Peripheral Vascular System Assessment
Objective Assessment
An objective assessment is usually completed after the subjective assessment, unless symptoms require urgent interventions.
An objective assessment of the peripheral vascular system (PVS) includes:
- Inspection and palpation of hands and arms.
- Inspection and auscultation of abdominal vasculature areas.
- Inspection and palpation of feet and legs.
All assessments should be performed on bare skin. You will need a penlight and a stethoscope.
Be aware of the environmental temperature in the room and the temperature of your hands. Room temperatures are not easily modified, so you should only expose the body part(s) you are assessing. Try to warm your hands before placing them on the client’s body. Don gloves if you observe skin that is not intact.
Ensure the client is positioned in the best way to assess the arms, abdomen, and legs. You will usually begin with the client seated on the side of the exam table with legs or feet dangling or in the high-Fowler’s position. If you are assessing a young child or newborn, you could ask someone (e.g., care partner, healthcare provider, parent) to hold them on their lap or on the exam table.
When assessing the PVS, you will usually assess arterial and venous sufficiency. Your findings from the objective assessment, along with those from the subjective assessment, will provide cues about whether any issues are arterial or venous related. Recall Table 3 from the Subjective Assessment section.
Clinical Tips
Trauma-informed approach: Always use a . This is particularly important considering that areas of the abdomen and legs will be exposed. Don’t assume who may have experienced trauma: it can happen to anyone, regardless of gender, age, or socioeconomic/educational level. Trauma is also subjective and personal to each individual; trauma for one person might not be trauma for another.
You could start by asking the client if they would like a family member or friend or another healthcare provider present. Always maintain privacy by closing the door and/or curtains and using draping. Ask permission to touch and explain what you are going to do so the client knows what to expect. If relevant, ask permission to touch any mobility aids and prosthetics; the client may view these as an extension of their body and part of their self-identity.
What if pulses are not palpable? If a pulse is not palpable in the distal most aspect of the limb, you should assess the next proximal pulse (or medial). For example, if you can’t feel a radial pulse, you might assess the brachial or ulnar pulses. It can also be helpful to use a Doppler ultrasound device (often just referred to a doppler) when you are struggling to feel a pulse and are concerned about perfusion into the limbs. This is a handheld device that allows you to hear the whooshing sound of the pulsatile blood flow. See Figure 8 and Video 2 for use of a Doppler device.
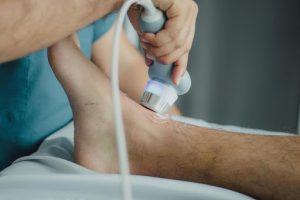
Figure 8: Doppler ultrasound device. (Photo by Juan Manuel Montejano Lopez on Pexel.)
Video 2: Use of a Doppler ultrasound device [1:51]
Contextualizing Inclusivity
Objective assessment involves assessing skin discolouration. Two common kinds of skin discolouration related to peripheral vascular assessment are cyanosis and pallor.
- Cyanosis involves an increase in deoxygenated hemoglobin in the blood (hypoxemia). Reduced oxygen makes blood a darker red colour. When this blood is circulated to the limbs, the tissues receive inadequate oxygen (hypoxia) and as result the skin becomes dull in colour and the skin and nail beds change in colour. The skin can become a variation of blue/purple and grey/green shades. In people with dark skin, cyanosis appears as a dark purple and sometimes a grey colour, but it is difficult to see with early cyanosis. People with yellowish tones to their skin can have a greyish/green shade (Lewis, 2020; Sommers, 2011), and people with lighter skin tones tend to develop a dusky bluish/purple shade (Lewis, 2020). Acrocyanosis is cyanosis that happens in the extremities (feet and hands). Newborns can be born with acrocyanosis, but it should disappear after a couple of hours and should be monitored.
- Pallor occurs when there is decreased perfusion to the limbs. In clients with darker skin, it is best assessed on the palms of the hands and the nail bed, as these areas are already paler in colour; with pallor, these areas become paler than the client’s normal skin colour (Lewis, 2020). This is also true for clients with lighter skin colour, but with these clients you will also observe paler toes and feet. In people with lighter brown skin, you might observe pallor as a yellowish shade (Lewis, 2020).
References
Lewis, G. (2020). Identifying AEFI in diverse skin colour. https://mvec.mcri.edu.au/references/identifying-aefi-in-diverse-skin-colour/
Mukwende, M., Tamony, P., & Turner, M. (n.d.). Mind the gap: A handbook of clinical signs in black and brown people. (1st edition). https://litfl.com/wp-content/uploads/2020/09/Mind-the-Gap-A-handbook-of-clinical-signs-in-Black-and-Brown-skin.-first-edition-2020.pdf
Sommers, M. (2011). Color awareness: A must for patient assessment. American Nurse. https://www.myamericannurse.com/color-awareness-a-must-for-patient-assessment/
involves integrating an understanding of the need for physical and emotional safety; choice and control; and empowerment (Trauma-Informed Practice Guide, 2013, p. 12).

