Chapter 5 – Gastrointestinal System Assessment
Perianal Region – Inspection and Palpation
The perianal region extends around the anal opening by about five centimetres. Assessment of the perianal region can create feelings of discomfort and nervousness in clients, so you should always employ a trauma-informed approach.
- Explain each step.
- Ask permission to touch.
- Use a drape, and only expose the client as long as needed.
- Avoid words that may be triggering, such as “bed” and “spread your legs.” Instead, use “exam table” and make requests like “move this leg out.”
- Ask the client if they would like to have another person present such as a family member/friend or another healthcare provider.
Positioning for this assessment depends on several factors including age, what is most comfortable for the client, and other parts of the assessment. It is best to use an inclusive approach to assessment: provide the client with options on how to proceed with positioning. Where appropriate, you can provide choices by saying, for example, “I need to exam your anal region. I usually have clients in position XX or XX, do you have a preference or another option?” Specific considerations for positioning include:
- To ensure infants and toddlers are comfortable and safe, involve their caregiver/parent when possible. They are often best positioned in supine position on the exam table or the caregiver’s lap and then the legs (hips and knees) are flexed towards the chest.
- With older children, adolescents, and adults, use a position that is comfortable and familiar for the client. For example, if you are only doing an examination of the perianal region and/or the client is restricted to the bed, you can help the client into a left lateral position. If clients have difficulty maintaining this position, place a pillow between their legs with the right leg flexed.
- A rectal exam is often performed at the same time as genitourinary or prostate exam, so you should use the position required for that to minimize position changes. More importantly, it is important to use a position that is most comfortable for the client and usually gender-affirming. For example, for a woman, you may use a lithotomy position in which they are in supine position with their legs flexed and abducted, and their feet in stirrups. With a cisgender man, you may use a standing position in which they lean over on a table with toes pointing inward. With and clients, use a position that is most comfortable for them at that moment: this is usually a position that is gender-affirming. For example, for a transman, you may use a standing position and for a transwoman, you may use a lithotomy position. Be aware that the preferred position may change over time for a non-binary or a trans client, so always ask.
Perianal assessment involves the following steps:
1. Prepare supplies needed (e.g., cover sheet/drape, gloves).
2. Don gloves.
3. Provide options for positioning.
4. Assist the client into position and ensure they are comfortable.
5. Expose the rectal area. If the client is in a left lateral position, place your dominant hand on the right buttock and gently pull it up. If the client is standing, you may need to gently spread the buttocks apart with both of your hands; you may also need to do this if the client is in supine or lithotomy position.
6. Inspect the area for colour. The peri-anal area is slightly darker than the rest of the client’s skin, but the colour in the region should be consistent with no discoloration (e.g., redness, dark brown/purple) or rashes.
7. Inspect the area for lesions or lumps (e.g., a wart).
- If any are noted, palpate them for consistency (soft or hard) and pain.
- If any are noted, identify the location, colour, size, shape, elevation, and whether the area is intact.
8. Inspect the area for discharge. If any is noted, identify the quantity, colour, and consistency.
9. Inspect the area for malformations. (e.g., hemorrhoids). See Figure 5.8 for an image of a hemorrhoid. If any malformations are noted, describe the appearance, location, colour, and size.
- If any are noted, palpate them for consistency (soft or hard) and pain.
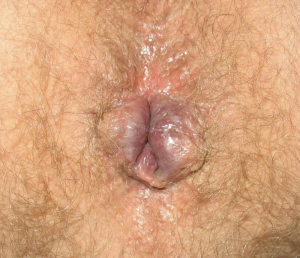
Figure 5.8: Hemorrhoids
Photo by Pachacamac33, Public Domain, from Wikimedia Commons (image was cropped and illustrated upon for the purposes of this chapter)
10. Assess for anal tone by asking the client to try to contract or “draw in” their anus. This can also be achieved by gently touching a cotton ball just lateral from the anus. Observe the external anal sphincter. Normally, a client has “good” anal tone as demonstrated by contraction or puckering of the anus.
- This is important to assess particularly in older clients or clients who may have indicated problems with . Anal tone can be affected by nerve or muscle damage. There are many causes of this damage, but it is sometimes related to individuals who strain when trying to have a bowel movement. Straining can be associated with constipation and can be treated by health promotion related to diet, sufficient water intake, and routine bowel training.
11. Note the findings.
- Normal findings might be documented as: “Perianal area is consistent in colour with no discolouration, lesions, discharge, or malformations. Good anal tone.”
- Abnormal findings might be documented as: “Perianal area has swollen veins at the anal opening with slight bleeding.”
Activity: Check Your Understanding
refers to person whose gender identity aligns with their sex at birth
refers to a person whose gender identity incongruent with their sex at birth.
refers to people who feel their gender cannot be defined based on the gender binary.
is the involuntary release of stool.

