacteria (Moorthy et al., 2020). However, this is not a good reason to start drinking wine, because many plant-based foods such as fruits contain polyphenols. Moreover, alcohol can have negative effects on your GI tract: it can cause diarrhea in some due to increased acid production in the intestines, and constipation in others due to its diuretic effect. Some people are also intolerant to the additives in alcohol (e.g., gluten in beer). The liver is the main organ that processes alcohol, and heavy drinking over a long period can damage the liver and lead to cirrhosis. Additionally, because the liver processes many medications, a damaged liver can affect how medications are absorbed and their effects. The most recent Canadian guidelines now suggest that there are health risks associated with any level of alcohol consumption, although negligible with two drinks or less weekly (Paradis et al., 2022). From a GI perspective, alcohol is a carcinogen that is linked to colon cancer as well as rectum, mouth, liver, and esophageal cancer (Paradis et al., 2022). Overall, the key is to consume limited amounts of alcohol.
The Canadian Society of Intestinal Research has reported that cannabis can be used effectively to treat loss of appetite and nausea and vomiting related to GI conditions such as irritable bowel diseases (IBD) and multiple sclerosis (MS) (https://badgut.org/information-centre/a-z-digestive-topics/cannabis/). However, negative GI-related effects of consuming cannabis have also been reported: some individuals are allergic, and long-term use can cause cannabinoid hyperemesis syndrome, which causes nausea, vomiting, and abdominal pain. Overall, clients should discuss cannabis use with their primary healthcare provider prior to consuming.
Probing questions related to alcohol, cannabis, and smoking could include:
- Tell me about how much alcohol you consume in a day? If the client does not consume alcohol daily, you can assess consumption based on weekly, monthly, or none. If the client’s answer is affirmative, ask probing questions such as: How much (e.g., ounces a day)? What type of alcohol (e.g., red wine, beer)? For how long? Can you tell me the reasons?
- Do you smoke or ingest cannabis? If affirmative, ask similar probing questions as above. Also ask if it is medically prescribed or recreational.
- Do you smoke cigarettes or use any tobacco-related products? If affirmative, ask similar probing questions as above examples. Also ask if the client inhales or chews tobacco.
- If you do not currently consume alcohol/cannabis/smoking, have you ever? If affirmative, you can ask similar probing questions as above, including the reason that the client quit.
- Have you had an allergic reaction to alcohol or cannabis? If affirmative, ask probing questions such as: What is the reaction (e.g., anaphylaxis, irritable bowel)? When did it start? How do you treat it?
Health promotion education should focus on each client’s lifestyle and reasons for consuming alcohol, cannabis, or tobacco. Interventions related to using safely or quitting the consumption should be tailored to each client and could include counselling, cognitive-behavioural therapy, and support groups. You should also consider the relational promotion approach: for example, a client’s consumption can be influenced by their surrounding environment (e.g., family, friends, workplace).
If the client is interested in using medical cannabis, your role as a nurse is to understand their interest and help them find appropriate resources specific to their needs. You can also advocate for educational resources about medical cannabis if a client’s healthcare setting or community lacks resources or support.
Activity
Activity and exercise promote peristalsis of the intestines ensuring that content moves along the digestive tract and helps to maintain a healthy body mass index. It is important for individuals to eat healthy and drink an adequate amount of fluids (primarily water) based on their age, genetics, and activity level. Guidelines vary, but it is suggested that individuals participate in about 30 to 60 minutes of aerobic activity five to seven times per week.
Check out this video about improving digestion with movement. It was created by Dr. Jaclyn Tolentino, a family medicine physician.
One or more interactive elements has been excluded from this version of the text. You can view them online here: https://pressbooks.library.torontomu.ca/assessmentnursing/?p=682#oembed-6
https://youtu.be/miIEBjULTuQ
Probing questions related to activity could include:
- Tell me about your activity or exercise routine?
- What is your exercise routine? What type of exercise? How long do you do this type of exercise for? How many days of the week do you participate in exercise? If the client engages in sports, ask about protective equipment.
- Do you have any mobility limitations?
- Do you have any concerns about your level of activity or exercise?
