Parenteral Nutrition
Welcome to the Parenteral Nutrition section! Throughout this section, an inpatient case study will be used to enhance your learning and comprehension of parenteral nutrition. You will learn what information to gather for your assessment, how to interpret that data to form a nutrition care plan, how to implement your patient’s care plan, and what to look for when following-up and evaluating your plan. As you progress through the content, please keep in mind that the nutrition care process model used here is dynamic and not a linear, step-by-step process. The case study used here is an example, and not all cases will follow the same path.
Learning Outcomes
By the end of the section you will be able to:
- Identify indications, contradictions, and routes of support to determine the requirement for parenteral nutrition.
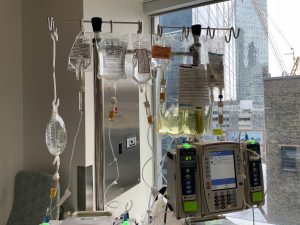
- Identify the routes, sites of delivery, and delivery methods of parenteral nutrition.
- Identify how to gather clinical, anthropometric, biochemical, and dietary data necessary to complete a parenteral nutrition assessment.
- Determine a patients energy, protein, and fluid needs using data from the initial assessment.
- Interpret biochemical values, including sodium, potassium, phosphorous, calcium, magnesium, albumin, BUN/urea, and creatinine.
- Identify the role of a total parenteral nutrition (TPN) team or the interdisciplinary team.
-
Choose an appropriate parenteral nutrition formulation and plan for a patient.
-
Identify a patient a risk of refeeding syndrome and implement procedures to prevent it.
-
Identify the complications of parenteral nutrition and understand the appropriate management procedures.
-
Understand the key factors in appropriately monitoring the parenteral nutrition care plan.
-
Evaluate the nutrition care plan using assessment data relevant to the patients concerns, including malnutrition, symptom management, parenteral nutrition changes, medications, supplements, and the medical plan.
Original Publication: 2021
Last Revised: August 2025