- Do you have any goals you would like to achieve related to your activity or exercise level?
Assess and collaborate with each client to create an activity/exercise care plan that is based on their goals and needs. The care plan should be realistic and attainable for the client according to their physical capabilities, environment, and availability. You can also assess the client’s access to support systems for additional support, such as community walking groups, fitness apps, and local gym memberships. The participACTION website is a helpful resource: https://www.participaction.com/en-ca.
Remember to assess the client’s broader community structures. For example, does the client’s community have accessible, safe sidewalks or streetlights. This kind of structural approach to health promotion can help address potential inequities. Access to services can vary and can be a barrier to the client’s exercise/activity goals. Other barriers might include finances (e.g., gym memberships, sports registration fees) or geographical location (e.g., different resources available in urban, rural or remote regions). As a nurse, you will need to tailor activity programming to each client. You can also advocate for structures to address inequities.
References
Canadian Dental Association (2021). Flossing and brushing. http://www.cda-adc.ca/en/oral_health/cfyt/dental_care_seniors/flossing_brushing.asp
Paradis, C., Butt, P., Shield, K., Poole, N., Wells, S., Naimi, T., Sherk, A., & the Low-Risk Alcohol Drinking Guidelines Scientific Expert Panels. (2022). Update of Canada’s Low-Risk Alcohol Drinking Guidelines: Final Report for Public Consultation. Ottawa, Ont.: Canadian Centre on Substance Use and Addiction.
Public Health Agency of Canada (2017). The state of community water fluoridation across Canada. https://www.canada.ca/en/services/health/publications/healthy-living/community-water-fluoridation-across-canada-2017.html
Clinical Judgment - Case Study
A 67-year-old client, pronouns she/her, came to the health clinic concerned about being constipated for the last 2 ½ weeks and has been experiencing cramping and pain in her left lower quadrant (LLQ) for the past 4 days. She reported feeling like she has to have a bowel movement (BM) but nothing comes out and she is worried she might have hemorrhoids. Today she began to feel nauseous. The client explained she was diagnosed with multiple sclerosis (MS) 5 years ago and that when she is stressed, her MS flares up and she gets constipated. Her daily life routine has been altered recently because she has been taking care of a friend who had heart surgery. Her vital signs are: blood pressure (BP) 138/88 mm Hg, pulse (P) 92 beats per minute, respirations (RR) 18 breaths per minute, oxygen saturation (O2 sats) 98% and oral temperature (T) 37.9 degrees Celsius.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=684#h5p-48
The nurse learns the client experiences these symptoms a couple of times per year when her MS flares-up. When not having a flare-up, the client normally has a bowel movement 5–6 times per week. The client reported that her diet and exercise has been interrupted due to helping a friend. She said that she usually eats a healthy diet, walks 30–60 minutes 5 times per week, and does yoga 3 times per week. During the last 2 weeks, she has not exercised and has been ordering take-out. Other symptoms include straining when having a bowel movement, passing small hard stool, and a bit of bleeding during the last bowel movement. The client’s constipation usually resolves after a week, but she believes it has lasted longer due to the added stress in her life.
An interactive H5P element has been excluded from this version of the text. You can view it online here:
https://pressbooks.library.torontomu.ca/assessmentnursing/?p=684#h5p-49
- Common symptoms to assess related to the GI system include pain, nausea and vomiting, appetite changes, food intolerances and allergies, changes to bowel patterns including diarrhea and constipation, bloating, and flatulence.
- An objective assessment of the GI system is first performed with the client sitting upright to assess the oral cavity and then lying supine to assess the abdomen. Collaborate with the client to determine the position to best assess the perianal region.
- A trauma-informed approach to the objective assessment is necessary considering that areas of the abdomen and the perianal region are being exposed.
- The objective assessment should begin with inspection and palpation related to the oral cavity; inspection, auscultation, palpation, and percussion of the abdomen; and inspection and palpation of the perianal region.
- Health promotion interventions should be developed with the client to address what is important to them.











































